Implementation of an Automated Phone Call Distribution System in an Inpatient Pharmacy Setting
Background: Inpatient pharmacies receive numerous phone calls from health care professionals and patients. This uncaptured workload poses potential staffing concerns for pharmacy administrators as unequal distribution or misdirected calls to the pharmacy team can lead to accountability and patient safety concerns. We aimed to implement and evaluate the effectiveness of an automated call distribution (ACD) system in an inpatient pharmacy setting at a US Department of Veterans Affairs hospital.
Observations: A new inpatient pharmacy service phone line extension was implemented at the Edward Hines, Jr. Veterans Affairs Hospital in Illinois. The ACD phone system yielded positive performance metrics, including ≤ 30 seconds mean speed to answer and ≤ 5% abandonment rate in the 12 months after implementation.
Conclusions: The ACD phone system is a promising, new application of available technology implemented in a nontraditional setting. The ACD system provides more actionable information and quality metrics data to pharmacy leadership. The implementation of the ACD system has improved accountability, efficiency, work distribution, and the allocation of resources.
Training and Communication
Before implementing the inpatient pharmacy ACD phone system, the CPs and pharmacy technicians received mandatory ACD training. After the training, pharmacy team members were required to sign off on the training document to indicate that they had completed the course. The pharmacy team was trained on the importance of staffing the phones continuously. As a 24-hour pharmacy service in the acute care setting, any call may be critical for patient care.
A hospital-wide memorandum was distributed via email to all unit managers and hospital staff to educate them on the new ACD phone system, which included a new phone line extension for the inpatient pharmacy. Additionally, the inpatient pharmacy team was trained on the proper way of communicating the ACD phone system process with the hospital staff. The inpatient pharmacy team was notified that there would be an educational period to explain the queue process to hospital staff. Occasionally, hospital staff believed they were speaking to an automated system and hung up before their call was answered. The inpatient pharmacy team was instructed to notify the hospital staff to stay on the line since their call would be answered in the order it was received. Once the inpatient pharmacy team received proper training and felt comfortable with the phone system, it was set up and integrated into the workflow.
Postimplementation Evaluation
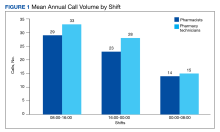
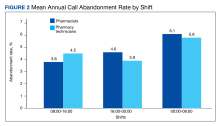
Inpatient pharmacy ACD phone system data were collected for 2021. To evaluate the effectiveness of an ACD system, the pharmacy leadership team set up the following metrics and goals for inpatient CPs and inpatient pharmacy technicians for monthly call volume/abandonment rate, mean speed to answer, mean call volume by shift, and the mean abandonment rate by shift.
Inpatient pharmacy technicians answered 27,655 calls with a mean call abandonment rate of 4.7%. and a mean 15.6 seconds to answer.
Discussion
Since implementing the inpatient pharmacy ACD phone system in January 2021, there have been successes and challenges. The implementation increased accountability and efficiency when answering pharmacy phone calls. An ACD uses an algorithm that ensures equitable distribution of phone calls between CPs and pharmacy technicians. Through this algorithm, the pharmacy team is held more accountable when answering incoming calls. Distributing phone calls equally allows for optimization and balances the workload. The ACD phone system also improved efficiency when answering incoming calls. By incorporating splits when a patient or health care professional calls, ACD routes the question to the appropriate staff member. As a result, CPs spend less time answering questions meant for pharmacy technicians and instead can answer clinical or order verification questions more efficiently.