Chronic genital skin disorders: 6 challenging conditions
When chronic skin disorders persist or recur, immune dysfunction may be a reason. Here’s how to respond.
HPV infection
The small HPV particle easily gains entry to minimally traumatized vulvar skin—with a high transmission rate with even a single exposure—and the immature epithelium of the cervical transformation zone makes that site a naturally compromised barrier to infection.
Under normal conditions, a cell-mediated immune response eliminates the HPV virus within 12 months, with lasting protection from reinfection. If cell-mediated immunity is compromised, the virus cannot be eliminated. The result is genital warts, variable degrees of dysplasia, or cancer, depending on the degree of immune compromise (FIGURE 5).
Risk factors for HPV-associated warts and dysplasia include allergy, immunosuppressant drugs to prevent rejection of a transplanted organ, and smoking. Smoking cessation is particularly important because control of the virus is dependent on Langerhans-cell function.
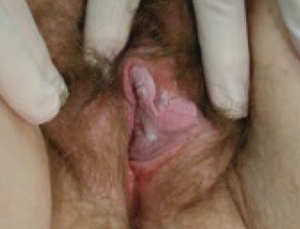
FIGURE 5 Genital warts
Debulking of warts with cryocautery or electrocautery may be appropriate, followed by imiquimod cream. It is prudent to biopsy persistent warts to exclude carcinoma, especially in an immunocompromised patient.
Begin by debulking warts
Electro- or cryocautery of large warts is an appropriate first step. Follow debulking with thrice-weekly application of one packet of imiquimod cream, to be washed off in the morning, for 4 to 6 weeks. This therapy may not eliminate genital warts in women who are taking immunosuppressant drugs to prevent organ-transplant rejection. Unfortunately, control of genital warts with monthly cautery of new warts may be the only useful option in these patients. Immunocompromised patients are at high risk for squamous carcinoma, and biopsy of persistent warts may be wise.
Vulnerabilities of vulvovaginal skin
The skin of the vulva and vagina is far from invincible. Some factors that affect it adversely are aging,4 tobacco use,5 estrogen deficiency,6 immunosuppressant drugs, and human immunodeficiency virus (HIV) infection.7 Look for these risk factors in women with persistent genital infection, so that the management plan can include treatment of the underlying dermatologic or immune disorder, as well as any microbes that are identified.
Immunosuppressed patients
Rejection of a transplanted organ is a function of cell-mediated immunity, so it is not surprising that drugs that suppress transplant rejection also inhibit vulvovaginal cell-mediated immunity. This increases the risk that HPV-associated disease will progress. Imiquimod cream promotes cell-mediated immunity by activating the release of interferon in the vulvar skin, and may compensate for depressed immune-cell function in the nontransplant population, but it is less effective in the transplant recipient. Sadly, there is no long-term solution to the effects of immunosuppressant therapy in this population; special surveillance for vulvar cancer and cervical dysplasia is necessary. Smoking cessation is also essential, especially for women with HPV-associated disease.
When HIV infection progresses to AIDS, Langerhans cells that carry HIV are depleted from the skin and substantially decrease in number, completely compromising cell-mediated immunity. This explains why AIDS patients often have severe genital herpes infections, severe chronic yeast vulvovaginitis, extensive molluscum disease, and unusual skin cancers. Antiretroviral therapy may restore some Langerhans-cell function.
Consider screening for HIV/AIDS when a woman has severe recurrent genital viral or yeast infection.
Aging and estrogen deficiency
Cell-mediated immune function declines with age. A higher risk of skin cancer, herpes (and its recurrence), and irritant and allergic vulvar dermatitis are the results. Increased surveillance for skin cancer, and varicella vaccination to lower the risk for herpes zoster, may be important.
Topical estrogen may be indicated if saline wet-prep evaluation reveals parabasal cells in vaginal secretions of a symptomatic postmenopausal woman. The estrogen may gradually alleviate burning and restrict potentially pathogenic bacterial flora. Be aware, however, that commercially available estrogen creams often contain propylene glycol, a recognized irritant of fragile skin. One solution: Have a compounding pharmacist formulate an equivalent cream (estradiol, 0.1 mg/g) for twice-daily topical application, using a base of petrolatum or solid vegetable oil.






