Study finds increased infant mortality for home births
AT THE PREGNANCY MEETING
NEW ORLEANS – Midwife-attended home births appear to have a higher mortality rate than midwife-attended hospital births, a new national database study suggests.
But for both physicians and families, the findings lie at the center of a tangled knot of statistics, philosophy, fear, and determination.
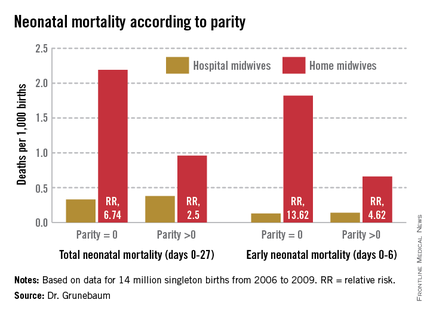
According to a new study of national birth and death statistics, total neonatal mortality in midwife-assisted hospital births was 0.32/1,000. For a midwife-attended home birth, that number was 1.26/1,000 – almost a fourfold increase in relative risk, Dr. Amos Grunebaum said at the annual Pregnancy Meeting sponsored by the Society for Maternal-Fetal Medicine.
His study drew its data from linked birth and death records available through the Centers for Disease Control and Prevention’s (CDC’s) database. The study looked at 14 million births from 2006 to 2009. Only healthy singleton infants of normal birth weight and vertex presentation were included; gestation was 38-42 weeks.
The figures for nulliparous women giving birth at home were even more striking, said Dr. Grunebaum, director of obstetrics at Weill Cornell Medical College, New York. Total neonatal mortality (deaths from day 0 to 27) was 2.19/1,000 for home-birthed infants, compared with 0.38/1,000 for hospital-born infants (relative risk, 6.74). The rates of early neonatal mortality (deaths from day 0 to 6) were 1.82/1,000 vs. 0.13/1,000, respectively (RR, 13.6).
"When we calculate the excess total neonatal deaths associated with home birth, we arrive at 9/10,000," he said during an interview. "If the trend of increasing home birth holds over the next few years, in 2016 we could have 32 excess neonatal deaths per year – a whole school class of children."
"It’s possible these risks are even higher," he added, because any babies born in the hospital after an emergency transfer from home are counted as hospital births.
It’s tough to parse out the details in his analysis, however. Because lay midwives would never have had hospital privileges, the in-hospital midwife group was likely composed entirely of certified nurse-midwives (CNMs), whose specialized training makes them highly skilled birth attendants. But the midwives who attended home births were a heterogenous group. In addition to CNMs, the analysis included anyone else who would register as "midwife" on a birth certificate – a group that represents an extremely varied range of skill.
These attendants could be could have been CNMs, certified midwives, certified professional midwives, licensed midwives, or lay midwives. CNMs must have a bachelor’s degree as a registered nurse and then graduate from an accredited school of nurse-midwifery. A certified midwife is a graduate of the same school of midwifery program, but can hold a degree in a field other than nursing. The American College of Nurse-Midwives (ACNM) regulates these providers.
No college degree is required for a certified professional midwife. They can obtain licensure based on an apprenticeship portfolio or from other schools of midwifery. The Midwives Alliance of North America and the National Association of Certified Professional Midwives regulate this group. Lay midwives are allowed to practice in some states, but there is no regulatory board, and no licensure or educational requirements.
In all probability, very few CNMs attended the home births in Dr. Grunebaum’s study, according to Jesse Bushman, ACNM’s director of advocacy and government affairs. The college’s own data indicate that 90% of deliveries performed by members are in hospitals. Only 30% of home births recorded in the CDC data were performed by CNMs, he said.
"That is one issue we have with Dr. Grunebaum’s results," Mr. Bushman* said in an interview. "There are many people who could call themselves a midwife who may not have the training or competencies that CNMs do. To lump them together is quite problematic."
In an interview, Dr. Grunebaum said that he had parsed out the mortality results by specific provider group. However, he would not release those numbers, saying it could jeopardize his study’s peer-reviewed publication. "I will tell you that CNMs at home did much, much worse than CNMs in the hospital, and that other midwives at home were not far behind."
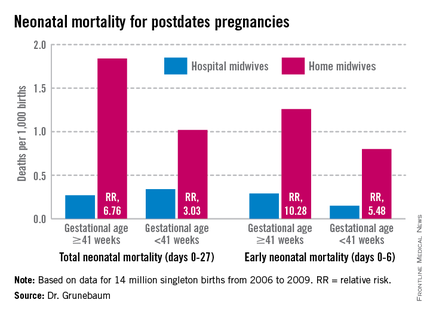
Birth outcomes data just released by the Midwives Alliance of North America (MANA) align with Dr. Grunebaum’s numbers (J. Midwifery Womens Health 2014 Jan. 30 [doi: 10.1111/jmwh.12172]). But the interpretation – if not the numbers – lies in the eye of the beholder. Dr. Grunebaum said the study illustrates the danger of home birth. MANA hailed it as proof of home birth’s safety.
"The results of this study ... confirm the safety and overwhelmingly positive health benefits for low-risk mothers and babies who choose to birth at home with a midwife," the group noted on its website. "At every step of the way, midwives are providing excellent care. This study enables families, providers, and policy makers to have a transparent look at the risks and benefits of planned home birth, as well as the health benefits of normal physiologic birth."






