A cheaper, faster way to resolve chronic cough
“Presumed diagnosis” strategy offers early treatment, a cost savings, and >90% treatment response.
1. Postnasal drip syndrome. Patients first underwent a rhinoscopic examination (FIGURE). When clinicians detected redness or abnormal discharge on the nasal mucosa, they prescribed a 5-day course of antihistamine (10 mg/day ebastine [Ebastel] orally), pseudoephedrine (30 mg 3 times daily, orally), and intranasal corticosteroid (triamcinolone acetonide [Nasacort] 110 mcg twice daily intranasally). Patients without symptoms of rhinitis were referred to the next diagnostic phase.
With completion of the prescribed medication 5 days after the first visit, we graded the severity of cough by questionnaire. Patients in the successful and partial responder categories received a presumptive diagnosis of postnasal drip syndrome, and we asked them to continue using the medication for at least 2 weeks. We had each nonresponder stop the medication.
2. Asthma syndrome. Partial responder and nonresponder patients entered the next diagnostic phase: a methacholine bronchial provocation test (MPT)7 and eosinophil count with induced sputum by hypertonic saline (3% NaCl).8 We defined a positive MPT result as <10 mg/ mL of methacholine causing a 20% fall in FEV1 from baseline (PC20). Patients with more than 3% eosinophils in the induced sputum specimen or with a positive MPT received a 1-week prescription for inhaled budesonide 160 mcg twice daily and inhaled formoterol (Symbicort) 4.5 mcg twice daily. Patients who did not exhibit these asthma indicators were referred to the next step.
At the next visit, we again graded the severity of cough. Patients in the successful and partial responder categories received a presumptive diagnosis of asthma syndrome. We asked successful and partial responders to continue the medication for at least 2 weeks. Those classed as nonresponders were asked to stop their medication. We referred all patients with positive MPT test results to a special clinic for asthma, regardless of responses to this therapeutic trial or eosinophil count in the induced sputum.
3. Reflux syndrome. Partial responders and nonresponders then received a 2-week prescription for a proton pump inhibitor, pantoprazole (Pantoloc), 40 mg orally once daily.9 At the next visit 2 weeks later, we graded the severity of cough. Successful and partial responders were given a presumptive diagnosis of reflux syndrome, but only successful responders were asked to continue the same medication for at least 6 weeks. At the discretion of their physicians, partial and nonresponders underwent other diagnostic investigations, including high-resolution computerized tomography (CT) of the lungs, bronchoscopic examination, sputum smear and culture for acid fast bacilli, sputum culture for ordinary bacteria and fungi, and a serological test for human immunodeficiency virus.
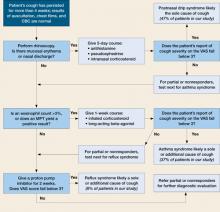
FIGURE
A presumptive-diagnosis algorithm
Chronic cough resolved for more than 90% of patients treated according to this algorithm.
MPT, methacholine bronchial provocation test; VAS, visual analog scale.
Results
Presumptive diagnoses
Among 378 patients, 346 (91%) showed erythematous mucosa or abnormal discharge in rhinoscopic examinations and received empiric medication for 5 days. The successful-responder category included 176 patients (47%); 79 (21%) were classed as partial responders, and 255 (67%) received the presumptive diagnosis of postnasal drip syndrome. Among the 346 treated patients, 91 (24% of those enrolled, or 26% of treated) showed no response.
Thirty-two patients with normal rhinoscopic findings and 170 categorized as partial or nonresponders in the first step underwent an MPT and eosinophil count of induced sputum. One hundred forty-four showed positive results and received empiric treatment for 1 week. Among these, 141 were deemed successful responders (37% of enrolled, or 98% of treated), 3 partial responders (1% of enrolled, or 2% of treated), and none were nonresponders.
In all, 61 patients had empiric treatment for reflux syndrome for 2 weeks; 58 had normal findings for both the MPT and sputum eosinophil count, and 3 were classified as partial responders in the previous therapeutic trial. Twenty-nine patients (8% of enrolled, or 47% of treated) were classified as successful responders after 2 weeks (TABLE 2).
TABLE 2
Presumptive diagnoses corresponded to expected frequency (and occasionally co-existed)
| DIAGNOSIS | NO. OF PATIENTS (%)* N=378 |
| Postnasal drip syndrome | 255 (67.5) |
| Asthma syndrome | 144 (38.1) |
| Reflux syndrome | 29 (7.7) |
| CO-EXISTING PATHOLOGIES | 82 (21.7) |
| Postnasal drip syndrome and asthma syndrome | 52 (13.8) |
| Postnasal drip syndrome and reflux syndrome | 7 (1.9) |
| Postnasal drip syndrome and other diagnosis | 20 (5.3) |
| Asthma syndrome and other diagnosis | 3 (0.8) |
| * The percentage of patients under "Diagnosis" does not add up to 100% because some patients had more than one condition, accounted for under "Co-existing pathologies." | |
Therapeutic response period for successful responders
Within 5 days of beginning the course determined by the algorithm (Figure), 176 patients (47%) who received treatment for presumed postnasal drip syndrome experienced resolution of their chronic cough.