High ankle sprains: Easy to miss, so follow these tips
Misdiagnosis can result in increased loss of play time and chronic ankle dysfunction. Here are the physical exam maneuvers and imaging options to consider.
PRACTICE RECOMMENDATIONS
› Maintain a high level of suspicion for syndesmotic injury in any athlete describing an external rotation or hyper-dorsiflexion ankle injury. A
› Obtain weight-bearing anteroposterior- and mortise-view ankle x-rays in all cases of suspected syndesmotic injuries. A
› Consider stress x-rays of the affected ankle, contralateral ankle x-rays for comparison views, or advanced imaging with magnetic resonance imaging (MRI) or computed tomography if initial x-rays are unrevealing. A
› Treat stable syndesmotic injuries with conservative measures and rehabilitation. A
Strength of recommendation (SOR)
A Good-quality patient-oriented evidence
B Inconsistent or limited-quality patient-oriented evidence
C Consensus, usual practice, opinion, disease-oriented evidence, case series
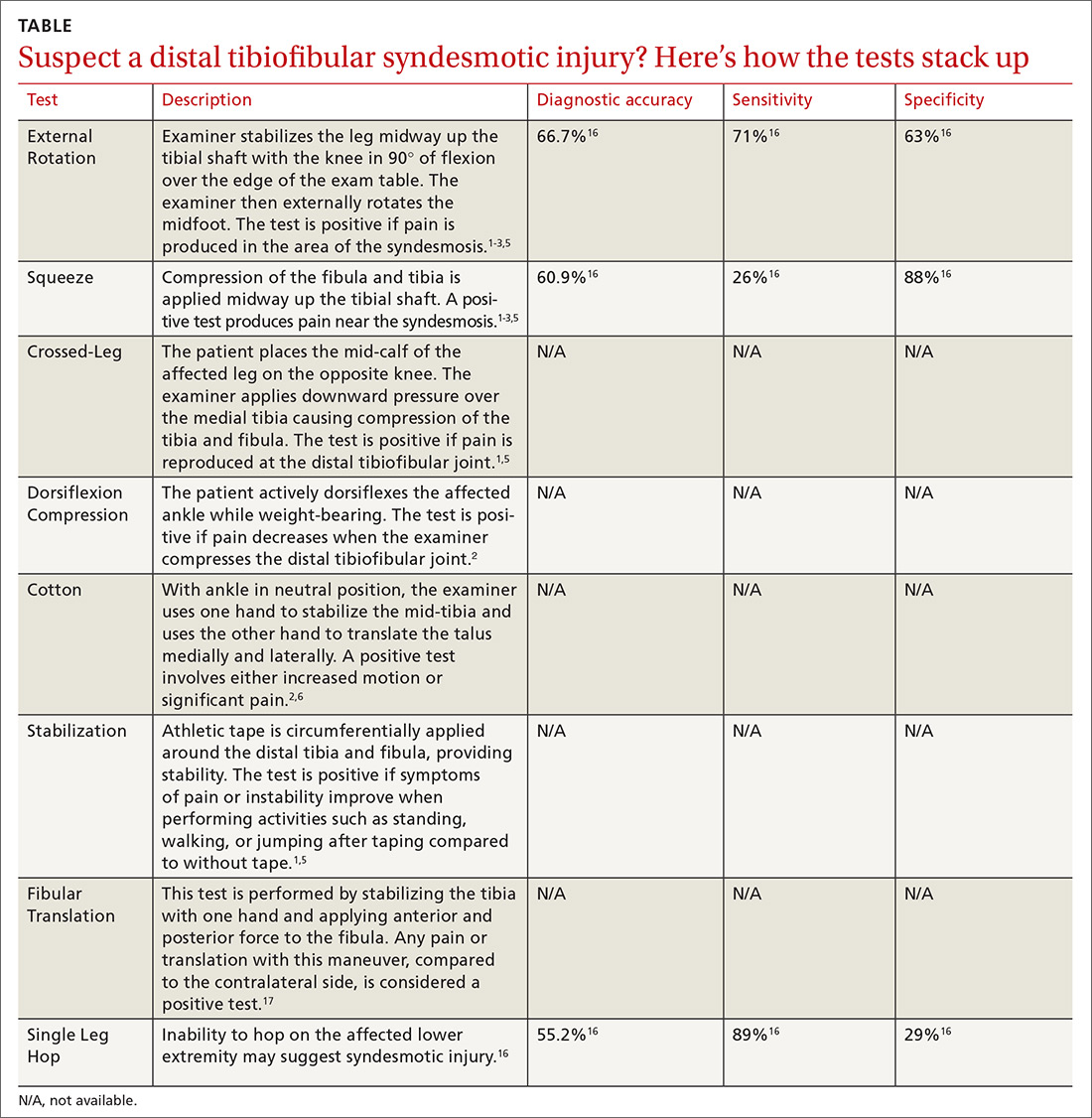
Multiple tests are available to investigate the possibility of a syndesmotic injury and to assess return-to-sport readiness, including the External Rotation Test, the Squeeze Test, the Crossed-Leg Test, the Dorsiflexion Compression Test, the Cotton Test, the Stabilization Test, the Fibular Translation Test, and the Single Leg Hop Test (see TABLE1-3,5,6,16,17). The External Rotation Test is noted by some authors to have the highest interobserver reliability, and is our preferred test.2 The Squeeze Test also has moderate interobserver reliability.2 There is a significant degree of variation among the sensitivity and specificity of these diagnostic tests, and no single test is sufficiently reliable or accurate to diagnose a syndesmotic ankle injury. Therefore, it is recommended to use multiple physical exam maneuvers, the history and mechanism of injury, and findings on imaging studies in conjunction to make the diagnosis of a syndesmotic injury.1,16
