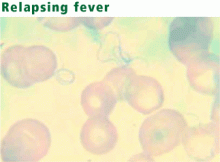
Blood smear analysis in babesiosis, ehrlichiosis, relapsing fever, malaria, and Chagas disease
ABSTRACTBlood smear analysis is especially useful for diagnosing five infectious diseases: babesiosis, ehrlichiosis, relapsing fever due to Borrelia infection, malaria, and American trypanosomiasis (Chagas disease). It should be performed in patients with persistent or recurring fever or in those who have traveled to the developing world or who have a history of tick exposure, especially if accompanied by hemolytic anemia, thrombocytopenia, or hepatosplenomegaly.
KEY POINTS
- In the United States, malaria and American trypanosomiasis principally affect travelers from the developing world.
- Babesiosis, ehrlichiosis, and relapsing fever are transmitted by ticks and may produce thrombocytopenia and elevation of liver enzyme levels.
- Malaria and babesiosis cause hemolytic anemia and may be associated with hepatomegaly and splenomegaly.
- Recurring fever is typical of malaria and Borrelia infection.
RELAPSING FEVER
Relapsing fever is an acute febrile illness caused by spirochetes of the genus Borrelia. The disease has two forms: tick-borne, in which human infection is zoonotic, and louse-borne, in which humans are the only known reservoir of infection.32
Few tick-borne cases in the United States
Tick-borne disease is caused by many species of Borrelia. Those found in the United States occur in the western mountains and high deserts and plains of the Southwest.33 Fewer than 30 cases of tick-borne relapsing fever are diagnosed in the United States annually.
Tick-borne relapsing fever is transmitted by soft-bodied argasid ticks (Ornithodoros genus), which feed for less than an hour (usually at night) and can survive for years without a blood meal. They stay close to human and animal habitations. Exposure often occurs in cabins, under buildings, in caves, near woodpiles, and in rooms shared with animals. Rodents are the primary animal reservoir. In contrast, most other tick-borne diseases—babesiosis, ehrlichiosis, Lyme disease, Rocky Mountain spotted fever, Colorado tick fever—are transmitted by hard-bodied ixodid ticks, which live in brush and forested areas and attach to passersby, on whom they feed for days if not removed.34–36
Louse-borne disease is endemic in Africa
Louse-borne relapsing fever is caused by a single species, B recurrentis, endemic in Ethiopia and Sudan. It may occur sporadically or in epidemics. War, famine, and mass migrations predispose to epidemics with death rates ranging from 30% to 70% if untreated.37,38 Disease is spread between humans by the human body louse (Pediculus humanus).
Relapsing high fevers
The clinical manifestations of tick-borne and louse-borne relapsing fever are similar, although louse-borne relapsing fever often has a longer incubation period and a longer duration of illness. Bacteremia is heralded by the acute onset of high fever (usually above 39°C [102.2°F]), accompanied by headache, nausea, myalgias, and arthralgias. On average, clinical illness remits in 3 days in tick-borne relapsing fever, but may take 5 to 6 days in louse-borne relapsing fever. Physical findings may include altered sensorium, petechiae, hepatosplenomegaly, and conjunctival suffusion. The fever culminates in a “crisis,” characterized by rigors and a precipitous rise in temperature, pulse, and blood pressure. This is followed by defervescence, diaphoresis, and hypotension. The risk of death is highest during this period and immediately afterwards.
With resolution of the bacteremia, an afebrile period ensues, lasting 4 to 14 days. Fever then recurs, although usually milder, again associated with bacteremia. On average, people with tick-borne relapsing fever have three febrile relapses; those with louse-borne relapsing fever have one.39 Relapse occurs because of antigenic variation, in which a major surface antigen of the spirochete is changed to evade the host’s immune system.40–42
Borrelia may invade organs and the nervous system
With each episode of bacteremia, spirochetes may penetrate the brain, heart, liver, eye, or inner ear. Involvement of the central nervous system is more common with tick-borne than with louse-borne relapsing fever. Nervous system involvement may include facial palsy, myelitis, radiculopathy, aphasia, hemiplegia, stupor, or coma.43,44 Myocarditis, common in both forms of relapsing fever, portends a poor prognosis.45 Invasion of the eye or ear may result in visual impairment or dizziness. Bleeding disorders, manifested by epistaxis, petechiae, and ecchymoses, are typical of louse-borne disease and may be associated with low-grade disseminated intravascular coagulation.46 Splenomegaly is more common in louse-borne than in tick-borne disease.
Auxiliary test findings
Laboratory findings include normocytic anemia, leukocytosis, and thrombocytopenia. Liver enzyme levels may be elevated and coagulation tests may be prolonged. Patients with cardiac involvement may have a prolonged QTc interval. Cardiomegaly and pulmonary edema may be seen on chest radiography. The cerebrospinal fluid in patients with neurologic involvement has a mononuclear pleocytosis and a mildly elevated protein concentration.
Suspect if recurrent fever in endemic areas
Treatment
Relapsing fever can be successfully treated with tetracycline, penicillin, or erythromycin.47 The preferred regimen for a nonpregnant adult with louse-borne relapsing fever is a single 0.5-g dose of tetracycline. In tick-borne relapsing fever, 0.5 g of tetracycline four times daily for 5 to 10 days is recommended. Meningitis or encephalitis is usually treated with parenteral penicillin or ceftriaxone (Rocephin). The death rate in treated disease is usually less than 5%.39 Treatment can induce a Jarisch-Herxheimer reaction (rigors and hypotension, resembling a febrile crisis), and patients must be watched closely for the first 4 hours after the antibiotic is given. Avoiding ticks and practicing good personal hygiene to prevent acquiring lice are the major preventive strategies.