A way to reverse CAD?
Though current medical and surgical treatments manage coronary artery disease, they do little to prevent or stop it. Nutritional intervention, as shown in our study and others, has halted and even reversed CAD.
ABSTRACT
Purpose Plant-based nutrition achieved coronary artery disease (CAD) arrest and reversal in a small study. However, there was skepticism that this approach could succeed in a larger group of patients. The purpose of our follow-up study was to define the degree of adherence and outcomes of 198 consecutive patient volunteers who received counseling to convert from a usual diet to plant-based nutrition.
Methods We followed 198 consecutive patients counseled in plant-based nutrition. These patients with established cardiovascular disease (CVD) were interested in transitioning to plant-based nutrition as an adjunct to usual cardiovascular care. We considered participants adherent if they eliminated dairy, fish, and meat, and added oil.
Results Of the 198 patients with CVD, 177 (89%) were adherent. Major cardiac events judged to be recurrent disease totaled one stroke in the adherent cardiovascular participants—a recurrent event rate of .6%, significantly less than reported by other studies of plant-based nutrition therapy. Thirteen of 21 (62%) nonadherent participants experienced adverse events.
Conclusion Most of the volunteer patients with CVD responded to intensive counseling, and those who sustained plant-based nutrition for a mean of 3.7 years experienced a low rate of subsequent cardiac events. This dietary approach to treatment deserves a wider test to see if adherence can be sustained in broader populations. Plant-based nutrition has the potential for a large effect on the CVD epidemic.
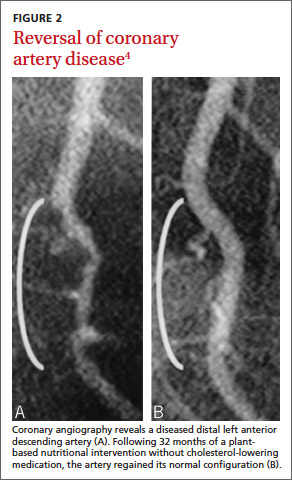
In a 1985 program initiated at the Cleveland Clinic, we examined whether plant-based nutrition could arrest or reverse advanced coronary artery disease (CAD) in 22 patients.1 One patient with restricted myocardial blood flow documented by positron emission tomography (PET) showed reperfusion on a repeat scan just 3 weeks after starting our nutritional intervention (FIGURE 1).2 Within 10 months of the start of treatment, another patient with severe right calf claudication and a quantifiably diminished pulse volume experienced total pain relief and exhibited a measurably increased pulse volume amplitude.2 Thus encouraged, we followed the small cohort of patients (adding cholesterol-lowering drugs in 1987) and reported results after 5 and 12 years of follow-up.1,3 Of the 22 patients, 17 were adherent to the protocol, and their disease progression halted. In 4 of the 12, we angiographically confirmed disease reversal,4 which can be striking (FIGURE 2).4
The significance of these findings. CAD remains the number one killer of women and men in western civilization despite 40 years of aggressive drug and surgical interventions.5 These approaches can be lifesaving in the midst of a heart attack. However, the elective use of percutaneous coronary intervention (PCI) shows little protection from future heart attacks or prolongation of life,6 perhaps because it does not treat the major cause of this disease. Such palliative treatments also carry significant risk of morbidity and mortality and lead to unsustainable expense.7

| 
|
Getting at the root cause of CAD requires a different approach. CAD begins with progressive endothelial injury,8 inflammatory oxidative stress, diminution of nitric oxide production, foam cell formation, and development of plaques that may rupture to cause a myocardial infarction (MI) or stroke.9 This cascade is set in motion in part by, and is exacerbated by, the western diet of added oils, dairy, meat, fowl, fish, sugary foods (sucrose, fructose, and drinks containing those, refined carbohydrates, fruit juices, syrups, and molasses) that injures or impairs endothelial function after each ingestion, making food choices a major, if not the major, cause of CAD.8,10-12
The study we report on here. In a continuation of the clinical strategy employing a plant-based nutrition intervention for CAD, we studied a separate cohort of 198 participants to determine if they could voluntarily adhere to the necessary dietary changes and to document their cardiovascular outcomes.
METHODS
Participants
This report reviews the outcomes of 198 consecutive nonsmoking patients with multiple comorbidities of hyperlipidemia (n=161), hypertension (n=60), and diabetes (n=23) who voluntarily asked for counseling in plantbased nutrition for disease treatment. These self-selected participants requested consultation after learning about the program through the Internet, the media, prior scientific publications, the senior author’s book (CBE Jr), other authors’ supportive comments, or word of mouth.2,13 A preliminary 25- to 30-minute telephone conversation established disease presentation and severity by eliciting reports of symptoms, history of MI, stress test and angiogram results, interventions undertaken, family history, lipid profile, and the presence of comorbid chronic conditions. In these calls, we outlined the program, established rapport, and documented the need for additional patient information. The Cleveland Clinic Institutional Review Board determined that these were acceptable outcome measurements to evaluate the nutrition program.
Intervention
We explained to each participant that plant-based nutrition typically succeeded in arresting—and sometimes reversing—CAD in our earlier study.






