Is Premarin actually a SERM?
It acts like a SERM…
Conjugated equine estrogen (Premarin) has historically been characterized as an estrogen agonist. But the report from the Women’s Health Initiative that long-term Premarin treatment is associated with a reduced risk of breast cancer raises the possibility that Premarin may have both estrogen agonist and antagonist properties. Premarin may actually be better categorized as a selective estrogen receptor modulator (SERM).
WHI: Premarin vs placebo
In the Premarin vs placebo arm, approximately 10,800 postmenopausal women with a prior hysterectomy who were 50 to 79 years of age were randomized to Premarin 0.625 mg daily or an identical-appearing placebo.1 After a mean follow-up of 7.1 years, the risk of invasive breast cancer in the women treated with Premarin was 0.80 (95% confidence interval [CI], 0.62–1.04, P=.09). When the data were analyzed based on adherence to the regimen, a statistically significant reduction in invasive breast cancer risk was observed in the women who reliably took their Premarin, compared with placebo (hazard ratio 0.67; 95% CI 0.47–0.97, P=.03).
Effects of tamoxifen and Premarin
Initially, tamoxifen was characterized as an “anti-estrogen,” but it is now recognized that tamoxifen has mixed properties. It is an estrogen antagonist in some tissues (breast) and an estrogen agonist in other tissues (bone). To recognize these mixed estrogen agonist–antagonist properties, tamoxifen is now categorized as a SERM. Premarin and tamoxifen share many similarities in their effects on major clinical outcomes in postmenopausal women (Table), including their effects on breast and endometrial cancer, deep venous thrombosis, and osteoporotic fracture. One clinically important divergence is that tamoxifen increases and Premarin decreases vasomotor symptoms.
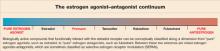
Commonly used medications that interact with the estrogen receptor can be arranged along a continuum from a “pure” estrogen agonist, such as estradiol, to a “pure” estrogen antagonist (antiestrogen), such as fulvestrant (Figure). Along this dimension, Premarin likely shares more properties with estrogen than other SERMs. In contrast, raloxifene probably shares more properties with a pure antiestrogen such as fulvestrant because, unlike tamoxifen and Premarin, raloxifene does not increase the risk of endometrial cancer.
TABLE
Effects of tamoxifen and Premarin on clinical endpoints in postmenopausal women
| CLINICAL ENDPOINT | TAMOXIFEN | PREMARIN | ARE THE EFFECTS OF TAMOXIFEN AND PREMARIN IN THE SAME DIRECTION? |
|---|---|---|---|
| Breast cancer | Decreased risk | Decreased risk | Yes |
| Endometrial cancer | Increased risk | Increased risk | Yes |
| Osteoporotic fracture | Decreased risk | Decreased risk | Yes |
| Deep venous thrombosis | Increased risk | Increased risk | Yes |
| Vasomotor symptoms | Increase | Decrease | No |
The complex biology of the estrogen receptor system and the complex pharmacology of Premarin may explain its SERM activity.2 The functional biology of the estrogen receptor system has not been fully elucidated. The selective tissue effects of various estrogenic compounds are thought to be mediated by at least 3 factors:
In addition, Premarin is a complex hormone containing many compounds, including estrone sulfate, equilin sulfate, delta 8,9-dehydroestrone sulfate, 17-alpha estradiol sulfate and 17-alpha dihyroequilin sulfate. Each may have different estrogen agonist–antagonist properties in various tissues. For example, some studies report that delta 8,9-dehydroestrone sulfate, one component of Premarin, is a potent estrogen agonist in the brain, but is a weak estrogen agonist in the liver.6 In contrast, estrone sulfate, a major component of Premarin, is an estrogen agonist in both the brain and liver. The 17-alpha estradiol and 17-alpha dihydroequilin compounds contained in Premarin are also of interest, because although they can bind to the human estrogen receptor, the 17-alpha configuration markedly reduces their biological activity. The 17-alpha estrogens in Premarin may be SERMs because they have good affinity for the estradiol receptor but low gene promoter activity in multiple model systems.
Is Premarin a SERM?
Most likely the answer is “yes,” but we need to know much more about the functional biology of the estrogen receptor system and the relative estrogen agonist–antagonist effects of Premarin and its components. Categorizing Premarin as a “SERM” rather than an “estrogen” necessitates that clinicians change their concepts about how this commonly used hormone treatment actually works. Until we know more about this complex issue, most clinicians will individualize hormone treatment and follow the guideline: “Use the lowest effective dose of hormone therapy for the shortest period of time.”
* Premarin was the medication used in the trial. It is unclear whether the results would be similar with other formulations of conjugated estrogens or conjugated equine estrogens.