The Design and Implementation of a Heart Disease Reversal Program in the Veterans Health Administration: Before and During the COVID-19 Pandemic
Background: Heart disease continues to be the leading cause of death in the US, and the number of people with cardiovascular disease (CVD) is rising. CVD is more prevalent among military veterans than nonveterans, and veteran status is associated with higher risk of incident heart disease after controlling for socioeconomic status, other medical diseases, depression, and lifestyle. Many patients seeking care in the Veterans Health Administration, including those who undergo cardiac catheterization, meet the criteria for multimorbidity (defined as ≥ 2 chronic diseases).
Observations: The Heart Disease Reversal Program (HDRP) is a novel interdisciplinary, multicomponent lifestyle program at the US Department of Veterans Affairs (VA) Sacramento VA Medical Center. This program is a streamlined adaptation of behavioral/lifestyle interventions aimed at promoting partial reversal (regression) of atherosclerotic heart disease and achievement of comprehensive cardiovascular risk reduction. HDRP was developed and implemented within a VA behavioral medicine clinic and successfully adapted for delivery through videoconferencing during the COVID-19 pandemic. Patient satisfaction survey data indicate a very high level of patient acceptability. We found direct-to-patient clinical outreach an effective method for launching a disease reversal program.
Conclusions: Beyond the clinical benefits to patients, there is significant value and benefit added to the health care system by offering an intervention within the disease reversal paradigm. Efforts of the health care team to reverse a disease can be considered the highest aim of medicine and health care.
Clinical practice guidelines for the treatment of patients with recent cardiovascular adverse events (AEs) include a referral to cardiac rehabilitation (CR).13 CR emphasizes exercise as the main intervention, along with coaching to promote multiple risk reduction. The most comprehensive CR program is intensive CR (ICR), including the Ornish ICR program.14 ICR includes 4 components: vegetarian diet, exercise, stress management (yoga, meditation), and group support. Ornish ICR has been shown to be efficacious in randomized controlled trials (RCTs).15-17 Three effectiveness studies, with 5,372 participants, demonstrated the real-world effectiveness of Ornish ICR in US hospitals.14,18,19 The program also was adapted successfully for the active-duty military and veteran population.20,21 Yet Ornish ICR is time intensive, and there are no certified VHA ICR Ornish sites. Furthermore, there is no formal strategy for targeting people with atherosclerotic CVD who no longer meet the criteria for CR or ICR. While Ornish ICR is highly effective for patients who are eligible and have access, a more effective and streamlined approach is needed for targeting many patients.
Nutrition may be the most powerful Ornish ICR component. The initial RCT conducted by Ornish and colleagues included only stress management training and a whole-food, plant-based (WFPB) diet, including grains, legumes, vegetables, fruits, nuts, and seeds. The trial found 91% of participants experienced reduced angina after only 24 days.15 The only single-component intervention study resulting in partial reversal of atherosclerosis was a WFPB diet-only study, which documented regression of atherosclerotic plaques after 5 years, using coronary angiography in 73% of participants, with arrested progression in the other 27%.22 Participants reported no cardiovascular AEs after 12 years.23 Furthermore, a number of other recent studies have demonstrated the benefits of WFPB diet-only interventions for type 2 DM (T2DM), hypertension, and obesity.24-27 The Heart Disease Reversal Program (HDRP) was developed to create an interdisciplinary lifestyle intervention that emphasized nutrition for a broad population of veterans with atherosclerotic CVD, of varying levels of functional ability, to promote comprehensive CVD risk reduction and bring heart disease reversal intervention into routine clinical practice.
Program Description
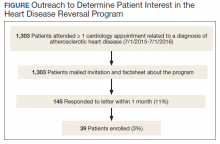
The Mental Health, Cardiology, and Nutrition and Food services all approved the launch of HDRP. We contacted veterans by mail, and 11% expressed interest (Figure). Among patients who received the initial mailed letter (prior to our accepting staff referrals), only 5% of patients who enrolled in HDRP reported previously being told about or prescribed a WFPB diet by any health care provider (HCP). Currently, patients are primarily referred to HDRP by Cardiology, Primary Care, and Mental Health services.