MODULE 2: Rethinking the Role of Thiazide-Type Diuretics in the Management of Hypertension: Which Diuretic Is Best?
Considerations for greater chlorthalidone efficacy
The differences between CTD and HCTZ, despite similar molecular structures, is a topic of much discussion.23 It is likely that these 2 drugs have different pharmacokinetic and pharmacodynamic properties, as shown in TABLE 1.17
TABLE 1
,Pharmacokinetic/pharmacodynamic comparison of hydrochlorothiazide and chlorthalidone17
| Onset (h) | Peak (h) | Half-life (h) | Duration (h) | |
|---|---|---|---|---|
Hydrochlorothiazide
| 2 | 4-6 | 6-9 (single dose) 8-15 (long-term dosing) | 12 (single dose) 16-24 (long-term dosing) |
Chlorthalidone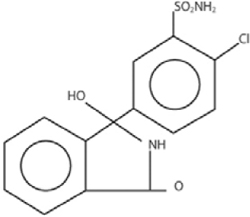
| 2-3 | 2-6 | 40 (single dose) 45-60 (long-term dosing) | 24-48 (single dose) 48-72 (long-term dosing) |
| Source: Hypertension by American Heart Association; Council for High Blood Pressure Research (American Heart Association); InterAmerican Society of Hypertension. Reproduced with permission of Lippincott Williams & Wilkins in the format Journal via Copyright Clearance Center | ||||
There is also evidence from an in vitro study that, compared with HCTZ, CTD has additional pleiotropic effects: reducing carbonic anhydrase activity, platelet aggregation, and vascular permeability while promoting angiogenesis.32
Another reason for the differences in efficacy between CTD and HCTZ could be the dosages of HCTZ used. Worldwide, nearly all prescriptions for HCTZ are for 12.5 to 25 mg/d, while most modern combination pills containing HCTZ incorporate these lower dosages.33 However, there is little evidence that such dosages lead to significantly improved outcomes.14,19,34-36
This was an issue in the Avoiding Cardiovascular Events Through Combination Therapy in Patients Living with Systolic Hypertension (ACCOMPLISH) trial. This study was designed to compare first-step therapy with benazepril/HCTZ 20/12.5 mg.37 Benazepril was force-titrated to 40 mg in each arm, whereas HCTZ and amlodipine were titrated to 25 mg and 10 mg, respectively, only if needed for BP control. The study was conducted in 11,506 high-risk patients 55 years of age and older. Other antihypertensive drugs could be added as needed for BP control. The study was stopped early after a mean follow-up of 36 months when the benazepril/amlodi-pine group demonstrated an HR of 0.8 (95% CI, 0.72-0.90) for the composite outcome of death from CV events, nonfatal MI or stroke, hospitalization for angina, resuscitation after sudden cardiac arrest, and coronary revascularization compared with the benazepril/HCTZ group.37
The ACCOMPLISH trial has been controversial for many reasons, with editorials suggesting that its design led to a “stacked deck” that favored amlodipine/benazepril over benazepril/HCTZ. Questions were raised as to why HCTZ was the diuretic of choice because CTD has been used in most thiazide-type trials. The dosages chosen were also questioned because outcome trials demonstrating reduced CV events with HCTZ used target doses of 50 mg/d or higher.14,21,22,38
Indeed, a meta-analysis published in 2011 found that despite the extensive use of HCTZ worldwide, the 12.5 to 25 mg dosage was inferior in reducing BP compared with standard doses of other antihypertensive agents (ACEIs, ARBs, beta blockers, and calcium channel blockers) in studies using 24-hour ambulatory BP monitoring.33 The efficacy of HCTZ closely mirrors that of the other drug classes at the 50-mg level, although that dose results in somewhat higher rates of hypokalemia. As the dose of HCTZ is increased to 100 mg, there is little or no further increase in antihypertensive efficacy, but hypokalemia becomes much more common.39
Thus, it can be clinically challenging to prescribe the optimum BP medication if practitioners prefer to use single-pill combinations that include HCTZ. Although the use of such single-pill combinations is warranted, particularly given the improved adherence with taking single-pill combinations compared with taking 2 or 3 pills, as noted in TABLE 1, most combinations include HCTZ dosages of 12.5 to 25 mg, which will often be less effective than full doses of 2 other medications.
Conclusion
Although thiazide-type diuretics are recommended as first-line therapy for most patients with hypertension, either alone or in combination with other classes of antihypertensives, they remain underused in clinical practice. In addition, HCTZ, which is the most commonly used diuretic (indeed, the most commonly prescribed antihypertensive) is prescribed at dosages too low to provide sufficient clinical efficacy in BP reduction and lower than what was proven to reduce CV events in clinical trials.
Chlorthalidone, a diuretic often considered a thiazide-type diuretic, has demonstrated superiority to HCTZ in reducing BP as evidenced in the MRFIT study and has been shown in numerous clinical trials to provide similar if not greater efficacy than other classes of antihypertensives in reducing BP, stroke, and CV events, with a good safety profile.
Clinicians need to manage patients with hypertension on an individual basis, selecting drugs and antihypertensive medication classes with the best outcomes in trials and then determining the most efficacious therapies with the lowest risk of adverse events for each patient. However, when prescribing a diuretic, they should also ensure that the drug used is prescribed at the appropriate therapeutic dosage level to enable patients to prevent the CV, thrombotic, and renal events that occur with long-term hypertension.






