Evaluation of the Appropriateness of Aspirin Therapy in a Veteran Population
Background: Aspirin is commonly used for primary and secondary prevention of atherosclerotic cardiovascular disease (ASCVD) but may cause more harm than benefit. This study aimed to assess the percentage of patients who were inappropriately prescribed aspirin in the veteran patient population and to assess safety outcomes associated with inappropriate aspirin use.
Methods: Retrospective chart reviews were conducted on up to 200 patients with active prescriptions for 81-mg aspirin tablets filled between October 1, 2019, and September 30, 2021, at the Captain James A. Lovell Federal Health Care Center in Illinois. The primary endpoint was the percentage of patients inappropriately on aspirin therapy and whether these patients were being followed by a clinical pharmacy practitioner. Each patient record was reviewed to determine the appropriateness of aspirin therapy by assessing the indication for use. Safety data were collected for patients who were deemed to be using aspirin inappropriately, including documentation of any major or minor bleeding events.
Results: A total of 105 patients were included in this study. For the primary endpoint, 31 patients (30%) had a possible ASCVD risk and were taking aspirin for primary prevention, while 21 patients (20%) had no ASCVD and were taking aspirin for primary prevention. For the secondary endpoint, 25 patients were aged > 70 years, 15 patients were concurrently taking medications that might increase bleeding risk, and 11 patients had chronic kidney disease. Looking at the entire study patient population, for the safety endpoint, 6 patients (6%) experienced a major bleeding event while on aspirin, and 46 (44%) experienced a minor bleeding event while on aspirin.
Conclusions: Common factors seen in this study to warrant deprescribing aspirin for primary prevention included individuals aged > 70 years, concurrent use of medications that increase bleeding risk, and patients with chronic kidney disease. By assessing ASCVD and bleeding risks and having a risk/benefit discussion with patients and prescribers, aspirin used for primary prevention can be appropriately deprescribed when the risks of bleeding outweigh the benefits.
For the primary endpoint, 53 patients (50%) were on aspirin for secondary prevention and 52 (50%) were on aspirin for primary prevention. Of the 105 patients included in the study, 31 (30%) had a possible ASCVD risk and were taking aspirin for primary prevention, while 21 (20%) had no ASCVD and were taking aspirin for primary prevention. Of the 52 patients on aspirin for primary prevention, 31 patients (60%) had a possible risk for ASCVD. Of the 52 patients in the primary prevention group, 15 (29%) were followed by a pharmacist, and the average number of follow-up appointments was 4.
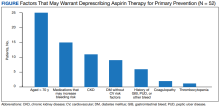
The secondary endpoint focused on patients taking aspirin for primary prevention and the factors that may warrant deprescribing aspirin. Of the 52 patients on aspirin for primary prevention, 25 patients were aged > 70 years, 15 patients were concurrently taking medications that may increase bleeding risk,
For the entire study group, 6 patients (6%) experienced a major bleeding event while on aspirin, 46 (44%) experienced a minor bleeding event while on aspirin, and 53 (50%) experienced no bleeding events while on aspirin. Of the 6 patients who experienced major bleeding events, 4 were on aspirin for secondary prevention, and 2 were on aspirin for primary prevention with ASCVD risk factors. The major bleeding events included 4 gastrointestinal bleeds, 1 intracranial hemorrhage, and 1 hemorrhagic stroke. Of the 46 who experienced minor bleeding events, 20 patients were on aspirin for primary prevention; 11 of those patients had possible ASCVD risk factors and 9 had no documented ASCVD. The minor bleeding events included hematuria, epistaxis, bleeding scabs, and dental bleeding.
Discussion
The majority of patients in this study were on aspirin appropriately. Indications deemed appropriate for aspirin therapy include secondary prevention and primary prevention with a possible ASCVD risk. About 20% of the total patient population in this study was taking aspirin for primary prevention with no ASCVD risk. For these patients, the risk of bleeding likely outweighs the benefits of aspirin therapy as patients are at low risk for ASCVD; therefore, aspirin therapy is likely inappropriate in this patient population. These patients may be unnecessarily at an increased risk for bleeding and may benefit from deprescribing aspirin. For the safety of patients, HCPs should be continuously assessing the appropriateness of aspirin for primary prevention and deprescribing when necessary.
About one-third of the patients using aspirin for primary prevention were followed by a pharmacist. Pharmacists can play a key role in deprescribing aspirin for primary prevention when aspirin use is deemed inappropriate. About 30% of the total patient population in this study was on aspirin for primary prevention with possible ASCVD risk. This patient population may benefit from aspirin therapy as they are at a higher risk for ASCVD. For these patients, a risk/benefit discussion is necessary to determine the appropriateness of aspirin for primary prevention. This risk/benefit discussion should be a continuous conversation between patients and HCPs as different factors such as age and changes in comorbid conditions and medications may increase bleeding risk.
The secondary endpoint focused on patients taking aspirin for primary prevention and the factors that may warrant deprescribing aspirin. The most common factors seen in this study included patients who were aged > 70 years, patients who were concurrently taking medications that may increase bleeding risk, and patients with CKD. All of these factors increase bleeding risk, making the risks potentially outweigh the benefits of aspirin for primary prevention. These factors should be the primary focus when assessing patients on aspirin for primary prevention to promote deprescribing aspirin if deemed appropriate as they were the most prevalent in this study.
The safety endpoints focused on bleeding events as a whole as well as the bleeding events seen in the primary prevention group. There were 2 major bleeding events and 20 minor bleeding events in the primary prevention group. The number of bleeding events both major and minor further shows the need for a continuous risk/benefit discussion between patients and HCPs on continued aspirin use for primary prevention. The bleeding risk with aspirin is prevalent. HCPs should continue to assess for factors that increase the bleeding risk that may warrant deprescribing aspirin to prevent future bleeding events in this patient population.