Imaging: Which modes and when?
The initial workup should include ankle x-rays when evaluating for the possibility of a distal tibiofibular syndesmosis injury. While the Ottawa Ankle Rules are helpful in providing guidance with regard to x-rays, suspicion of a syndesmotic injury mandates x-rays to determine the stability of the joint and rule out fracture. The European Society of Sports Traumatology, Knee Surgery and Arthroscopy–European Foot and Ankle Associates (ESSKA-AFAS) recommend, at a minimum, obtaining anteroposterior (AP)- and mortise-view ankle x-rays to investigate the tibiofibular clear space, medial clear space, and tibiofibular overlap.7 Most physicians also include a lateral ankle x-ray.
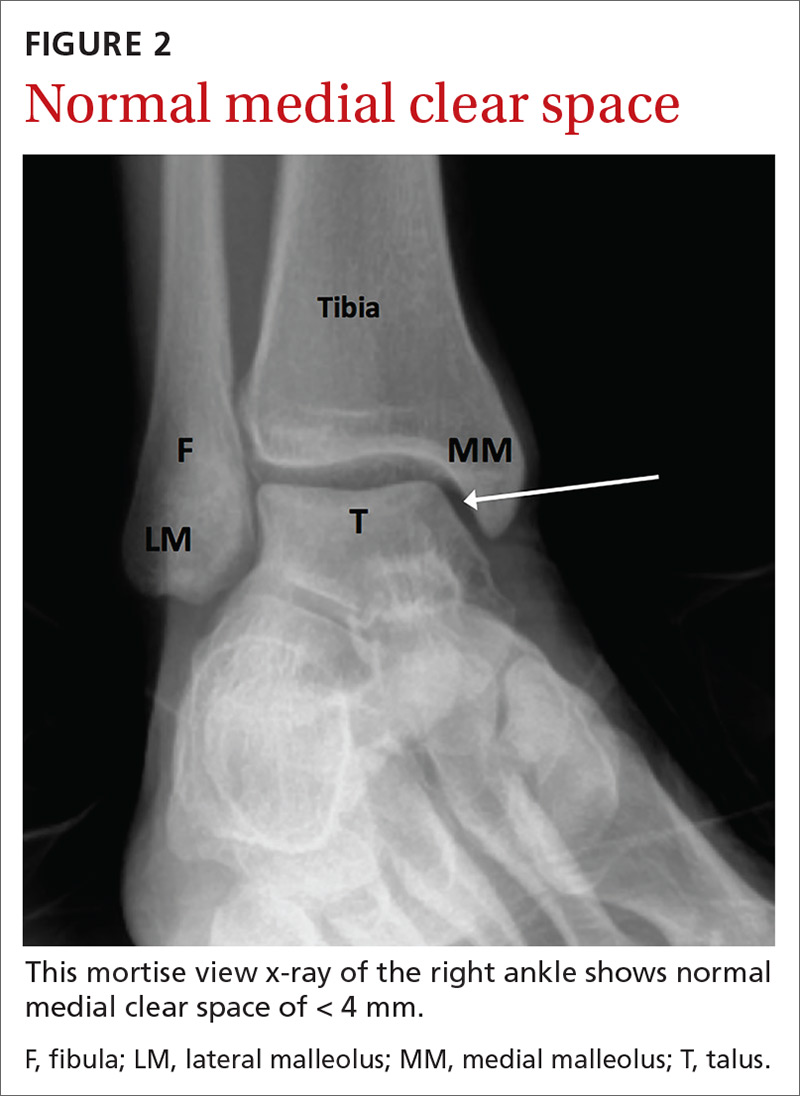
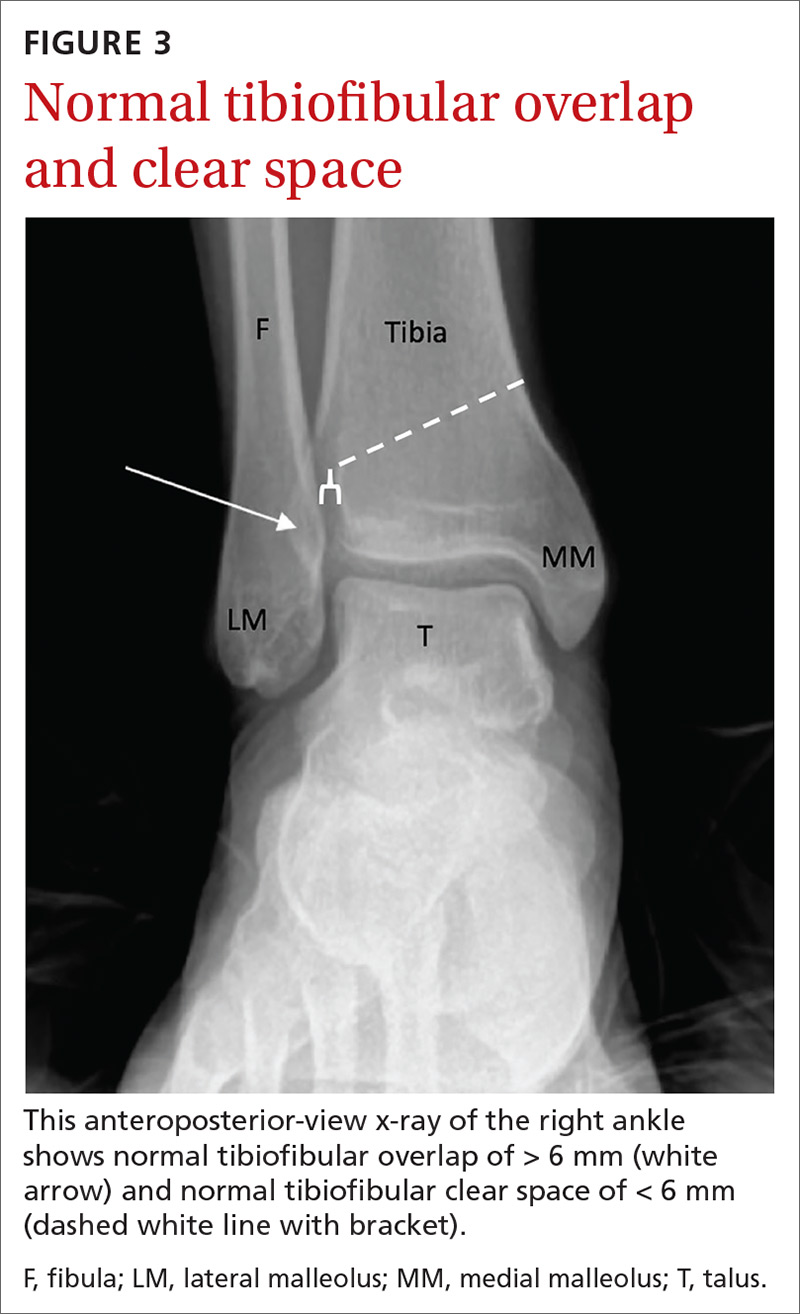
