Novel treatments for AKN include laser hair removal, UVB
EXPERT ANALYSIS FROM SDEF LAS VEGAS DERMATOLOGY SEMINAR
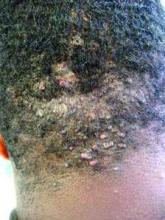
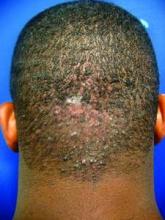
LAS VEGAS – Bothersome and even disfiguring for some, acne keloidalis nuchae (AKN) is a mysterious but common skin disorder mostly affecting men of African descent.
But an accurate clinical diagnosis and a flexible treatment approach can boost treatment success, said Dr. Andrew F. Alexis, chair of the department of dermatology, and director of the Skin of Color Center, Mount Sinai St Luke’s and Mount Sinai Roosevelt, New York.
Speaking at the Skin Disease Education Foundation’s annual Las Vegas dermatology seminar, Dr. Alexis that the diagnosis can be made clinically, without the need for biopsies or skin scrapings. The condition is characterized by fibrotic, follicular papules, usually at the nape of the neck and on the occipital scalp. However, in more severe cases, the papules coalesce into a larger plaque. Occasionally, the characteristic scarring alopecia and keloidlike papules can be seen more toward the vertex of the scalp.
“We don’t really, truly know what the etiology of acne keloidalis nuchae is,” said Dr. Alexis, noting that many etiologies have been proposed. Some say it’s an epithelial elimination disorder, or a variant of lichen simplex chronicus. Many lay people may feel this is an ingrown hair disorder, but histopathologic studies have refuted this theory. These studies have also found no evidence of bacterial overgrowth in affected areas.
A newer and leading hypothesis is that AKN’s primary mechanism is fibrosis secondary to a mechanically induced folliculitis. At the very least, mechanical forces, even if they don’t cause the disorder, “certainly can exacerbate acne keloidalis nuchae, and short haircuts using electrical clippers may be a factor,” Dr. Alexis said. Support for this hypothesis can be found in two South African cross-sectional studies of nearly 2,000 men and boys: 86% of those with AKN reported receiving short haircuts with clippers. Among the adults reporting at least one episode of bleeding during a haircut, the odds ratio for having AKN was 3.45 (Int J Dermatol. 2011 Oct;50[10]:1212-6).
Therapy is multimodal, with some behavioral components, including avoidance of mechanical factors that can exacerbate AKN. In addition to low haircuts, tight-fitting caps and picking or scratching at the papules can worsen the condition.
Few studies exist to support one treatment regime over another for AKN, Dr. Alexis said. One small open label study of 20 individuals evaluated clobetasol 0.05% foam twice daily for two cycles of 2 weeks on and 2 weeks off treatment. Patients with persistent disease were then stepped down to 2 weeks of betamethasone valerate 0.12% foam twice daily. Overall, the mean papule/pustule count dropped by more than half, from 25 at baseline to 10 at 12 weeks, Dr. Alexis said (Cutis. 2005;75:317-21).
For larger papules and coalescent plaques, Dr. Alexis recommends intralesional triamcinolone acetonide at a concentration of 20-40mg/mL. “Don’t undertreat” and be sure to inject into, rather than under the lesion, he said. Concomitant topical class 1 or class 2 corticosteroids, such as clobetasol or fluocinonide, can be used along with injections. Addition of a topical antibiotic such as clindamycin can also accelerate resolution in his anecdotal experience.
Further recommendations based on practice experience include once-daily chlorhexidine washes of the affected area, as well as the addition of an oral tetracycline, such as doxycycline, when pustules are present or with more severe cases, Dr. Alexis said.
For some severely affected patients, surgical therapy may become the best treatment option. “You can inject all day long and still have disfiguring keloidlike plaque” in some patients with severe disease, he noted. Case series of both primary closure and healing by secondary intention have both shown good results. “Whichever camp you belong to, the key is to use a horizontal ellipse that includes the posterior hairline, and the depth of the excision must be down to the dermal-subcutaneous junction,” he said.
More recently, laser hair removal has been studied as a treatment alternative for AKN, Dr. Alexis pointed out. In a pilot study of 16 patients with AKN who received five sessions of laser hair removal, all had a marked reduction in papules and pustules at one year of follow-up (Eur J Dermatol. 2012 Sep-Oct;22[5]:645-50).
Another novel treatment approach used targeted UVB light with good results in a small split-scalp study. Pathology suggested the targeted skin was undergoing active matrix remodeling as a result of the UVB therapy (Br J Dermatol. 2014 Nov;171[5]:1156-63).
Dr. Alexis disclosed that he has received grants and research support from Allergan and Novartis, and speaker honoraria from Cipla. He has received consulting fees from Acclaris Therapeutics, Allergan, Amgen, Anacor, Bayer, Galderma, Johnson & Johnson, Leo, L’Oreal, Roche, Schick, Suneva, and Valeant.