Psychotic depression: State-of-the-art algorithm improves odds for remission
Consider an antipsychotic, even when paranoia or cognitive changes are more obvious than delusions or hallucinations.
Hypochondriasis is a characteristic of psychotic depression, and distinguishing body dysmorphic disorder and other somatoform-spectrum disorders from psychotic depression’s delusions may be difficult:
- Delusions in body dysmorphic disorder tend to be fixed over time.
- Delusions in psychotic depression tend to fluctuate in severity and may subside when the acute psychotic-depressive episode resolves.
ECT may be slightly more effective than medications for treating psychotic depression.13 ECT is not readily available in some regions, however, and the public has negative perceptions of “shock treatment.” Unfortunately, this stigma is often more influential than the evidence. According to some studies, less than 8% of U.S. psychiatrists offer ECT.14
Because medications are usually needed for maintenance treatment in psychotic depression, many clinicians choose medications over ECT as a first-line treatment. ECT should be considered as a first-line treatment for psychotic depression:
- in patients with a history of good response to ECT
- in patients with suicidal intent or severe inanition
- in older patients
- as second-line therapy for patients who fail to respond to or experience complications with medications.
Treatment recommendations
When a patient meets diagnostic criteria for psychotic depression, American Psychiatric Association practice guidelines12 recommend ECT or an antidepressant plus an antipsychotic. Although ECT may be slightly more effective than medications for treating psychotic depression, it is not readily available in many areas (Box).13,14
Medication has been shown to be effective in early studies that combined tricyclic antidepressants (TCAs) with conventional antipsychotics and in trials using selective serotonin reuptake inhibitors (SSRIs) and atypical antipsychotics.
Table 2
Medications reported effective for treating psychotic major depression
| Study, year of publication | Antipsychotic | Antidepressant |
|---|---|---|
| Double-blind studies | ||
| Spiker et al, 1985 | Perphenazine, 54 to 64 mg/d | Amitriptyline, 200 mg/d |
| Anton et al, 1990 | None | Amoxapine, 400 mg/d |
| Dube et al, 2002 | Olanzapine, 5 to 20 mg/d | Fluoxetine, 20 to 80 mg/d |
| Case reports and open-label studies | ||
| Quitkin et al, 1978 | Imipramine, 300 mg/d | None |
| Manberg et al, 1984 | Haloperidol, 20 mg/d | Bupropion, 300 mg/d |
| Nelson et al, 1986 | Perphenazine, 45 mg/d | Desipramine, 150 mg/d |
| Aronson et al, 1987 | Chlorpromazine, 1,000 mg/d | None |
| Howarth et al, 1989 | Imipramine, 248 mg/d | None |
| Rothschild et al, 1993 | Perphenazine, 32 mg/d | Fluoxetine, 40 mg/d |
| Banov et al, 1994 | Clozapine, 325 mg/d | None |
| Jacobsen, 1995 | Risperidone, 2.5 mg/d | None |
| Wolfersdorf et al, 1995 | Haloperidol, 2.5 to 10 mg/d | Paroxetine, 20 mg/d |
| Zarate et al, 2000 | Quetiapine (various) | ? (naturalistic chart review) |
Spiker and colleagues15 treated 58 patients with psychotic depression for 35 days, using amitriptyline, 200 mg/d; perphenazine, 64 mg/d; or the same dosages of amitriptyline plus perphenazine.15 Fourteen of 18 patients (78%) taking combination therapy achieved a >50% reduction in HRSD score, compared with 7 of 17 (41%) taking amitriptyline alone and 3 of 16 (19%) taking perphenazine alone.
In a more recent study,16 249 patients with psychotic depression were randomly assigned to:
- olanzapine, 5 to 20 mg/d, plus fluoxetine, 20 to 80 mg/d
- olanzapine, 5 to 20 mg/d, plus placebo
- or placebo.
Patients receiving olanzapine plus fluoxetine showed greater improvement in HRSD scores, compared with olanzapine monotherapy or placebo. Anecdotal reports indicate that quetiapine, risperidone, or olanzapine may be effective for patients with psychotic depression.17,18
We usually start with an SSRI plus an atypical antipsychotic (Algorithm). The atypicals have fewer side effects than conventional antipsychotics and may offer intrinsic antidepressant qualities through their effects on serotonin type-2 receptors. Table 2 lists recommended dosages.
When initial treatment fails
Consider second- and third-line options when patients fail to achieve remission with ECT or an SSRI plus an atypical antipsychotic. Document that first-line trials were of sufficient duration (8 to 12 weeks) and dosage.
We define remission as:
- HRSD score of <10 for at least 2 weeks
- score of 1 (no delusions or hallucinations) on the Schedule for Affective Disorders and Schizophrenia (SADS)
- and no longer meeting full criteria for a major depressive episode on the Structured Clinical Interview for DSM-IV.
We define partial remission as:
- HRSD score between 11 and 17
- HRSD improvement of >30% from baseline
- score of 1 on the SADS
- and no longer meeting full DSM-IV criteria for a major depressive episode.
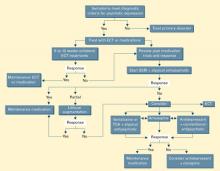
Algorithm State-of-the-art treatment of psychotic major depression
Lithium. We suggest adding lithium when patients respond partially to an SSRI/atypical antipsychotic combination. Although limited evidence supports lithium augmentation of antidepressants for psychotic depression, this strategy is often used.
Adding lithium to an antidepressant/antipsychotic combination was examined in a retrospective chart review of patients treated for bipolar and unipolar psychotic depression.19 Lithium, 600 to 1,200 mg/d, was added when patients did not respond to desipramine, 150 mg/d, plus either perphenazine, 12 to 64 mg/d, or haloperidol, 4 to 20 mg/d. Eight of nine patients with bipolar psychotic depression achieved remission with the added lithium, compared with 3 of 12 patients with unipolar psychotic depression (p = 0.003).