Chronic genital skin disorders: 6 challenging conditions
When chronic skin disorders persist or recur, immune dysfunction may be a reason. Here’s how to respond.
In many cases, the dermatitis may exhibit no clinical signs beyond flakes of skin in the saline wet prep.
Start with a topical steroid
A trial of topical steroid ointment is appropriate, using a low-to medium-strength ointment such as 0.1% hydrocortisone butyrate, which may also lower the risk of yeast infection.
Several weeks of treatment may be necessary. It may take 4 to 6 weeks for a full layer of skin to be replaced. Subdermal atrophy, skin neovascularization, and other risks of topical steroids are of less concern during extended use of low-potency steroids, and may be more acceptable on an unexposed part of the body such as the vulva.
To test for therapeutic success, look for a reduction in pruritus and a lower incidence of yeast infection. Failure of steroid ointment and oral yeast suppression may justify vulvar biopsy, which should be submitted to a dermatopathologist.
Occasionally, a high-potency topical steroid such as clobetasol 0.05% ointment may be necessary (applied twice daily and rubbed in), but adrenal suppression may develop if therapy exceeds 3 to 4 weeks. The agent should be tapered rather than stopped abruptly.
Irritant contact dermatitis
This condition is characterized by a burning sensation. Common vulvar irritants include oxylate (in urine), propylene glycol (in medicated creams and lotions), and abrasive toilet paper. The list of potential irritants is long, and each irritant may have a different mechanism of action. A burning reaction after application of a topical cream suggests significant compromise of the skin barrier that would otherwise have prevented entry of the irritant. Skin-barrier compromise due to chronic, low-level vulvar irritant dermatitis likely contributes to acquisition of sexually transmitted disease.
Begin by identifying the culprits
The first step of treatment is recognizing and eliminating potential irritants such as bath soap, urine, topical creams that contain propylene glycol, and soap residue in clothing. Have the patient use a squirt bottle to rinse the genital area after urination to eliminate irritants such as oxylate. Also suggest that she rinse undergarments twice and use liquid rather than powder detergent. Cotton undergarments are more skin-friendly than synthetics.
Twice-daily or more frequent application of a skin moisturizer such as vegetable shortening, MimyX cream, or mineral oil/petrolatum cream (Eletone) helps to heal the skin, and continued use may prevent recurrence of symptoms.
When a patient complains of persistent vulvar pruritus and exhibits a figure-of-eight vulvar rash, suspect lichen sclerosus (FIGURE 2). The cause of this condition is unclear. Often, allergic contact dermatitis is superimposed on it. In older gynecologic terminology, this was referred to as mixed vulvar dystrophy.
Women with lichen sclerosus are at increased risk for persistent vulvar yeast infection and squamous vulvar cancer.
Vulvar biopsy occasionally discloses unexpected early lichen sclerosus.
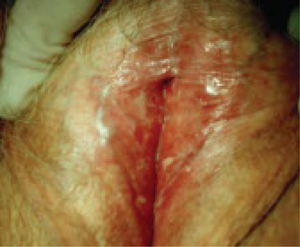
FIGURE 2 Lichen sclerosus
Note the labial agglutination (labia minora) and diffuse white epithelium, which are characteristic findings. If the areas of thickened epithelium do not resolve with topical steroid ointment, biopsy is appropriate.
Topical steroids are key to therapy
The degree of involvement that is grossly apparent determines the strength of the steroid ointment. If tissue is thickened, with areas of deep white change, a high-potency ointment such as clobetasol 0.05% may be necessary, applied twice daily for as long as several weeks. Milder cases may respond to a medium-strength topical steroid, such as fluticasone propionate 0.005% ointment.
If a higher-strength steroid is selected, it is appropriate to switch to a milder steroid as soon as symptoms resolve, with the goal of maintaining control with 1% hydrocortisone ointment or even continuous use of one of the skin moisturizers recommended for irritant dermatitis. Biopsy any thickened white patch, ulcerated area, or nonhealing skin fissure to check for squamous cancer.
Lichen planus
Erosive lichen planus (desquamative inflammatory vaginitis) of the vulva and vagina is an autoimmune skin disorder that causes superficial ulceration of the vaginal mucosa (FIGURE 3). An increase in vaginal discharge represents a shift in microflora away from lactobacillus dominance and an increase in the number of white blood cells and parabasal epithelial cells, with markedly heightened skin turnover. Local cellulitis does not develop, despite an overgrowth of various enteric organisms.
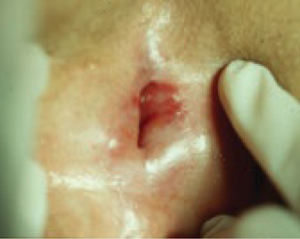
FIGURE 3 Lichen planus
This severe case resolved with a 3-month course of daily azathioprine (150 mg) but recurred after therapy ended.
A dermatologist may be required
Lichen planus is characterized by purulent discharge that contains bacteria, white blood cells, and parabasal cells. Unusual enteric microbes are often detected by routine culture, but antibiotic therapy is not helpful. Potent systemic anti-inflammatory therapy is often necessary rather than antimicrobial therapy. Daily azathioprine (Imuran) in doses ranging from 25 mg to 150 mg orally have been used, depending on the degree of vulvovaginal involvement. Tacrolimus ointment 0.1% applied twice daily may help in milder cases, but this agent typically causes an irritant reaction (burning) until the disorder partially resolves.






