Pulsed dye laser targets keratosis pilaris rubra
AT THE SPD ANNUAL MEETING
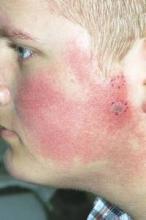
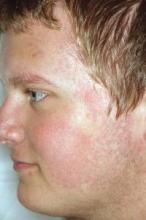
MILWAUKEE – Pulsed dye laser therapy reduced the redness associated with chronic keratosis pilaris rubra in as little as one session in a case series of seven adolescents.
The problem, however, is convincing insurers to pay for the procedure.
"That’s part of why we brought this to a forum like this meeting," Dr. Jennifer J. Schoch said at the annual meeting of the Society for Pediatric Dermatology. "These kids are so significantly affected by this and embarrassed [by the condition], that if we can do something in just one treatment and have a good response, it makes sense. But these kids required a lot of letters to the insurance companies, and a lot of them paid out of pocket."
Several attendees at the meeting echoed these comments, and some observed that pulse dye laser (PDL) therapy is not as effective in patients with higher Fitzpatrick skin types or that it was out of reach for their patients at a price tag of $200 or more per session.
"It seems to make a lot of sense, but I don’t think it would be worth the cost for my patients," Dr. Aimee Smidt, University of New Mexico, Albuquerque, said in an interview.
Keratosis pilaris rubra is often viewed as a benign condition, but one patient found it so socially disturbing that he flew from Alabama to Minnesota for treatment, said Dr. Schoch, a dermatologist at the Mayo Clinic in Rochester, Minn.
Dr. Schoch noted that there are few data in the literature on PDL treatment of keratosis pilaris rubra, and the current series is occurring over a 13-year-period at the clinic. In this series, adolescents aged 14-17 years received one to four sessions of PDL at a wavelength of 585 nm or 595 nm, for erythema and hyperkeratotic follicular papules on both cheeks. Two patients also received treatment to the chin, forehead and/or neck.
All patients had Fitzpatrick skin type I or II, five were male, and two also had ulerythema ophryogenes. Some patients had been misdiagnosed with severe acne, and all had failed a range of treatments including emollients, lactic acid, topical retinoids, urea, sulfacetamide lotion, and weak topical corticosteroids, as well as laser therapy with intense pulsed light, Fraxel, and Nd:YAG lasers, she said.
PDL treatment was physician-dependent. Starting fluences ranged from 4-9 J/cm2, with the goal of achieving a mild, bruiselike response. The spot size was predominantly 7 mm, and pulse duration was 1.5, 3, or 10 msec.
"I hypothesize that people are probably undertreating because it’s a benign condition, and you don’t want to cause problems, but to be effective, it seems you have to go for a little more aggressive response," Dr. Schoch said in an interview.
All patients experienced significant improvement after one to four treatments, based on patient report or provider assessment. Bruising resolved in 1-2 weeks. Resolution of erythema was observed, but not specifically measured. Patients also experienced some transient purpura, which was not well documented, said Dr. Schoch.
After 1-19 months follow-up, most patients remained satisfied with the results, although some flushing returned in two patients, she said. Blanching has not been a significant problem, and overlapping the treated areas reduced the risk of a honeycomb pattern developing on the skin.
The investigators are considering a prospective study to more objectively monitor responses. Treatment parameters will depend on patient’s response to test spots, Dr. Schoch said.
Dr. Schoch and her coauthors reported having no financial disclosures.