What Ob/Gyns need to know about drug therapy in bipolar gravidas
Careful attention to dosing, drug combinations, and the risks of key psychotropic agents can help prevent fetal malformations and reduce the risk of relapse.
- All psychotropic medications cross the placenta. If psychotropic medication is used, prescribe carefully during the first trimester, giving the minimum number of drugs and the lowest dosages needed to restore or maintain well-being.
- No psychotropic agents are FDA-approved for use in pregnancy.
- Teratogenicity notwithstanding, psychotropic intervention is the most effective treatment for women with bipolar disorder.
- We recommend that women who continue to take valproate or carbamazepine during pregnancy receive folate, 3 to 4 mg/d, as a precaution.
Managing gravidas with bipolar disorder requires obstetricians to balance the potential for neonatal malformations against the high risk of relapse when patients discontinue medications.1 This article offers an evidence-based approach that includes:
- analysis of the US Food and Drug Administration’s (FDA) teratogenicity categories for psychotropics
- safety profiles of drugs used in mood stabilization
- an algorithm for managing patients who are considering conception or are pregnant
When a patient is at risk for severe psychiatric problems before, during, and after pregnancy, a collaborative effort between the obstetrician and psychiatrist may be best for both the patient and her child.
Further, because low maternal folate levels are associated with neural tube defects, and some anticonvulsant agents used for mood stabilization diminish supplies of the nutrient, supplementation is essential. (See “Folate and neural tube defects”.)
Psychotropic risks to offspring
All psychotropic medications cross the placenta, exposing the fetus to some degree. Risks include teratogenicity, obstetric complications, perinatal syndromes, and long-term postnatal behavioral sequelae.
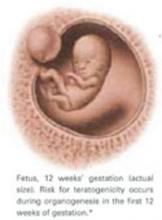
Teratogenicity. A medication is considered teratogenic when prenatal exposure significantly increases the risk of congenital deformities over the baseline, which is 2% in the United States.2 The cause of most congenital malformations is unknown. Risk for teratogenicity occurs during organogenesis in the first 12 weeks of gestation.
Obstetric complications include preterm delivery, low birth weight, and delivery complications such as low Apgar scores or behavioral effects requiring intensive care.
Perinatal syndromes include physical and behavioral symptoms noticed in the infant shortly after birth (such as jitteriness). These consequences are putatively related to drug use at or near birth and have limited duration.
Postnatal behavioral sequelae include long-term neurobehavioral abnormalities in children who were exposed to psychotropics in utero.
Balancing risks
Risks with medication. The FDA’s “use-in-pregnancy” rating system (TABLE 1) uses available data to assess the degree of teratogenic risk. These guidelines are one of many tools to use when considering drug treatment.
Most psychotropics are category “C” or “D,” which imply a chance of harm to the exposed fetus. Category “B” drugs would appear safer, but this rating could simply indicate a lack of adequate human data or that no data have shown harm in animals.
Moreover, a category “D” drug may be chosen more often during pregnancy than a category “C” drug. This may occur when more human data exist on using the category “D” drug in patients with a particular disorder (such as using lithium versus valproate or olanzapine in pregnant women).
No psychotropics are classified as “A,” meaning either some risks are associated with every psychotropic or the risk of some agents has not been adequately explored. Furthermore, no psychotropics are FDA-approved for use during pregnancy.
Risks without medication. Teratogenicity notwithstanding, psychotropic intervention is the most effective treatment for women with bipolar disorder. Patients who discontinue mood-stabilizing medication after conception significantly increase their likelihood of a relapse into depression or mania,3 either of which could lead to complications and untoward effects on the fetus.
Depression during pregnancy has been linked to low birth weight and preterm delivery.4,5 These effects may be mediated by the illness itself or by other factors that indirectly affect birth outcomes. For example, depression during pregnancy is associated with decreased appetite, substance use and abuse, and lower use of prenatal care.6
Untreated mania may also be associated with perinatal risks, as a pregnant patient in a manic state may engage in impulsive, high-risk behaviors that endanger herself and her fetus.7
TABLE 1
FDA use-in-pregnancy ratings for medications
| CATEGORY | DESCRIPTION |
|---|---|
| A | Adequate, well-controlled studies in pregnant women have not shown an increased risk of fetal abnormalities |
| B | Animal studies have revealed no evidence of harm to the fetus; however, no adequate and well-controlled studies have been conducted in pregnant women |
| OR | |
| Animal studies have shown an adverse effect, but adequate and well-controlled studies in pregnant women have failed to demonstrate a risk to the fetus | |
| C | Animal studies have shown an adverse effect and no adequate and well-controlled studies have been conducted in pregnant women |
| OR | |
| No animal studies have been conducted and no adequate and well-controlled studies have been conducted in pregnant women | |
| D | Studies—adequate and well-controlled or observational—in pregnant women have demonstrateda risk to the fetus. However, the benefits of therapy may outweigh the potential risk |
| X | Studies—adequate and well-controlled or observational—in animals or pregnant women have demonstrated positive evidence of fetal abnormalities. The use of the product is contraindicated in women who are or may become pregnant |
| Data from US Food and Drug Administration38 | |