Evaluation and management of pituitary incidentalomas
ABSTRACTA surprising number of apparently healthy people harbor unsuspected pituitary tumors, which are being discovered incidentally on computed tomography (CT) or magnetic resonance imaging (MRI) performed for other reasons. The majority can be safely observed; for others, medical therapy or surgical resection is necessary. In this article we outline our approach.
KEY POINTS
- Two key questions that must be answered when a pituitary incidentaloma is discovered are whether it is hormonally active and whether it is causing a mass effect (eg, a visual field defect due to pressure on the optic chiasm).
- Incidentalomas that are not hormonally active and that are not causing a mass effect can generally be managed by watchful waiting.
- Hormonally active prolactin-secreting tumors can be treated with dopamine agonists. Other hormonally active tumors and those that are causing a mass effect should be surgically removed.
- The risks of further tumor growth and of pituitary apoplexy are higher in tumors that are larger when discovered.
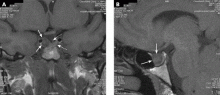
A 39-year-old woman is referred for evaluation of a pituitary mass, which was found on magnetic resonance imaging (MRI) performed because of persistent vertigo. The mass, measuring 1.1 by 1.0 cm, arises from the right portion of the sella turcica and does not reach the optic chiasm (Figure 1). It appears hypointense on MRI and enhances after contrast is given, suggesting it is a pituitary adenoma.
On physical examination she does not have any stigmata of Cushing syndrome or of acromegaly. Her blood pressure is 116/72 mm Hg and her heart rate is regular at 68 beats per minute. Her visual fields are normal as assessed by confrontation, and she has no galactorrhea.
How should this patient be evaluated?
BY DEFINITION, INCIDENTALOMAS ARE UNSUSPECTED
Pituitary “incidentalomas” are, by definition, masses that are discovered by computed tomography (CT) or MRI performed to evaluate unrelated disorders (such as head trauma), for cancer staging, or because of nonspecific symptoms such as dizziness and headache. In some series, headache was the most common reason for imaging studies that led to the discovery of pituitary incidentalomas.1
With more patients undergoing computed tomography (CT) and MRI, more incidentalomas are being discovered. Incidentally discovered pituitary adenomas accounted for 12% of the pituitary tumors in a series of 353 consecutive patients with a presumptive diagnosis of pituitary tumor at one institution over a 14-year period.2 Pituitary masses other than adenomas are discussed later in this paper.
Microadenomas are common, macroadenomas less so
Autopsy studies have revealed pituitary microadenomas (ie, < 10 mm in greatest dimension) in 3% to 27% of patients with no history of pituitary disorders. Macroadenomas (10 mm or larger), on the other hand, are found in fewer than 0.5% of people.3,4 Recently, a study of MRI in 2,000 healthy adult volunteers, age 45 to 97 years, found pituitary macroadenomas in 0.3%.5
Hall et al6 found that 10% of relatively young (< 60 years old) healthy volunteers harbored a pituitary microadenoma on pituitary MRI, but none had a macroadenoma. In a meta-analysis by Ezzat and colleagues,3 adenomas of all sizes were found in 1% to 40% of imaging or postmortem studies (for an average of 16.7%), but macroadenomas were found in only 0.16% to 0.2% of the population.
Although the natural history of pituitary incidentalomas is not well characterized, the numbers suggest that microadenomas rarely grow into macroadenomas.7 Another possibility is that most macroadenomas cause symptoms and therefore come to clinical attention, and thus are not incidentalomas per se.
THE INITIAL EVALUATION: TWO QUESTIONS
The initial approach to a patient with a pituitary incidentaloma should be guided by two questions:
- Is the tumor hormonally active?
- Is it causing a mass effect (ie, is it exerting pressure on adjacent structures)?
IS THE TUMOR HORMONALLY ACTIVE?
A careful history and physical examination may reveal overlooked symptoms or signs of hypersecretion of a specific hormone, which can be evaluated in detail to establish the diagnosis. However, most patients with pituitary incidentalomas have no symptoms, and for them there is no real consensus about the optimal workup strategy.
Prolactin excess
King et al8 calculated that the serum prolactin level is the single most cost-effective screening test for hormonal activity in patients with incidentally discovered pituitary microadenomas. They also suggested, however, that it may be cost-effective to measure multiple hormones in very anxious patients, since a negative test may provide reassurance and improve quality of life.
One should be careful in interpreting elevated prolactin levels in patients with pituitary incidentalomas, since a number of medications (eg, metoclopramide [Reglan], verapamil [Calan], phenothiazines) and disorders (eg, hypothyroidism, cirrhosis, renal failure) can cause mild to moderate elevations of prolactin. In general, a prolactin level of more than 200 ng/mL is almost always diagnostic of prolactinomas. In our experience, a prolactin level above 100 ng/mL is almost always due to a prolactin-secreting pituitary adenoma, except during pregnancy and in some patients who receive antipsychotics or metoclopramide. For these patients, if it is clinically safe to hold or switch medications, retesting after a drug holiday may prove useful and diagnostic.
Growth hormone excess
Growth hormone hypersecretion has been reported in patients with pituitary tumors who have no clinical stigmata of acromegaly.9,10 Moreover, acral changes may not correlate with the metabolic consequences of growth hormone excess.11 In a study by Reincke et al,12 one of 18 patients with pituitary incidentalomas and no apparent acromegalic features had a growth hormone-secreting pituitary adenoma. For this reason, looking for so-called silent growth hormone hypersecretion may be warranted in patients with pituitary tumors, especially in those with macroadenomas.9
The best initial test for growth hormone hypersecretion is the measurement of insulin-like growth factor-1 (IGF-1).13 A normal age- and sex-adjusted IGF-1 level almost always rules out acromegaly.
Further hormonal evaluation
Further hormonal evaluation should be guided by the clinical picture.
Cortisol. In a patient with excess weight gain, central obesity, proximal myopathy, and skin manifestations that suggest hypercortisolism, appropriate initial tests would be a midnight salivary cortisol level, an overnight 1-mg (low-dose) dexamethasone suppression test, or a 24-hour urinary free cortisol level.
Thyroid hormones. Patients with symptoms that suggest hyperthyroidism should have their thyroid-stimulating hormone (TSH; thyrotropin) and free thyroxine (T4) levels measured to rule out a TSH-secreting pituitary adenoma, a very rare tumor.
Gonadotropins. Screening for a gonadotropin-secreting pituitary adenoma by measuring follicle-stimulating hormone, luteinizing hormone, and gonadotropin alpha subunit is not routinely indicated, since almost all of such tumors are clinically silent and generally come to clinical attention only because of a mass effect (see below).