Oropharyngeal Squamous Cell Carcinoma Outcomes by p16 INK4a Antigen Status in a Veteran Population
Background: The correlation between head and neck squamous cell carcinoma (SCC) and human papillomavirus (HPV) has been of great interest. We aimed to study immunoexpression of the p16 INK4a (p16) antigen, a surrogate marker for high-risk HPV infection, in oropharyngeal SCC among veterans to estimate HPV-related cancer and survival. Secondary aims included stratification of race and ethnicity, degree of tobacco and alcohol use, tumor location, stage, and age at diagnosis.
Methods: A retrospective electronic health record review was performed between January 1, 2000, and December 31, 2008, at a tertiary-level US Department of Veterans Affairs (VA) medical center for veterans who were treated for oropharyngeal SCC, had follow-up for a minimum of 2 years, and for whom paraffin-embedded tissue was available. Paraffin-embedded tissue was analyzed for p16 expression.
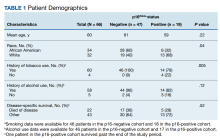
Results: We identified 66 veterans who met the inclusion criteria. p16 expression was observed in 29% of the patients. All patients were male with no difference in age at diagnosis between the groups. Among patients with p16-negative status, 60% were African American, whereas among patients with p16-postive status, 32% were African American ( P = .04). Among patients with p16-postive status, 22% were tobacco-naïve, and 18% were alcohol-naïve vs 0% and 4%, respectively, of patients with p16-negative status ( P = .005 and P = .12, respectively). Two-year survival was the same for both groups ( P = .52).
Conclusions: We observed p16 expression in 29% of VA patients with oropharnygeal SCC, which was less than observed in non-VA populations. At presentation, both groups demonstrated a predilection for tonsil location and late stage without significant difference in age or disease-specific survival. Disparities in racial distribution and tobacco use between patients with and without p16-positive status appear like that reported in non-VA populations; however, the frequently reported younger age at presentation, lower stage, and improved prognosis were not observed.
Since 1983, the correlation between head and neck squamous cell carcinoma (SCC) and human papillomavirus (HPV) has been of great interest to head and neck oncologists.1 In 1998, Smith and colleagues provided evidence of HPV as an independent risk factor for the development of head and neck SCC.2 HPV-associated head and neck SCC accounts for between 30% and 64% of oropharyngeal SCC, depending on the published study; tonsil primaries account for the majority of these cancers.3,4
The presence of HPV E6 and E7 oncoproteins leads to the inactivation of p53 and pRb tumor suppressors. Furthermore, Ragin and colleagues discussed a distinct molecular pathway specific to HPV-associated head and neck SCC, which was different from non–HPV-associated head and neck SCC, involving genetic mutations in CDKN2A/p16.5
Current methods in correlating the presence of HPV infection in head and neck SCC have centered on p16INK4a (p16) immunohistochemistry (IHC) staining and DNA in situ hybridization (ISH) for specific HPV DNA types. IHC staining for p16 involves a monoclonal antibody specific to p16. The usefulness of this test relies on p16 overexpression due to the inactivation of pRb by the HPV E7 oncoprotein. This test is readily performed on archived tissue and has a documented sensitivity and specificity of 100% and 79%, respectively, as reported by Singhi and Westra in 2010.6 HPV DNA fluorescence in situ hybridization is the gold standard for determining the presence of specific types of HPV DNA; however, p16 IHC can serve as a rapid, less costly means of studying archived tissue, lending its utility to retrospective population-based studies.
METHODS
A retrospective study was designed to determine the proportion of HPV-associated oropharyngeal SCC in a US Department of Veterans Affairs (VA) population, using p16 antigen IHC on paraffin-embedded tissue as the surrogate marker for the presence of HPV infection. Patients consisted of veterans who were treated for oropharyngeal SCC at Veterans Affairs Memphis Healthcare System (VAMHS) in Tennessee between January 1, 2000, and December 31, 2008. This data range allowed for at least 5 years of follow-up. Patients were excluded who lacked enough tissue specimens for analysis. Measurement outcomes included p16 expression, with subset analysis by race and ethnicity, degree of tobacco and alcohol use, tumor location, stage, age at diagnosis, and survival outcome. Microsoft Excel was used to calculate Fisher exact test, Student t test, and χ2 statistics. Significance was set at P < .05. This study received institutional review board approval from the University of Tennessee Health Science Center and the VAMHS.
RESULTS
We identified 66 total cases of oropharyngeal SCC; 19 cases (29%) were positive for p16. The mean age at diagnosis for the p16-positive cohort was 59 years vs 61 years for the p16-negative cohort (P = .22; Table 1).
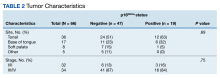
Although the tonsil was the most common site of tumor origin in both the p16-positive and negative cohorts (63% vs 51%, respectively), our analysis showed no statistically significant difference in sites of origin (P = .69) (Table 2).