Evaluation and management of pituitary incidentalomas
ABSTRACTA surprising number of apparently healthy people harbor unsuspected pituitary tumors, which are being discovered incidentally on computed tomography (CT) or magnetic resonance imaging (MRI) performed for other reasons. The majority can be safely observed; for others, medical therapy or surgical resection is necessary. In this article we outline our approach.
KEY POINTS
- Two key questions that must be answered when a pituitary incidentaloma is discovered are whether it is hormonally active and whether it is causing a mass effect (eg, a visual field defect due to pressure on the optic chiasm).
- Incidentalomas that are not hormonally active and that are not causing a mass effect can generally be managed by watchful waiting.
- Hormonally active prolactin-secreting tumors can be treated with dopamine agonists. Other hormonally active tumors and those that are causing a mass effect should be surgically removed.
- The risks of further tumor growth and of pituitary apoplexy are higher in tumors that are larger when discovered.
Cranial neuropathy
Abnormal eye movements, which may cause diplopia, result from extension of a pituitary tumor into one or both cavernous sinuses. Compression of the third (occulomotor, the cranial nerve most often affected), fourth (trochlear), and sixth (abducens) cranial nerves leads to eye movement deviations as well as eyelid ptosis due to third nerve dysfunction. Cranial neuropathy most commonly occurs in the setting of pituitary apoplexy (see below) but may occur without it.
Headache
Headache can be associated with pituitary tumors, but the underlying pathophysiology remains uncertain. Possible mechanisms include structural causes such as dural stretching or cavernous sinus invasion.17 Other possible mechanisms are an increase in the intrasellar pressure and tumor activity.15,18 The link between headache and tumor activity is supported by the observation that headaches resolve in some patients with acromegaly shortly after they start taking somatostatin analogues.19
Migraine may be the most common type of headache reported in patients with pituitary adenomas; however, short-lasting unilateral neuralgiform headache with conjunctival injection and tearing (SUNCT) has also been reported.19
Of interest, there seems to be a strong association between pituitary-associated headache and a family history of headache.19 That said, headache is a common symptom in the general population, and establishing a cause-and-effect relationship prior to surgical removal of a pituitary tumor can be challenging. Approximately 50% of patients with headache who undergo an operation for a pituitary tumor have relief after surgery; however, 35% may not have relief, and up to 15% have a worsening of their headaches.19
OUR PATIENT’S HORMONAL EVALUATION
In the patient we described earlier, hormonal evaluation revealed the following:
- Prolactin 12.2 ng/mL (reference range 2–17.4)
- IGF-1 189 ng/mL (114–492)
- Thyrotropin 1.63 μU/mL (0.4–5.5)
- Free thyroxine index 9.5 μg/L (6–11)
- Maximum cortisol during a low-dose ACTH stimulation test 18.4 μg/dL. In short, all her test results were normal.
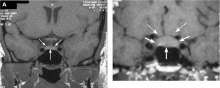
A formal visual field test was not performed, since the pituitary mass did not reach the optic chiasm (Figure 1).
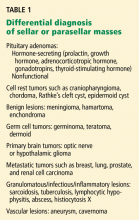
ADENOMAS VS OTHER SELLAR MASSES
In some cases, it may be difficult to distinguish a nonadenomatous lesion from a nonfunctioning pituitary adenoma. However, several endocrine, radiographic, and neurologic features may help to differentiate pituitary tumors from other, less common sellar disorders.20
For instance, diabetes insipidus is extremely rare in patients with pituitary adenomas at presentation without significant suprasellar extension of the tumor. Therefore, its presence strongly suggests a nonpituitary cause such as hypophysitis, sarcoidosis, or a meta-static lesion.21
Some radiographic features that suggest sellar masses other than pituitary tumors include calcifications on CT in patients with craniopharyngiomas and meningiomas or a rapidly enlarging mass with lack of sellar enlargement (sellar remodeling), which suggests a metastatic lesion. While a dural tail sign (a linear enhanced structure or “tail” extending away from the tumor mass along the dural surface) may be seen with some meningiomas, peripheral enhancement of the dura is not specific for meningioma and may be seen with pituitary apoplexy as well.22,23
Cranial neuropathy is less common in patients with pituitary adenomas than in those with nonadenomatous masses (for example a metastasis or a meningioma), although the acute onset of cranial neuropathy often accompanies a hemorrhagic infarction of a preexisting pituitary adenoma (pituitary apoplexy).20
OUR RECOMMENDATIONS
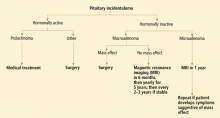
Our approach to a patient with a pituitary incidentaloma is summarized in Figure 4.
If the tumor is hormonally active
Prolactinoma is the exception. For this tumor, dopamine agonists can resolve symptoms and shrink the tumor in most cases. Even in patients with a visual field defect associated with a macroprolactinoma, vision usually improves within days after starting a dopamine agonist, before the tumor has observably shrunk. However, a follow-up visual field test is necessary 2 to 6 weeks after starting therapy to establish that the tumor is responding to therapy; if the tumor does not respond, surgery may be necessary.