Hysteroscopy: Managing and minimizing operative complications
Techniques to assess the site, spot imminent perforation, and avoid or correct the 5 most common types of problems.
When perforation occurs during the use of thermal energy, laparoscopy is necessary to assess the organs overlying the site.9 During setup for laparoscopy, bring the hysteroscope near the area of perforation to inspect the bowel beyond the uterus. Since the pelvis fills quickly with distention fluid, the hysteroscope can even be placed through the perforation to yield an excellent view of the undersurfaces of the bowel immediately adjacent to the injured area (FIGURE 3). (Disconnect the electrosurgical cord before doing this!)
Thorough laparoscopic inspection of the bowel in the pelvis often reveals thermal injury, which appears as a whitish patch on the bowel serosa. To repair bowel injuries, bring the injured segment out through a minilaparotomy and excise the damage with a 2- to 3-cm border. A general surgeon should be called in to consult.
A 42-year-old woman who underwent endometrial ablation 2 years earlier presents with persistent menorrhagia and a 12-week–size fibroid uterus and expresses a desire for repeat ablation. At the second surgery, the uterine cavity appears scarred, with multiple synechiae.
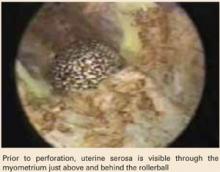
As the procedure progresses, the uterine serosa becomes visible from within the cavity, appearing as a smooth, bluish structure that can be moved with only slight pressure. As the ablation continues, the uterus perforates, necessitating laparoscopic inspection of the organs overlying the site.
Although the patient recovers, her menorrhagia eventually returns, and she opts for laparoscopically assisted vaginal hysterectomy 1 year later.
Uterine perforation is more likely during repeat procedures
This case illustrates one of the most common risks of operative hysteroscopy: uterine perforation, which occurs more frequenly in repeat procedures.
The case also highlights an important indicator of perforation: the serosal sign, which I first described in 1996.24 When the smooth, bluish structure appears, cease ablation in the region immediately.
If no injury is apparent, discharge the patient but follow her closely, including daily white blood cell counts for 4 to 5 days. Instruct her to take her temperature twice daily and return to the hospital immediately if any signs of bowel perforation develop. Delayed perforation from thermal injury can occur as late as 2 weeks following surgery, and the patient should be apprised of this possibility.
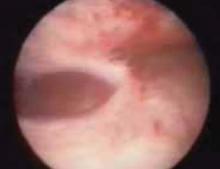
FIGURE 1 Signs of a false passage
Myometrial fibers signal that a false passage has been created. Stop the procedure even if no perforation is detected, to prevent distention fluid from being absorbed into the circulation through the injury.
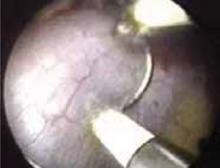
FIGURE 2 Risk of myomectomy: Myometrial avulsion
Small bowel visible within the uterine cavity after avulsion of uterine wall at the time of myomectomy
FIGURE 3 Use the hysteroscope to assess perforation site
Hysteroscopic view of perforation at the fundus. The small bowel is visible beyond the perforation at left.
Intraoperative bleeding is rare
Bleeding is unlikely unless vessels are lacerated or injured in the cervical canal or lower uterine segment during dilation or deep ablation or vaporization. Bleeding is more common when endomyometrial resection is performed with the wire loop electrode or during ablation or vaporization of fibroids. Bleeding sufficient to require intervention occurs at a rate of 0.5% to 1.9% in several reported series.
To achieve hemostasis via balloon tamponade, insert a Foley catheter with a 30-cc balloon into the uterine cavity, inject 15 to 20 mL (or more for a larger cavity) of fluid into the balloon, and observe the patient.10 If there is no bleeding in 1 hour, remove half the fluid. Remove the remainder of the fluid and the catheter over the next hour if no further bleeding occurs.
Alternative method: Pack the uterus. I prefer 1/2-inch–gauge packing that has been soaked in a dilute vasopressin solution (20 U [1 mL] in 60 mL normal saline).11
The benefits of vasopressin. Before balloon tamponade or packing the uterus, I inject very dilute vasopressin (4 U [0.2 mL] in 60 mL normal saline) directly into the cervix 2 cm deep, at the 4 and 8 o’clock positions. Phillips12 demonstrated a marked decrease in blood loss during resectoscopic surgery using this approach. I also do this routinely prior to operative hysteroscopy, since the vasopressin-induced vasoconstriction reduces intravasation of distention media.
A vaporizing electrode may prevent significant blood loss during myoma resection by sealing blood vessels as the tissue is vaporized.13 All major manufacturers of hysteroscopic equipment produce these electrodes.
In my series of 44 endometrial ablations and hysteroscopic myomectomies performed with the vaporizing electrode, blood loss was “minimal” or less than 50 mL in 29 cases. The maximum blood loss was 300 mL in a patient with a 4-cm submucous myoma who was managed emergently for hemorrhage.14 In another case, during resection of a 5-cm submucous myoma, I encountered significant bleeding from large vessels at the base of the myoma, which required intrauterine tamponade with a vasopressin-soaked pack.