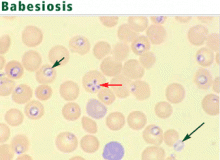
Blood smear analysis in babesiosis, ehrlichiosis, relapsing fever, malaria, and Chagas disease
ABSTRACTBlood smear analysis is especially useful for diagnosing five infectious diseases: babesiosis, ehrlichiosis, relapsing fever due to Borrelia infection, malaria, and American trypanosomiasis (Chagas disease). It should be performed in patients with persistent or recurring fever or in those who have traveled to the developing world or who have a history of tick exposure, especially if accompanied by hemolytic anemia, thrombocytopenia, or hepatosplenomegaly.
KEY POINTS
- In the United States, malaria and American trypanosomiasis principally affect travelers from the developing world.
- Babesiosis, ehrlichiosis, and relapsing fever are transmitted by ticks and may produce thrombocytopenia and elevation of liver enzyme levels.
- Malaria and babesiosis cause hemolytic anemia and may be associated with hepatomegaly and splenomegaly.
- Recurring fever is typical of malaria and Borrelia infection.
Blood smear analysis, while commonly used to evaluate hematologic conditions, is infrequently used to diagnose infectious diseases. This is because of the rarity of diseases for which blood smear analysis is indicated. Consequently, such testing is often overlooked when it is diagnostically important.
Nonspecific changes may include morphologic changes in leukocytes and erythrocytes (eg, toxic granulations, macrocytosis).1 And with certain pathogens, identifying organisms in a peripheral blood smear allows for a rapid diagnosis.
This paper discusses the epidemiology, clinical manifestations, laboratory findings, and management of five infectious diseases in which direct visualization of the organism in the blood plays a major diagnostic role. Our intent is to summarize the clinical findings that should prompt blood smear analysis so that these uncommon conditions are not overlooked.
BABESIOSIS
Babesiosis, a tick-borne protozoal disease, occurs principally in the United States and Europe. Of the more than 100 species of Babesia, two account for almost all human disease: B microti and B divergens.
Both species are transmitted by Ixodes ticks, although patients often do not recall being bitten. The disease may rarely complicate blood transfusion. Most cases occur from May to September, when tick exposure is highest. The incubation period varies from 1 to 4 weeks.
Common in the Northeast, usually asymptomatic
B microti infection occurs predominantly in the United States. Rodents, especially the white-footed mouse, are the principal reservoir.2,3 Endemic areas, where seropositivity rates range from 4% to 21%, include the coastal areas and islands off of Massachusetts, particularly Cape Cod, Nantucket, and Martha’s Vineyard; the islands near New York City, especially Long Island, Shelter Island, and Fire Island; Block Island, off the coast of Rhode Island; and certain areas in Connecticut.4 WA-1, a species that is morphologically identical to B microti, is emerging in California and Washington.5,6
Infection with B microti is usually asymptomatic. Elderly and immunosuppressed people, especially those without a spleen or with impaired cellular immunity, are more likely to become ill. Symptoms, including fever, malaise, headache, nausea, and generalized aching, may last weeks to months.
About one-fourth of patients with babesiosis are coinfected with the Lyme disease bacterium (Borrelia burgdorferi) and often have more severe illness.3
Hepatomegaly, splenomegaly, jaundice, and dark urine are common findings in patients with symptoms. Severe hemolysis, often accompanied by thrombocytopenia, leukopenia, and atypical lymphocytosis, is more common in high-risk patients. Hepatic transaminases may be elevated. Urinalysis may show proteinuria and hemoglobinuria. Acute respiratory distress syndrome has been reported in severe cases.7–10
B divergens infection: A serious but rare disease seen in Europe
B divergens is found mainly in Europe. Altogether, fewer than 50 cases of infection have been reported in France, Spain, Germany, Great Britain, Ireland, Yugoslavia, and the former Soviet Union.11,12 Cattle are the principal reservoir of infection.
Infection with B divergens causes a rare but devastating disease mainly in asplenic people, usually resulting in coma and death. No cases of subclinical infection have been reported. The clinical course is fulminant, and hemolytic anemia is common.2,3
Suspect babesiosis in endemic areas in cases of prolonged ‘flu’
Babesiosis should be considered when a patient residing in or traveling from an endemic area presents with a prolonged flu-like illness and hemolysis, with or without organomegaly and jaundice.
The protozoa may resemble the rings of malaria parasites. Distinguishing traits include exoerythrocytic organisms; the absence of pigmented granules in infected red blood cells; and a “maltese cross,” a rare pattern produced by tetrads of Babesia merozoites.13 An infected erythrocyte may contain up to eight parasites.
Serologic and polymerase chain reaction tests are useful when the organism is not visible.14,15
Treat patients with severe disease
Most patients with B microti infection have a mild illness that resolves without treatment. Treatment is recommended for those with severe infection and in those with high-level parasitemia. Agents with consistent activity against B microti include clindamycin (Cleocin), azithromycin (Zithromax), ato-vaquone (Mepron), doxycycline (Vibramycin), and quinine (Quinamm). Combination therapy with either clindamycin and quinine or azithromycin and atovaquone is recommended. B divergens infection has been successfully treated with a combination of clindamycin, quinine, and exchange transfusion.16