Chronic genital skin disorders: 6 challenging conditions
When chronic skin disorders persist or recur, immune dysfunction may be a reason. Here’s how to respond.
It may be helpful to seek the assistance of an experienced dermatologist if a biopsy demonstrates this disorder.
Vulvovaginal yeast infection is often found in conjunction with chronic vulvar eczema.3 Infection is promoted by:
- deficient skin microbicides
- skin-surface disruption with flaking
- ineffective Langerhans-cell response to invading yeast.
Yeast organisms release proteins that further activate a local allergic response to perpetuate an environment that supports infection (FIGURE 4). This represents a breakdown in the skin’s natural defenses.
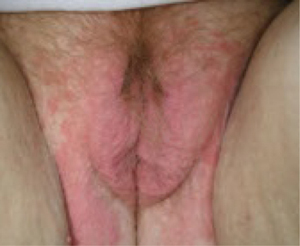
FIGURE 4 Yeast infection
Vulvar yeast rash in the normally occluded area of the vulva with large satellite lesions (erythematous patches around the margin of the vulvar rash). Satellite lesions are typically much smaller.
Oral therapy may be preferred
Topical anti-yeast creams often contain propylene glycol, an irritant to fragile skin, so oral therapy may be more appropriate. For oral therapy, 200 mg of fluconazole every 3 days for three doses is a useful starting point. For severe cases, this can be followed by a weekly 200-mg oral dose for 2 to 3 months to maintain yeast suppression while the underlying skin disorder begins to resolve. An extended course of oral fluconazole may not be appropriate during pregnancy or anticoagulation or while the patient is taking a statin drug to lower cholesterol. If oral therapy is not appropriate, 1% clotrimazole 7-day vaginal cream is the only topical agent in the United States that does not contain propylene glycol.
Beauty may be only skin deep, but that layer of epidermis is a pretty busy place. Among its activities is the production of hundreds of substances that regulate susceptibility to infection. More than 50 of these chemicals fall into the class of skin microbicides.8
We began to learn about these microbicides a decade ago, when researchers asked why eczema usually is secondarily infected with pathogenic staphylococcus, streptococcus, and yeast, and psoriatic skin isn’t. The answer: Both healthy and psoriatic skin produce natural microbicides, but allergic dermatitis (eczema) prevents their release on the skin surface.9
1. Proteins
Some proteins fight microbes better than pharmaceutical agents do. The most important antimicrobial proteins in the skin are defensins and cathelicidins, which are found in all epithelial structures, including the vulva and vagina.10 In the defensin category, human ß-defensins 2 and 3 are the most important proteins and are present in the surface epithelium. An inflammatory response triggers their release to inhibit microbes on the skin surface. The mean inhibitory concentration of human ß-defensin 3 against the relatively resistant yeast, Saccharomyces cerevisiae, is about 14 μg/mL.11 This inhibitory action is superior to many azole anti-yeast agents. Human cathelicidin is an equally effective skin microbicide, with antiviral, antifungal, and antibacterial activity. In normal function, these natural antimicrobial substances prevent colonization of pathogenic organisms in healthy skin.
2. Stratum corneum
The stratum corneum comprises the outer few microns of the epithelium. When it remains intact, the stratum corneum is an effective barrier to microbial invasion. Intact skin prevents substances with a molecular weight greater than 500 daltons from passing into the skin.
This barrier may be compromised by microtrauma or dermatologic disorders such as irritant or allergic dermatitis. Minimal microtrauma is all that is necessary to allow small microbes such as viruses to pass through the stratum corneum. Larger organisms (spirochetes, yeast) may require a greater degree of compromise, such as flaking skin. Environmental and dermatologic factors often compromise this natural barrier.
The vaginal epithelium is not keratinized and lacks an effective stratum corneum. Instead, vaginal tissue produces mucus, which floats on a thin transudate of intercellular fluid. Potential pathogens are captured in the mucus and drain out of the vagina. The vaginal epithelium produces several milliliters of mucus daily that is constantly draining out of the vaginal lumen.
3. Langerhans cells
The skin has a final layer of defense within its structure. Microbes that pass through the stratum corneum and enter the skin are attacked by defensive cells that reside there, known as antigen-presenting cells. Langerhans cells are the chief antigen-presenting cells in the skin. They originate in the bone marrow, but rest in the skin, awaiting microbial invasion.
Antigen-presenting cells kill intraepithelial microbes as they are detected, and then process the microbial antigens, enabling a cell-mediated immune response against the microbes. Langerhans cells also destroy individual cancer cells that appear randomly in the epithelium.
The genital skin and the skin around the mouth and eyes carry the highest concentration of Langerhans cells.12 Under normal conditions, Langerhans cells constitute as much as 8% of the cells in vulvar skin. In the genital area, the cervical transformation zone has the highest count of Langerhans cells13—possibly compensation for a highly vulnerable epithelial barrier, owing to the immature squamous epithelium at this site.
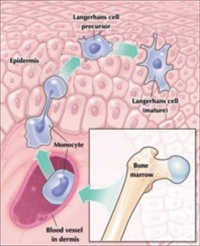
Maturation of a Langerhans cell
Langerhans cells, the main antigen-presenting cells in skin, defend it from microbes that breach the stratum corneum. Although Langerhans cells originate in bone marrow, mature cells reside in the epidermis.
With its high concentration of Langerhans cells, the cervical transformation zone may be the primary port of entry of HIV.14 Langerhans cells have a surface CD4 receptor to which HIV attaches. The Langerhans cells are unable to kill the HIV after phagocytosis. HIV-infected Langerhans cells then lead to systemic spread of the virus.
Overall, the antimicrobial function of Langerhans cells is imperfect. When a pathogen is located within a cell, some microbes, such as Chlamydia trachomatis, herpesvirus, and HPV, may evade detection. In addition, some dermatologic conditions are associated with significant dysfunction of Langerhans cells.






