Blood smear analysis in babesiosis, ehrlichiosis, relapsing fever, malaria, and Chagas disease
ABSTRACTBlood smear analysis is especially useful for diagnosing five infectious diseases: babesiosis, ehrlichiosis, relapsing fever due to Borrelia infection, malaria, and American trypanosomiasis (Chagas disease). It should be performed in patients with persistent or recurring fever or in those who have traveled to the developing world or who have a history of tick exposure, especially if accompanied by hemolytic anemia, thrombocytopenia, or hepatosplenomegaly.
KEY POINTS
- In the United States, malaria and American trypanosomiasis principally affect travelers from the developing world.
- Babesiosis, ehrlichiosis, and relapsing fever are transmitted by ticks and may produce thrombocytopenia and elevation of liver enzyme levels.
- Malaria and babesiosis cause hemolytic anemia and may be associated with hepatomegaly and splenomegaly.
- Recurring fever is typical of malaria and Borrelia infection.
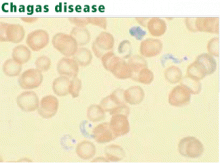
AMERICAN TRYPANOSOMIASIS (CHAGAS DISEASE)
American trypanosomiasis is a zoonotic, protozoal disease caused by Trypanosoma cruzi.
The parasite is transmitted by bloodsucking triatomine insects, or “kissing bugs.”63 These insects favor mud-brick and clay houses, where they live in wall cracks, under furniture, and behind pictures. The insects acquire the organism by feeding on infected animals or on humans that have circulating trypomastigotes. The organisms then multiply in the gut of the insects and are transmitted to a second vertebrate host as the insect defecates following a blood meal. The parasite then enters the body through the skin, conjunctivae, or mucous membranes. After entering the body, the parasite disseminates through the bloodstream, invading many cell types, especially muscle and nerve.
American trypanosomiasis occurs in Central and South America, Mexico, and the southern United States. Between 16 and 18 million people are infected with the parasite, and nearly 50,000 die annually, usually from cardiac complications. Once confined to rural areas, the disease is now common in cities. The majority of reported cases come from Brazil. Only a few cases have been reported in the United States, but an estimated 50,000 to 100,000 immigrants are thought to be infected.64–68
Transmission of the parasite may also occur with blood transfusion, with organ transplantation, and congenitally.63,69,70 An increase in transfusion-related cases is expected in the United States because of an influx of migrant workers from Mexico and Central America.
Acute phase ranges from asymptomatic to multiorgan involvement
Most infected people are asymptomatic carriers. Only 1% become acutely ill, but up to a third of those infected may develop chronic symptoms decades later. Acute Chagas disease, usually seen in children, is characterized by fever, malaise, and anorexia, often accompanied by vomiting, diarrhea, and rash.64,71,72 The heart, liver, spleen, and lymph nodes become enlarged. A red and indurated nodule or furuncle (chagoma) appears at the inoculation site. If inoculation occurs across the conjunctivae, painless edema of the palpebrae and periocular tissues may be observed (Romaña sign). Generalized lymphadenopathy and hepatosplenomegaly may also be seen.
Myocarditis and meningoencephalitis occur in some cases of acute Chagas disease. Myocardial inflammation may extend to the pericardium, causing pericardial effusion, and to the endocardium, causing thrombus formation. All cardiac chambers become enlarged and the conduction system is disrupted.73 Brain damage from meningoencephalitis usually occurs in infants and young children, and may result in death.
This acute phase lasts 4 to 8 weeks and is characterized by profound parasitemia, tissue invasion, and inflammation. Following the acute phase, an asymptomatic latent or indeterminate phase lasting 10 to 40 years occurs.74 Less than half of those in clinical latency enter a chronic phase of disease.
Severe chronic phase may occur decades later
The chronic phase, which occurs years to decades after the initial infection, is characterized by cardiac, esophageal, and colonic enlargement. Cardiac involvement is associated with congestive heart failure, arrhythmias, and cardiac arrest. Intracardiac thrombi may embolize, causing systemic and pulmonary infarctions.71–73,75 Enlargement of the esophagus is associated with dysphagia, chest pain, weight loss, and sometimes perforation or aspiration-related pneumonitis. Colonic enlargement may result in constipation, abdominal distention, and intestinal obstruction. Sometimes, the small bowel, ureters, and bronchi become dilated as well. These findings are the result of low-grade parasitemia, tissue inflammation, and immune-mediated disruption of the microvasculature.71,76
Diagnosis: Protozoa evident in acute phase
Serologic tests are most useful for diagnosing chronic Chagas disease.77 The organism can be identified by polymerase chain reaction, but the sensitivity of this test is highly variable.
Treatment reduces symptoms
Two drugs are used to treat American trypanosomiasis. Nifurtimox (Lampit) reduces symptom duration and severity, as well as mortality rates, in acute and congenital Chagas disease; however, fewer than 75% of patients have a parasitologic cure, and adverse effects limit tolerability.78 Benznidazole (Rochagan, Radanil) has an efficacy similar to that of nifurtimox and is considered the drug of choice in Latin America. These drugs are not commercially available in the United States. Therapy may help during the indeterminate phase but is rarely effective for chronic Chagas disease. Treatment of Chagas disease with triazoles is under evaluation.