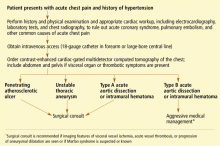
CT imaging for acute aortic syndrome
ABSTRACTAcute aortic syndrome can be due to acute aortic dissection, intramural hematoma, penetrating atherosclerotic ulcer, or unstable thoracic aneurysm. These life-threatening conditions are clinically indistinguishable, often presenting with acute chest pain. Contrast-enhanced, cardiac-gated multidetector computed tomography (CT) is a highly accurate imaging method for determining the cause of acute aortic syndrome.
KEY POINTS
- Acute aortic syndrome typically presents with chest pain in patients with a history of hypertension. In young patients with aortic dissection, one should consider Marfan syndrome and other connective tissue abnormalities.
- Cardiac gating is essential to avoid cardiac motion artifacts when evaluating the aortic root with contrast-enhanced multidetector CT.
- Urgent surgical repair is often necessary, especially for acute aortic dissection and intramural hematoma in the ascending aorta and aortic arch, unstable or ruptured thoracic aneurysm, and symptomatic penetrating atherosclerotic ulcers.
Acute aortic syndrome is often a life-threatening emergency, but because the presenting symptoms are nonspecific, it can be difficult to diagnose. Advances in computed tomography (CT)i have made the diagnosis of acute aortic syndromes easier and faster.
This article discusses the role of CT in patients with acute aortic syndrome. We review the imaging features and common indications for treating the various causes of acute aortic syndrome, and we discuss the possibly wider future role of CT for evaluating acute chest pain.
ACUTE AORTIC SYNDROME PRESENTS WITH CHEST PAIN
Acute aortic syndrome is defined as chest pain due to an aortic condition such as acute aortic dissection, intramural hematoma, penetrating atherosclerotic ulcer, or unstable thoracic aneurysm (see below).1
Of 464 patients included in the International Registry of Acute Aortic Dissection (IRAD),3 85% had acute symptoms. The pain was more often described as sharp than as the classic tearing pain. More than 70% of patients had hypertension.3 Half of patients younger than 40 years had Marfan syndrome4;a young patient with Marfan features who presents with acute chest pain should be strongly suspected of having aortic dissection. A bicuspid aortic valve or a history of aortic surgery should also raise the suspicion of acute aortic dissection.4
Acute chest pain is nonspecific
Furthermore, other possible manifestations of acute aortic syndrome are also nonspecific, eg, unexplained syncope, stroke, acute onset of congestive heart failure, pulse differentials (weaker pulses in one or more extremities), and malperfusion syndromes of the extremities or viscera.
Although aortic disease can sometimes cause acute coronary syndrome, keep in mind that acute coronary syndrome is more than 100 times more common than acute aortic dissection.3
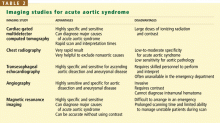
IMAGING STUDIES FOR ACUTE AORTIC SYNDROME
Transthoracic echocardiography is limited for evaluating acute aortic syndromes. However, transesophageal echocardiography is about 95% sensitive and specific for diagnosing acute aortic dissection, and intramural hematoma, and associated valvular regurgitation if the personnel who perform and interpret the test are highly experienced (although this level of expertise is not always available in the emergency department).5
CT has been improved
Several recent advances have contributed to CT’s very high sensitivity and specificity for diagnosing aortic disease.
Multiple detectors. Today’s CT machines have up to 64 rows of detectors, and this enables them to generate multiple simultaneous images with a slice thickness of less than 1 mm. Multidetector CT is also extremely fast: spiral imaging of the thorax can be done in a single breath-hold, which eliminates respiratory motion artifact.
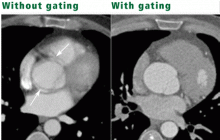
Cardiac synchronization of the image acquisition (cardiac gating) should be performed whenever the heart, coronary vessels, pulmonary veins, or aortic root needs to be evaluated; without cardiac gating, motion of the aortic root wall during the cardiac cycle causes artifacts in more than 90% of CT studies,5–7 precluding adequate evaluation of these structures (Figure 2). In cardiac gating, CT is synchronized with electrocardiography, “freezing” the action at specific phases of the cardiac cycle, typically during diastole when heart motion is limited. Two types of cardiac synchronization are available: retrospective gating and prospective triggering.
In retrospective gating (“spiral” or “helical” scanning), the x-ray source stays on throughout the cardiac cycle, but only the data from the desired part of the cardiac cycle are used to construct images. With this method, one can refine the images and remove motion abnormalities caused by irregular heartbeats. This acquisition technique is currently the most frequently used.
In prospective triggering (“step and shoot”), the x-ray source is turned on only during diastole or another prespecified part of the cardiac cycle. An advantage is that the patient is exposed to less radiation. A disadvantage is that, afterward, one has very little ability to correct any motion artifacts that occurred due to changes in heart rate or dysrhythmias.
Other improvements that have increased the sensitivity and specificity of CT for evaluating acute aortic syndrome are the ability to generate images in multiple planes (multiplanar reformation) on dedicated computer workstations.