If possible, images should be performed while the patient is bearing weight to further evaluate stability. Radiographic findings that support the diagnosis of syndesmotic injury include a tibiofibular clear space > 6 mm on AP view, medial clear space > 4 mm on mortise view, or tibiofibular overlap < 6 mm on AP view or < 1 mm on mortise view (see FIGURES 2 and 3).1,3,5,8 Additionally, if you suspect a proximal fibular fracture, obtain an x-ray series of the proximal tibia and fibula to investigate the possibility of a Maisonneuve injury.1,2,4,11
If you continue to suspect a syndesmotic injury despite normal x-rays, obtain stress x-rays, in addition to the AP and mortise views, to ensure stability. These x-rays include AP and mortise ankle views with manual external rotation of the ankle joint, which may demonstrate abnormalities not seen on standard x-rays. Bilateral imaging can also be useful to further assess when mild abnormalities vs symmetric anatomic variants are in question.1,7
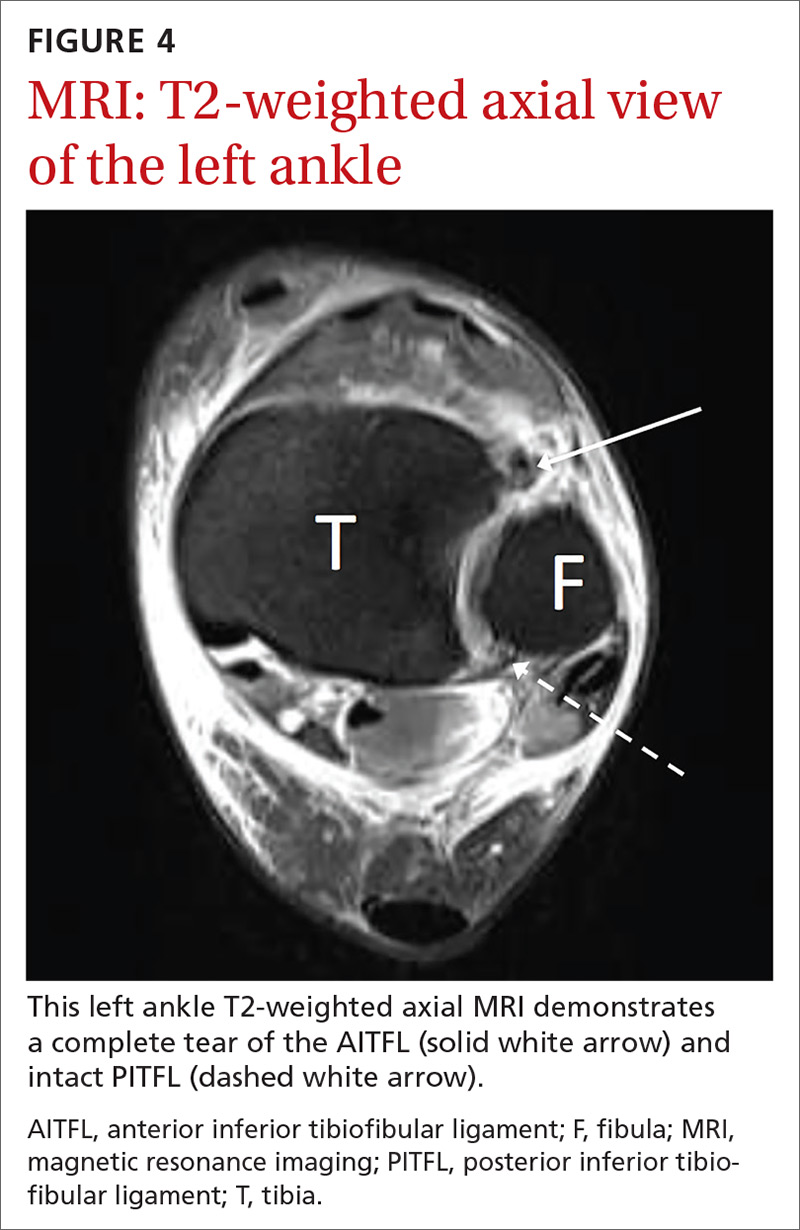
