Androgens in women: To replace or not?
Androgen therapy can improve sexual desire and response—here’s how
IN THIS ARTICLE
Although women produce only one tenth the amount of androgen that men do, testosterone and related androgen metabolites are as important to women throughout the lifespan as is estrogen. Androgens modulate a feeling of well-being, increase energy, support bone metabolism, and improve sexual function in women.1-3 But too much androgen production, with elevated levels of testosterone and dehydroepiandrosterone (DHEA), can result in hirsutism, acne, and infertility in the setting of polycystic ovary syndrome (PCOS), all of which present clinical problems.
An equally complicated topic is androgen insufficiency in women. Not only is it difficult to diagnose, it is a major clinical issue to decide whether, when, and how to replace androgens in women. In this article, I look at androgen production throughout the female lifespan, particularly the relationship between estrogen and androgen. I also describe the evaluation of androgen insufficiency, which requires understanding of androgen physiology and ovarian function before and after menopause. These issues form the basis of the decision to replace androgen in women.
Androgen over the lifespan
In the premenopausal woman, androgen production is approximately equally divided between the adrenal gland and the ovaries. Androstenedione from both is converted to testosterone and then irreversibly to dihydrotestosterone (DHT). Androstenedione, testosterone, and even DHEA are secreted in equal quantities by the adrenals and ovaries. The only androgen that is predominantly adrenal is DHEAS, which is sulfated in the adrenal gland.
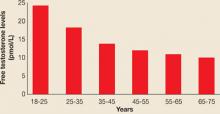
In premenopausal women, androstenedione is the precursor to testosterone, which is then metabolized to DHT, the androgen most active in hair follicles and implicated in hirsutism. It has been clear for many years that DHEA, although a weak androgen, is present in the greatest quantity in the circulation and is secreted during adrenarche, prior to menarche, beginning at ages 8 to 10. DHEAS peaks in young adulthood and begins to decline after age 40.4 The same is true for both total testosterone and free testosterone levels, which also decline in women after about age 25. Thus, peri- and postmenopausal women have approximately half the level of circulating androgens of women in their 20s (FIGURE 1, TABLE 1).5
FIGURE 1
Testosterone levels in women decline with aging
N=595
SOURCE: Davison S, et al5TABLE 1
How menopause affects plasma hormone levels
| HORMONE | MEAN PLASMA LEVEL | ||
|---|---|---|---|
| REPRODUCTIVE AGE* (N=15) | NATURALLY MENOPAUSAL (N=18) | OOPHORECTOMIZED (N=8) | |
| Estrone (pg/mL) | 58 | 49 | 48 |
| Estradiol (pg/mL) | 40 | 20† | 18 |
| Testosterone (ng/dL) | 44 | 30† | 12‡ |
| DHT (ng/dL) | 30 | 10† | <5‡ |
| Androstenedione (ng/dL) | 166 | 99† | 64‡ |
| DHEA (ng/dL) | 542 | 197† | 126§ |
| DHT=dihydrotestosterone, DHEA=dehydroepiandrosterone | |||
| * Mean value during early follicular phase | |||
| † P<.01 for comparison with reproductive age | |||
| ‡ P<.01 for comparison with naturally menopausal women | |||
| § P<.05 for comparison with naturally menopausal women | |||
| SOURCE: Vermeulen18 | |||
It matters how menopause happens
Circulating androgen levels are greatly influenced by menopause—how much depends on whether it occurs naturally with the ovaries intact, or by surgical removal of the ovaries. Not only does estradiol diminish significantly in naturally menopausal women, but all androgens do as well. In young oophorectomized women, estrogen levels are similar to levels in naturally menopausal women, but androgen levels—including testosterone, DHT, and androstenedione—are significantly lower than in naturally menopausal women, demonstrating that the circulating levels of androgen after natural menopause are still significantly greater than those in oophorectomized women.6 Thus, the postmenopausal ovary contributes significantly to circulating levels of androgen.
Androgen physiology
Both androgens and estrogens circulate in the bloodstream tightly bound to the protein sex hormone-binding globulin (SHBG), and more loosely bound to albumin. The SHBG-bound fraction is unavailable for biologic activity. Therefore, the amount of SHBG a woman produces is a key determinant of her level of androgen bioactivity. For this reason, it is crucial to measure circulating SHBG.
In a feedback mechanism, SHBG production is regulated by androgen and estrogen levels, with estrogen stimulating SHBG production and testosterone decreasing it.7 In the normal woman, about 65% of testosterone is bound to SHBG and 30% is bound to albumin, leaving only 0.5% to 2% free and bioactively available.8 In postmenopausal women taking hormone replacement therapy, SHBG increases, but the addition of methyltestosterone lowers the overall levels of SHBG, even in the presence of estrogen, increasing the amount of bioavailable testosterone simply by lowering SHBG levels. Postmenopausal replacement with estrogen alone decreases the amount of bioavailable testosterone because of higher SHBG levels.
SHBG is synthesized in the liver, whose metabolism is increased by exposure to steroids. Therefore, oral forms of estrogen replacement, which stimulate the liver because of the “first pass” effect, result in a greater increase in SHBG than do transdermal estrogen preparations.