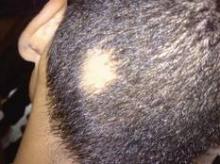
New Era in Alopecia Areata Therapy Beckons
EXPERT ANALYSIS FROM THE ANNUAL MEETING OF THE SOCIETY FOR INVESTIGATIVE DERMATOLOGY
RALEIGH, N.C. – Recent genetic insights into the roots of alopecia areata have fostered the development of new therapeutic targets, with clinical trials offering promising results.
The investigational drugs are, for the first time, addressing the underlying disease mechanism, Angela M. Christiano, Ph.D., said at the annual meeting of the Society for Investigative Dermatology.
Alopecia areata affects roughly 5.3 million Americans of all ages and ethnic groups. The dramatic hair loss exacts an underappreciated, often devastating toll in terms of patient self-esteem and quality of life. To date, treatment has been unsatisfactory, with intralesional injections of glucocorticoids being the mainstay. Wigs are big.
But all of that may be about to change. "Our translational studies offer us the beginning of a therapeutic arsenal," said Dr. Christiano, professor of dermatology and genetics at Columbia University in New York.
She and her colleagues have identified interleukin-15 as a novel and highly promising therapeutic target in alopecia areata.
Interleukin-15 is required for the growth and sustenance of the natural killer-type CD8+ cells that surround the growing end of the hair follicle during active disease. This dense infiltrate of activated T cells, known as the "swarm of bees," is the pathognomonic finding in alopecia areata.
Interleukin-15 is an attractive therapeutic target because it can be addressed along the IL-15 signaling pathway by using Janus kinase inhibitors. Dr. Christiano and her coworkers have found evidence that both the oral and compounded topical formulations of tofacitinib and ruxolitinib are effective for the prevention and treatment of alopecia areata in a mouse model of the disease.
Tofacitinib inhibits the Janus kinase 3 (JAK-3) enzyme located along the IL-15 signaling pathway. The investigational oral agent recently received a thumbs-up recommendation for the treatment of rheumatoid arthritis from a Food and Drug Administration advisory panel.
In Dr. Christiano’s mouse model of alopecia areata, when tofacitinib was administered when mice received diseased grafts, 100% of the animals retained their hair. The same phenomenon occurred when the mice were treated prophylactically with oral ruxolitinib (Jakafi), a JAK1/2 inhibitor marketed for the treatment of myelofibrosis and under investigation for the treatment of other diseases.
Dr. Christiano and her coworkers also formulated the two JAK inhibitors into a 0.5% cream for topical application. The topical agents prevented the development of alopecia areata in mice, and they triggered hair regrowth when applied to mice with established disease. At the molecular level, these drugs resulted in reversal of a pathologic interferon-gamma gene expression signature.
"The follicular expression of molecules changes back to an immune-privileged phenotype. We’re very encouraged by what we’ve seen so far with this," she said.
Alopecia has long been recognized as having a strong genetic component. The relative risk of the disease in first-degree relatives of affected individuals is increased 10-fold. Twin concordance studies have demonstrated that when one monozygotic twin has alopecia areata, there is more than a 50% chance that the other twin will be affected, whereas there is zero concordance in dizygotic twin pairs.
It’s also well recognized in the research community that the normal hair follicle is one of the few tissues in the human body that enjoys a state of immune privilege protecting it from autoimmune attack. Normal hair follicles are cloaked from immune recognition. The collapse of this immune privilege is what allows the "swarm of bees" leading to alopecia areata.
"Notably, the stem cell compartment is spared from the disease, which gives patients the ability, even after many years of longstanding disease, to experience spontaneous regrowth for reasons we really don’t understand," Dr. Christiano explained.
While the JAK inhibitors haven’t made it to clinical studies, another novel therapy in alopecia areata will be the focus of a small clinical trial slated to begin in July. Abatacept (Orencia) is a biologic agent approved for the treatment of rheumatoid arthritis. It is also in ongoing clinical trials for other autoimmune diseases, including type 1 diabetes. Abatacept is a soluble fusion protein that serves as a selective costimulation modulator and T-cell activation suppressant. Last summer, the intravenously administered formulation of abatacept was joined by a subcutaneous version permitting patient self-treatment.
"That makes it more appealing for the treatment of alopecia areata," she noted.
Dr. Christiano’s research is funded by the National Institutes of Health, American Skin Association, and National Alopecia Areata Foundation. She reported having no financial conflicts.