Interoceptive cues: When ‘gut feelings’ point to anxiety
Exploring patients’ somatic experiences can help expose their unconscious fears.
CASE: 'I don't know how I feel'
Ms. N, age 48, is seen in an outpatient clinic for episodic, impulsive aggression and evaluation of possible bipolar disorder. When you ask her to describe one of her episodes—which always involve a conflict with her partner or another loved one—Ms. N says, “I just lose control… I go blank.” You observe Ms. N’s deep, sighing respirations, trembling hands, and restless, fidgety leg movements. When you ask about her awareness of her physical state while she was recalling the incident, she immediately calms, looks at you quizzically, and states, “I don’t know how I feel.”
When assessing a patient who might have an anxiety disorder, don’t overlook the body. In addition to worry and avoidance, body-centered feelings are a vital component of anxiety and an important treatment target.1
This article:
- highlights clinically relevant neurobiology of anxious feelings
- discusses interoception—awareness of the physiologic state of one’s body—and its connection with anxiety
- explains the use of interoceptive cues as an aid to diagnosing and treating anxiety.
Affective neuroscience and fear
Interoceptive cues are questions directed toward the somatic manifestations of anxiety. Because these questions encourage patients to consciously experience the physical symptoms of anxiety, using interoceptive cues essentially is an exposure-based intervention that may feel counterintuitive to practitioners who are more accustomed to trying to relieve anxiety.
Emotions are thought to be grounded in brain areas that receive and regulate somatic signals, such as the amygdala and insula.2 A feeling-focused approach to anxiety weds affective neuroscience—the study of emotions—with clinical assessment and treatment of anxiety disorders, and conceptualizes that fear is a core component of many anxiety-related disorders.3,4
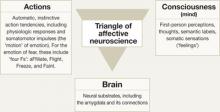
Although the DSM-IV-TR views anxiety disorders as clinically heterogeneous, affective neuroscience emphasizes what these disorders have in common.5 This unifying perspective allows clinicians to anchor anxiety disorders and anxiety-related disorders—such as hypochondriasis—in core emotional systems that have 3 clinically important aspects—actions (behavior and body), brain, and consciousness (mind) (Figure).4 Two emotional systems related to anxiety disorders are fear (anxious anticipation) and panic (evolutionarily related to separation anxiety and suffocation alarm signals). Viewing anxiety disorders as rooted in core emotion systems allows you to incorporate recent advances in emotional neuroscience, including interoception, into your clinical practice.
Figure: A,B,C model for understanding emotions
Affective neuroscience is a broad-based scientific discipline that explores emotions from 3 vantages: actions (behaviors and bodily responses), brain bases, and conscious manifestations. Two core emotional systems related to anxiety disorders are fear and panic.
Source: Adapted with permission from Panksepp J. Affective neuroscience. New York: Oxford University Press; 1998:31.
Detecting ‘hidden’ anxiety
Conscious symptoms. Activity in the brain’s fear system can generate conscious experiences, including worry, heightened arousal, attentional biases, and body-based feelings of fear. Anxious feelings—by definition, sensory experiences—are an important component of an anxiety assessment and relatively easy to identify.
Kroenke et al6 evaluated a 2-item screening tool, the Generalized Anxiety Disorder scale (GAD-2) that highlights both cognitive (worry) and somatic (feeling) sides of anxiety. Researchers asked 965 randomly sampled primary care patients, “Over the past 2 weeks, how often have you been bothered by the following problems:
- feeling nervous, anxious, or on edge
- not being able to stop or control worrying.
Possible responses ranged from 0 (not at all) to 3 (nearly every day). The GAD-2 was as specific for detecting anxiety disorders as a 7-item scale, the GAD-7, (88%), though less sensitive (65% vs 77%).
Nonconscious symptoms. A challenge arises, however, when patients demonstrate signs of anxiety (stress-related physical symptoms such as stomach pains or avoidance-related behaviors) without conscious awareness of anxious feelings. Though patients may intellectually understand the concept of body-based “gut feelings,” these sensations are often reflexively ignored, avoided, or mislabeled. Patients may use terms such as “stressed,” “distressed,” or “tense,” focus on the external source of the fear (rather than their response to it), or reflexively engage in behaviors (avoidance, impulsive behaviors) without being aware of their internal responses.
Anxiety symptoms that occur without corresponding awareness can be called occult, nonconscious, or unconscious anxiety. These symptoms, unique to each patient, can be used as:
- cues to the patient that he or she is anxious
- stimuli to be desensitized (via exposure-based interventions)
- markers of treatment progress.
Patients who experience occult anxiety often have a deficit in interoception (Box).2,7-11 Using interoceptive cues to foster awareness of these unrecognized body-based symptoms can provide insight into formerly unrecognized manifestations of anxiety.