VA-Based Peritoneal Dialysis Program Feasibility Considerations and Process Outline
Background: Home dialysis utilization is lower among veterans than in the general US population. Several sociodemographic factors and comorbidities contribute to peritoneal dialysis (PD) underutilization. In 2019, the Veterans Health Administration (VHA) Kidney Disease Program Office convened a PD workgroup to address this concern.
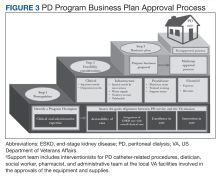
Observations: The PD workgroup was explicitly concerned by the limited availability of PD within the VHA, which frequently requires veterans to transition kidney disease care from US Department of Veterans Affairs medical centers (VAMCs) to non-VHA facilities when they progress from chronic kidney disease to end-stage kidney disease, causing fragmentation of care. Since the administrative requirements and infrastructure of VAMCs vary, the workgroup focused its deliberations on synthesizing a standard process for evaluating the feasibility and establishing a new PD program within any individual VAMC. A 3-phased approach was envisioned, beginning with ascertainment of prerequisites, leading to an examination of the clinical and financial feasibility through the process of data gathering and synthesis, culminating in a business plan that translates the previous 2 steps into an administrative document necessary for obtaining VHA approvals.
Conclusions: VAMCs can use the guide presented here to improve therapeutic options for veterans with kidney failure by establishing a new or restructured PD program.
Compared with hemodialysis (HD), peritoneal dialysis (PD) offers comparable survival and superior patient-centered and health services outcomes.1,2 This has prompted repeated calls over the past 2 decades for policies to increase the use of home dialysis and, more specifically, for PD in the United States.3,4
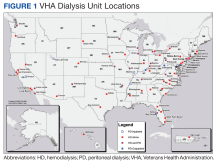
Veterans comprise nearly 10% of the population with end-stage kidney disease (ESKD) burden; > 50,000 US veterans are currently on dialysis.5,6 A majority of these veterans receive their chronic kidney disease (CKD) care through their affiliated US Department of Veterans Affairs (VA) medical centers (VAMCs).
To address these needs, the VHA National Kidney Disease Program (NKDP) formed a 4-member PD workgroup in 2019. Considering the breadth of challenges involved, the PD workgroup broadly designed its approach based on the I CARE (Integrity, Commitment, Advocacy, Respect, and Excellence) VA Core Values.
This review focuses on the initial deliberations of the PD access subgroup and provides a guide to establishing a new local VA PD program.