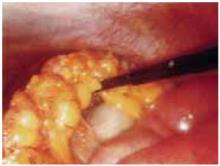
Minimally invasive surgery in ovarian cancer
Laparoscopy has dramatically altered management of many gynecologic malignancies, but its utility in ovarian cancer has been limited—until now.
Cyst rupture is no more likely with laparoscopy than with laparotomy,2 and is unrelated to the surgical route. It is more closely associated with the frequency of cystectomy.24
If rupture does occur, thoroughly irrigate the peritoneal cavity.
TABLE
When a cyst ruptures during surgery, what is the prognosis? The data are mixed on the significance of this event in stage I ovarian cancer
| AUTHOR | NUMBER OF CASES | IMPACT |
|---|---|---|
| Sevelda 1990 (Austria) | 204 | No prognostic importance |
| Sainz 1994 (US) | 79 | May worsen prognosis |
| Sjovall 1994 (Sweden) | 394 | No negative influence |
| Ahmed 1996 (UK) | 194 | Not prognostically significant |
| Vergote 2001 (Belgium) | 1,545 | Rupture should be avoided (hazard ratio = 1.64) |
How chemotherapy comes into play
If final pathology shows stage IC or high-grade histology, chemotherapy generally is offered to women managed in the United States. In selected cases, chemotherapy is given immediately after the initial surgery if completing a full staging procedure would considerably delay chemotherapy.
Leblanc et al21 found that, when staging was performed after completion of chemotherapy in women with stage IC or high-grade histology, 3 of 11 patients (27%) had positive nodes. Because positive nodes can be less chemosensitive, Leblanc and colleagues advocate either of 2 options: immediate restaging, including retroperitoneal nodes, or staging after chemotherapy, including retroperitoneal nodes.
Advanced Ovarian Cancer
Optimal surgical cytoreduction by laparotomy, followed by platinum-based chemotherapy, maximizes survival in women with advanced ovarian cancer. Unfortunately, in many patients, optimal debulking is not feasible, and laparotomy without optimal cytoreduction offers no survival advantage.25 At the same time, preoperative imaging has limited ability to determine the feasibility of cytoreduction. For example, computed tomography is highly sensitive when it comes to detecting ascites and mesenteric and omental disease (FIGURE 3), but is not as successful in detecting gallbladder fossa disease and diffuse peritoneal nodules smaller than 2 cm.
As a result, laparoscopy is increasingly used to determine whether optimal resection is feasible. If it is, immediate laparotomy is appropriate. Otherwise, a tissue specimen is obtained for histological confirmation, allowing accurate diagnosis prior to chemotherapy.
FIGURE 3 Omental cake signifies metastasis
Omental cake in a stage IIIC ovarian cancer patient. Disease appears to be resectable.
Potential drawbacks of laparoscopy
In selected women with advanced cancer, laparoscopy may be a good way to determine which patients would not benefit from laparotomy, thus sparing them the morbidity of an additional operation. But laparoscopy can have limitations:
- Ascites can reduce visibility.
- Omental and bowel adhesion to the anterior abdominal wall may increase the likelihood of bowel injury.
- Trocar site implantation may increase in the presence of adenocarcinoma, ascites, and carcinomatosis.13
If trocar sites are carefully closed and chemotherapy is initiated promptly, these risks can be substantially reduced.14
Is laparoscopy acceptable for restaging?
Leblanc E, Querleu D, Narducci F, Occelli B, Papageorgiou T, Sonoda Y. Laparoscopic restaging of early stage invasive adnexal tumors: a 10-year experience. Gynecol Oncol. 2004;94:624–629.
Yes, but only if the surgeon is highly skilled, with experience in both ovarian cancer and advanced laparoscopy. Comprehensive staging not only yields important prognostic information, but also identifies women who stand to benefit from chemotherapy.
The evidence: 10 years of experience
From 1991 to 2001, Leblanc et al21 laparoscopically restaged 53 women who had undergone incomplete staging for apparent stage I adnexal carcinoma.
Immediate (primary) restaging was done in 42 patients, and 11 were staged after completing chemotherapy (secondary restaging) for grade 3, clear-cell, or small-cell histology; FIGO stage IC cancer; or ruptured granulosa cell tumor.
Meticulous restaging technique:
- peritoneal washings and careful inspection,
- 8 to 10 random peritoneal biopsies (if peritoneal inspection was normal),
- BSO and hysterectomy (if not already done) or uterine curettage (if fertility was desired),
- bilateral pelvic and paraaortic lymphadenectomy,
- infracolic omentectomy.
The peritoneal cavity and trocar sites were irrigated at the end of the procedure, with full closure of any port sites larger than 10 mm.
Overall, laparoscopy was safe and successful
Complete laparoscopic restaging was performed in 52 women (98%). Dense adhesions indicated conversion to laparotomy in 1 case.
Four complications were directly related to the restaging procedure: a hematoma after epigastric vessel injury, 2 lymphocysts (managed laparoscopically), and 1 ureteric transection (which required laparotomy).The operation resulted in the following averages:
- operating time: 238 minutes,
- postoperative hospital stay: 3.1 days,
- node resection: 20 nodes in the paraaortic region and 14 in the pelvic dissection.
Mean follow-up was 54 months.
Outcomes
Of the 42 women who underwent primary restaging, 8 (19%) were upstaged—2 because of positive random peritoneal biopsies.
In the secondary restaging group, 4 of 11 women (36%) had their malignancies upstaged—3 because of positive retroperitoneal nodes and 1 because of positive random peritoneal biopsies. No port-site recurrences were observed in any of these patients.
One of the 8 patients upstaged in the primary restaging group had a recurrence 8 months postoperatively and died 16 months later. Of the 34 women with stage IA cancer after primary restaging, 3 (9%) had recurrences.
In the secondary-restaging group, 1 woman with small-cell carcinoma had a recurrence 10 months postoperatively and died 4 months later despite second-line chemotherapy.
Nine women had fertility-sparing surgery, and 3 later became pregnant and delivered without incident.