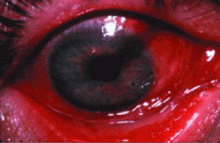
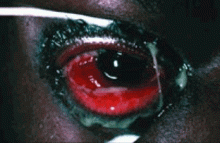
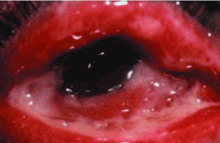
Red eye for the internist: When to treat, when to refer
ABSTRACTWhen a patient presents with redness in the eye, the cause needs to be diagnosed quickly. Some of the diseases that cause redness in the eye can be initially managed by an internist, but others call for quick referral to an ophthalmologist. This article reviews the spectrum of conditions manifesting as a red eye, emphasizing how to differentiate between the benign and the vision-threatening.
KEY POINTS
- Blepharitis, conjunctivitis, corneal abrasion, dry eye, and subconjunctival hemorrhage are benign and can usually be managed initially by an internist, although referral is usually indicated if symptoms persist or progress.
- Patients with corneal bacterial infection, uveitis, scleritis, or acute narrow-angle glaucoma need immediate referral to an ophthalmologist, as do most patients with a red eye who use contact lenses, who have had trauma to the eye, or who have vision changes, severe pain, nausea, vomiting, severe headache, marked purulent discharge, or abnormalities in the cornea or anterior segment.
- Because it is difficult to distinguish between infectious and noninfectious conditions, and because treating infections with corticosteroids alone can have grave consequences, we recommend that internists generally not use topical corticosteroids to treat eye symptoms.
Conjunctivitis
Conjunctivitis involves hyperemia and edema of the bulbar conjunctiva (the part of the conjunctiva covering the eyeball) along with papillary and follicular changes of the palpebral conjunctiva (the inner layer of the eyelids).
Conjunctivitis can be viral, bacterial, or allergic, or due to wearing contact lenses; the cause can usually be distinguished by the history and physical examination.
Viral conjunctivitis, usually caused by an adenovirus, is more common than bacterial conjunctivitis in adults. The patient typically has had a recent upper respiratory tract infection or was exposed to conjunctivitis.
Treat supportively with cool compresses. Symptoms often worsen for a few days, then slowly improve over 1 to 2 weeks.
Viral conjunctivitis is contagious for 2 weeks after the second eye becomes involved, and good hygiene must be maintained to avoid spreading it to coworkers and family members. Those who work with the public, in schools, or in health-care facilities should be given a 2-week leave of absence to avoid spreading the infection to others.
Refer to an ophthalmologist if symptoms do not resolve in 2 weeks, as certain subtypes of adenovirus can cause prolonged symptoms with corneal involvement.7
Treat bacterial conjunctivitis empirically with antibiotic eyedrops (eg, a fluoroquinolone, a polymyxin, or sulfacetamide—several brands available) four times daily for 7 to 10 days, even though most cases are self-limited and do not result in complications. Cultures can be obtained, especially if the patient is in the hospital8 or if the conjunctivitis persists after 1 week of antibiotic therapy.
Refer patients with vision changes or who do not improve after 1 week of treatment.9,10
Treat aggressively with both a topical antibiotic (usually a fluoroquinolone) four times daily and a systemic antibiotic such as ceftriaxone (Rocephin) given as a single 1-g intramuscular injection.11,12 Because one-third of patients with gonorrheal infection also have chlamydial infection, treatment for both diseases is frequently prescribed.
Chlamydial infection, a sexually transmitted disease, can cause chronic follicular conjunctivitis. The genital tract infection may be asymptomatic. Diagnosis is made by swabbing the conjunctiva to culture for Chlamydia trachomatis. Treat systemically with either azithromycin (Zithromax) in a single 1-g oral dose or a 10–14-day course of either doxycycline (Doryx) 100 mg twice daily or erythromycin 250 mg four times daily.13
Allergic conjunctivitis is characterized by bilateral itching that worsens with scratching. Discharge is variable but is usually clear or white and stringy. Many patients have a history of seasonal or perennial allergies.
Remove offending allergens, if possible. Topical mast cell stabilizers and antihistamines relieve symptoms but may exacerbate underlying dry eye symptoms. A combined mast cell stabilizer and antihistamine such as olopatadine (Patanol), ketotifen (Zaditor), or epinastine (Elestat) can be given twice daily.14,15 Artificial tears can treat the associated dryness.
Topical corticosteroids may be used to treat an acute, severe episode but should not be used long-term. In fact, because it is difficult to differentiate between infectious and noninfectious eye conditions, and because treating some infections with corticosteroids by themselves can have grave consequences, we recommend that internists generally refrain from using them.
Oral antihistamines may relieve symptoms but are usually less effective than topical therapy.
Refer if symptoms do not resolve after 2 weeks of topical treatment.
Giant papillary conjunctivitis, most often seen in patients who wear soft contact lenses, presents with bilateral contact lens intolerance, itching, mucous discharge, and giant papillae on the upper palpebral conjunctiva.
Again, promptly refer any patient who wears contact lenses and presents with a red eye, owing to the risk of a vision-threatening corneal infection. The patient should stop wearing contact lenses for about 1 month, after which he or she can be refitted with new soft or gas-permeable lenses and taught better lens hygiene. During an acute episode, topical mast cell stabilizers are helpful for mild irritation, and topical steroids (prednisolone phosphate 1%) are helpful for more severe irritation. Topical steroids should never be used on a long-term basis because of possible adverse effects. Artificial tears can be used for dryness.15