Acute Painful Horner Syndrome as the First Presenting Sign of Carotid Artery Dissection
Background: Horner syndrome is a rare neurologic disorder that can arise from severe neurologic and systemic conditions, which may require immediate diagnosis with radiologic imaging and treatment with antiplatelet and anticoagulant therapy. Horner syndrome is often asymptomatic but can have distinct, easily identified characteristics seen with an ophthalmic examination.
Case Presentation: A 61-year-old woman presented with periorbital pain localized around and behind the right eye that she rated as 7 on a 10-point scale with onset 3 days prior. She reported light sensitivity, syncope, dizziness, and a recent history of transient ischemic attacks of unknown etiology. The patient had acute, slight ptosis with pathologic miosis and pain in the ipsilateral eye with no reports of exposure to miotic pharmaceutical agents and no history of trauma to the globe or orbit eliminated other differentials, leading to a diagnosis of right-sided Horner syndrome. She was referred for emergency department evaluation where radiography was indicative of an internal carotid artery dissection.
Conclusions: Due to possible life-threatening complications that can arise in patients with Horner syndrome, clinicians must have a thorough understanding of the condition, appropriate treatment, and management modalities. Determining the underlying etiology of Horner syndrome can help prevent a decrease in a patient’s vision or quality of life and in some cases prevent death. Magnetic resonance imaging and computed tomography should be used to rule out carotid artery dissection and other severe conditions.
Symptoms and signs. Patients with Horner syndrome can present with a variety of symptoms and signs. Patients may be largely asymptomatic or they may complain of a droopy eyelid and blurry vision. The full Horner syndrome triad consists of ipsilateral miosis, anhidrosis of the face, and mild ptosis of the upper eyelid with reverse ptosis of the lower eyelid.8 The difference in pupil size is greatest 4 to 5 seconds after switching from bright to dim room illumination due to dilation lag in the miotic pupil from poor innervation.1
Although the classical triad of ptosis, miosis, and anhidrosis is emphasized in the literature, the full triad may not always be present.4 This variation is due to the anatomy of the oculosympathetic pathway with branches of the nerve system separating at the superior cervical ganglion and following different pathways along the internal and external carotid arteries, resulting in anhidrosis only in Horner syndrome caused by lesions to the first- or second-order neurons.4,5 Because of this deviation of the nerve fibers in the pathway, the presence of miosis and a slight ptosis in the absence of anhidrosis should still strongly suggest Horner syndrome.
In addition to the classic triad, Horner syndrome can present with other ophthalmic findings, including conjunctival injection, changes in accommodation, and a small decrease in intraocular pressure usually by no more than 1 to 2 mm Hg.4 Congenital Horner syndrome is unique in that it can result in iris heterochromia, with the lighter eye being the affected eye.4
Due to the long and circuitous nature of the oculosympathetic pathway, damage can occur due to a wide variety of conditions (Table) and can present with many neurologic findings.7
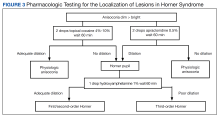
Localization of lesions. In Horner syndrome, 13% of lesions were present at first-order neurons, 44% at second-order neurons, and 43% at third-order neurons.7 While all these lesions have similar clinical presentations that can be difficult to differentiate, localization of the lesion within the oculosympathetic pathway is important to determine the underlying cause. This determination can be readily achieved in office with pharmacologic pupil testing (Figure 3).