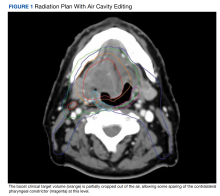
Contralateral Constrictor Dose Predicts Swallowing Function After Radiation for Head and Neck Cancer
Background: Radiation therapy can cause long-term dysphagia that seriously affects quality of life for survivors of head and neck cancer. This study evaluates a novel organ at risk, the contralateral pharyngeal constrictor muscles, to find out whether radiation dose to this structure predicts late swallowing function in patients with head and neck cancer.
Methods: The study included patients with head and neck cancer treated with radiation and concurrent systemic therapy at a single institution over 3 years. One-year dysphagia was defined as either the presence of a gastrostomy tube or an abnormal modified barium swallow ≥ 1 year after completion of radiation.
Results: Fifty-five patients met inclusion criteria, of which 46 were alive at 1 year. One-year dysphagia was present in 37% (n = 17) of this population. Contralateral constrictor V60 < 40% was associated with a 1-year dysphagia rate of 6%, compared with 57% in patients with V60 ≥ 40% (P < .001). An uninvolved pharynx mean dose < 45 Gy was associated with a 1-year dysphagia rate of 22%, compared with 52% in patients with an uninvolved pharynx mean dose ≥ 45 Gy (P = .03). Editing the clinical target volume off air cavities was associated with a decrease in 1-year dysphagia from 67% to 12% (P < .001), and with a reduction of contralateral constrictor V60 from 62% to 33% (P < .001). Air cavity editing was not associated with a change in locoregional recurrence or 1-year survival.
Conclusions: This is the first study to report a connection between contralateral constrictor dose and late swallowing function. The correlation between air cavity editing and contralateral constrictor V60 suggests that contralateral constrictor dose may depend partly on technique. Further studies are needed to explore whether these findings can be replicated prospectively and in other practice settings.
Radiation therapy can cause long-term dysphagia that seriously affects quality of life for survivors of head and neck cancer. 1-3 Numerous studies have linked pharyngeal constrictor dose to long-term dysphagia, but conclusions about the dose distribution that can be safely tolerated have been inconsistent. For example, a group from the Netherlands found that the mean dose to the superior pharyngeal constrictor muscle and the supraglottic larynx were each predictive of dysphagia. 4 A subsequent Vanderbilt study refuted these findings, reporting that these structures were not predictive but that dose to the inferior pharyngeal constrictor muscle was. 5 Other studies have connected late dysphagia with dose to the middle pharyngeal constrictor muscle, total larynx, oral cavity, contralateral submandibular gland, contralateral parotid gland, or a combination of these structures. 6-14 NRG Oncology trials commonly evaluate dose to the “uninvolved pharynx,” which is the total pharyngeal constrictor muscle volume minus the planning target volume (PTV) for the lowest dose target volume. NRG head and neck trials 3, 4, 5, 6, 8, and 9 all use uninvolved pharynx mean dose ≤ 45 Gy as a constraint to judge radiation plan quality.
Differences in methodology or patient population may explain the inconsistency of prior studies on dosimetric predictors of dysphagia, but it is possible that these studies did not evaluate the optimal metric for dysphagia. This study evaluates a novel organ at risk, the contralateral pharyngeal constrictor muscle, to determine whether dose to this structure is predictive of late swallowing function. The study also compares a constraint based on this structure to the NRG uninvolved pharynx constraint mentioned earlier.
Methods
This study is a retrospective review of patients treated at the Richard L. Roudebush Veterans Affairs (VA) Medical Center in Indianapolis, Indiana. Patients were identified by searching the VA Cancer Registry for patients treated for head and neck squamous cell carcinoma between September 1, 2016, and August 30, 2019. Eligible sites included cancers of the nasopharynx, oropharynx, hypopharynx, larynx and oral cavity, as well as head and neck cancer of an unknown primary site. Only patients treated with primary radiation with concurrent systemic therapy were included. Patients were excluded if they had prior surgery or radiation to the head and neck.
The pharyngeal constrictor muscles were contoured per the techniques described by Bhide and colleagues.11 The contralateral constrictor was defined as the half of the constrictor volume contralateral to the primary site. For midline tumors, the side of the neck with a lower volume of lymph node metastases was judged to be the contralateral side.
One-year dysphagia was defined as having a gastronomy tube (G-tube) in place or an abnormal modified barium swallow (MBS) ≥ 12 months after the completion of radiation. At the study institution, MBS is not routinely done after therapy but is ordered if a patient or clinician has concerns about swallowing function. MBS was considered abnormal if there was laryngeal penetration that reached the level of the glottis or was not ejected from the larynx.