Red eye for the internist: When to treat, when to refer
ABSTRACTWhen a patient presents with redness in the eye, the cause needs to be diagnosed quickly. Some of the diseases that cause redness in the eye can be initially managed by an internist, but others call for quick referral to an ophthalmologist. This article reviews the spectrum of conditions manifesting as a red eye, emphasizing how to differentiate between the benign and the vision-threatening.
KEY POINTS
- Blepharitis, conjunctivitis, corneal abrasion, dry eye, and subconjunctival hemorrhage are benign and can usually be managed initially by an internist, although referral is usually indicated if symptoms persist or progress.
- Patients with corneal bacterial infection, uveitis, scleritis, or acute narrow-angle glaucoma need immediate referral to an ophthalmologist, as do most patients with a red eye who use contact lenses, who have had trauma to the eye, or who have vision changes, severe pain, nausea, vomiting, severe headache, marked purulent discharge, or abnormalities in the cornea or anterior segment.
- Because it is difficult to distinguish between infectious and noninfectious conditions, and because treating infections with corticosteroids alone can have grave consequences, we recommend that internists generally not use topical corticosteroids to treat eye symptoms.
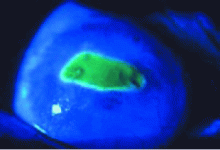
Corneal abrasion
Treat with topical antibiotics to prevent infection until the corneal epithelium has healed.16 However, most abrasions heal rapidly without sequelae because epithelial cells proliferate and migrate rapidly.
Refer if symptoms persist for longer than 48 hours or if pain suddenly worsens after the healing process has started.
Pingueculae and pterygia
A pinguecula is a small, yellow, benign growth on the nasal and temporal conjunctiva near the limbus. A pterygium is a wing-shaped band of fibrovascular tissue originating on the conjunctiva and extending onto the cornea. Both conditions are idiopathic but are believed to arise from chronic sun exposure.
Pingueculae can become inflamed and can cause eye redness and irritation. Treat conservatively with lubrication and judicious use of topical steroids; if irritation persists, pingueculae can be surgically removed.17
Episcleritis
Episcleritis is inflammation of the superficial vessels of the episclera, the connective tissue layer between the conjunctiva and the sclera. It presents with a sectoral area of redness (although it can be diffuse) and is not typically associated with pain, vision changes, or discharge. The condition tends to be recurrent and unilateral, but it can be bilateral or alternating. The underlying pathophysiology is believed to be autoimmune, although a systemic evaluation is often unrevealing.
Episcleritis is treated with topical corticosteroids or oral nonsteroidal anti-inflammatory drugs (NSAIDs); refer if the disease persists or recurs.
Thyroid-related eye disease
Thyroid-associated ophthalmopathy, an autoimmune process, usually occurs in patients with known thyroid disease, although it may develop before other systemic symptoms. Symptoms can include irritation and double vision. Signs are bulging eyes, eyelid retraction, chemosis (swelling of the conjunctiva around the cornea), conjunctival injection, periorbital edema, and limited ocular motility.
Although most cases can be managed with lubrication, vision loss may occur due to corneal exposure or compressive optic neuropathy. Patients with significant visual changes should be referred immediately to an ophthalmologist.18
CONDITIONS NEEDING REFERRAL WITHIN 48 HOURS
Scleritis
Scleritis is inflammation of the deep vessels within the episclera. The red color appears more pronounced and more purplish than in episcleritis and does not blanch after phenylephrine drops are given. The eye is tender to palpation and may be painful enough to awaken the patient from sleep. Vision is not typically affected unless the cornea, anterior chamber, or posterior segment is involved.
Half of patients who have scleritis have an associated systemic disease, eg, rheumatoid arthritis (most common), other autoimmune diseases (Wegener granulomatosis, relapsing polychondritis, inflammatory bowel disease), or infections such as tuberculosis and syphilis.
Therefore, one should search for an underlying systemic condition with a thorough history, physical examination, chest radiography (for sarcoidosis and tuberculosis), and laboratory testing: antineutrophil cytoplasmic antibody test, fluorescent treponemal antibody absorption test, Lyme antibody test, (if in an endemic area), urinalysis, a complete blood count, and a comprehensive metabolic panel.
However, patients should be promptly referred to an ophthalmologist for diagnosis and management. Treatment can depend on the underlying diagnosis, and is often guided by the status of the scleritis. Mild scleritis can be treated with oral NSAIDs; more severe disease should be treated with oral corticosteroids with or without corticosteroid-sparing agents such as methotrexate, mycophenolate (CellCept), cyclophosphamide (Cytoxan, Neosar),19,20 or tumor necrosis factor-alpha antagonists such as infliximab (Remicade) or etanercept (Enbrel).21