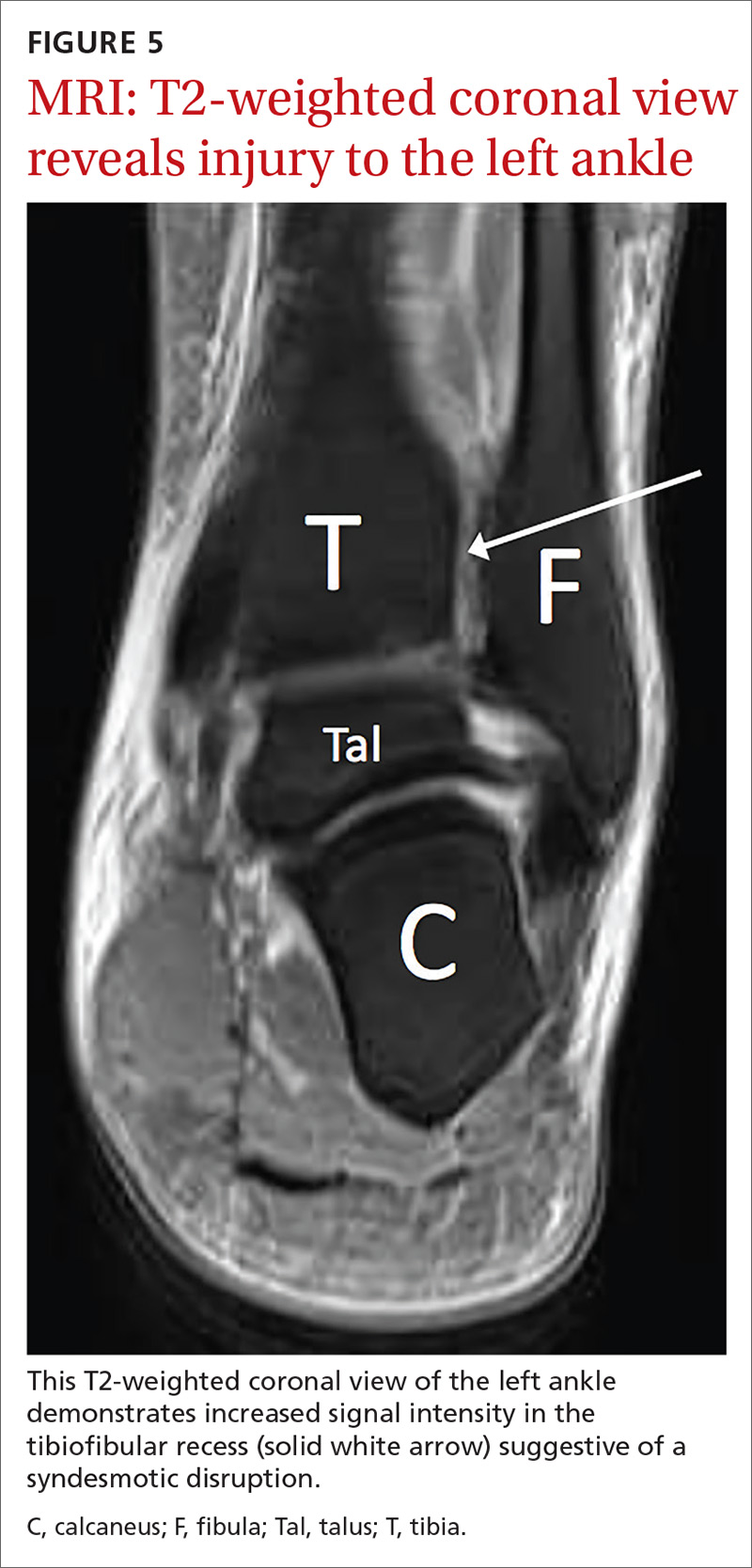
If there is concern for an unstable injury, refer the patient to a foot and ankle surgeon, who may pursue magnetic resonance imaging (MRI) or standing computed tomography (CT).1,2,5,7 MRI is the recommended choice for further evaluation of a syndesmotic injury, as it is proven to be accurate in evaluating the integrity of the syndesmotic ligaments (see FIGURES 4 and 5).18 MRI has demonstrated 100% sensitivity for detecting AITFL and PITFL injuries, as well as 93% and 100% specificity for AITFL and PITFL tears, respectively.8 A weight-bearing CT scan, particularly axial views, can also be a useful adjunct, as it is more sensitive than standard x-rays for assessing for mild diastasis. Although CT can provide an assessment of bony structures, it is not able to evaluate soft tissue structures, limiting its utility in evaluation of syndesmotic injuries.1,7
Continue to: Although not the standard of care...






