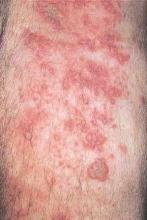
Second dose of herpes zoster vaccine beneficial to seniors
FROM THE JOURNAL OF INFECTIOUS DISEASES
The herpes zoster vaccine should be administered earlier rather than later in order to achieve optimal immune response, but an additional booster shot for individuals 70 years or older is also advisable.
This is according to a recent study published in the Journal of Infectious Diseases, which looked at four distinct cohorts – 200 subjects at least 70 years old who had already received the herpes zoster vaccine (ZV) 10 years or more prior (Group 1), 200 subjects at least 70 years old who had never received ZV (Group 2), 100 subjects ages 60-69 years old who had never received ZV (Group 3), and 100 subjects 50-59 years old who had never received ZV (Group 4) – to determine the efficacy of relatively late ZV administration on inducing an adequate immune response (J Infect Dis. 2016 Jan 1;213[1]:14-22. doi: 10.1093/infdis/jiv480).
“During aging there is a progressive decline in immune responsiveness to vaccination and a shortening of the duration of vaccine-induced immunity,” wrote Dr. Myron J. Levin of the University of Colorado, Denver, and his associates, who added that “as an initial step in investigating the potential for reversing this decline in efficacy, we determined that a booster dose of ZV administered to adults [at least] 70 years of age elicits a varicella-zoster virus (VZV) antibody response that is noninferior to that of ZV administered as a first dose.”
Dr. Levin and his coinvestigators separated subjects into one of the four aforementioned cohorts, enrolling individuals who had a history of varicella and had been U.S. residents for at least 30 years, but had no history of herpes zoster prior to enrollment. All individuals received a single, subcutaneous, deltoid region ZV (Zostavax) injection of 0.65 mL on the first day of the study, with subsequent blood samples collected and analyzed at 1, 6, and 52 weeks after receiving ZV. Subjects in Group 2 were matched with subjects in Group 1 based on age to compare results.
Baseline levels of both interferon gamma (IFN-gamma) and interleukin 2 (IL-2) were significantly higher in Group 1 than in Group 2. The geometric mean count of VZV-specific effector memory cells per million peripheral blood mononuclear cells in Group 1 was 47 at baseline, 88 at week 1, 90 at week 6, and 65 at week 52, vs. 36 at baseline, 65 at week 1, 73 at week 6, and 37 at week 52 in Group 2 (P less than .05). Similar disparities were seen between Groups 3 and 4, too, with Group 4 having consistently and significantly higher geometric mean counts at each collection of blood samples throughout the study.
“All age groups developed an increase in GMT [geometric mean titer] at week 1 after ZV receipt that peaked at week 6,” the authors explained. However, “the booster dose of ZV administered to adults [at least] 70 years old after [at least] 10 years elicited a GMT and geometric mean fold-rise in VZV antibody titer that was noninferior to that of ZV administered as a first dose to subjects [at least] 70 years old.”
The indication of that, the authors conclude, is that cell-mediated immunity is affected by ZV and enhanced by a stronger, or more recent, dose. This lends credence to the theory that although it is better to get a ZV shot earlier in life, those who are approaching age 70 years can – and, in many cases, should – get a booster shot to strengthen and maintain that immunity.
“Although the practical implications of the current findings are not fully understood, the similarity of [enzyme-linked immunosorbent spot] responses to those observed in the successful efficacy trial of ZV in vaccinees [at least] 60 years of age supports further investigation of administration of ZV at an early age vs. at a later age and further investigation of a booster dose for elderly individuals at an appropriate interval after initial immunization against HZ,” Dr. Levin and his coauthors concluded.
The study was funded by Merck, Sharp & Dohme. Dr. Levin reported having received grants, personal fees, and royalty payments from Merck. Several other coauthors disclosed individual potential conflicts of interest as well.