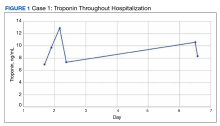
A Case Series of Rare Immune-Mediated Adverse Reactions at the New Mexico Veterans Affairs Medical Center
Background: Immune checkpoint inhibitor (ICI) therapy has revolutionized the treatment of several solid tumors. The use of ICIs is expected to rise as a growing number of indications are approved for their use by the US Food and Drug Administration and with the increasing number of patients with cancer. Unfortunately, ICIs are associated with the development of immune-mediated adverse reactions (IMARs). About 5% to 10% of patients developing severe toxicities requiring treatment postponement or discontinuation. IMARs can affect any organ, but most frequently the skin and endocrine glands are involved.
Case Presentation: We present a case series of IMARs observed at the New Mexico Veterans Affairs Medical Center. First, we present a case of grade 4 myocarditis in an 84-year-old man receiving chemoimmunotherapy for lung adenocarcinoma to demonstrate the rapid progression of this rare condition. Second, we present a case of uveitis in a 70-year-old man with superficial bladder cancer undergoing treatment with pembrolizumab. Finally, we present a case of a 63-year-old man with pleuritis and organizing pneumonia secondary to dual ICI treatment (nivolumab and ipilimumab) for mesothelioma. A discussion regarding the epidemiology of these IMARs, expected course, and optimal management follows each rare toxicity described.
Conclusions: Though these toxicities are uncommon, they serve as a reminder to clinicians across specialties that IMARs can drive the acute deterioration of any organ, and consideration of toxicities secondary to ICIs should be considered for any atypical presentation of unclear etiology.
Case 1: Myocarditis
An 84-year-old man receiving a chemoimmunotherapy regimen consisting of carboplatin, pemetrexed, and pembrolizumab for recurrent, stage IV lung adenocarcinoma developed grade 4 cardiomyopathy, as defined by the Common Terminology Criteria for Adverse Events (CTCAE) v5.0, during his treatment.8 He was treated for 2 cycles before he began experiencing an increase in liver enzymes.
The patient’s presentation was concerning for myocarditis, and he was quickly admitted to NMVAMC. Cardiac catheterization did not reveal any signs of coronary occlusive disease. Prednisone 1 mg/kg was administered immediately; however, given continued chest pain and volume overload, he was quickly transitioned to solumedrol 1000 mg IV daily. After the initiation of his treatment, the patient’s transaminitis began to resolve, and troponin levels began to decrease; however, his symptoms continued to worsen, and his troponin rose again. By the fourth day of hospitalization, the patient was treated with infliximab, a tumor necrosis factor-α inhibitor shown to reverse ICI-induced autoimmune inflammation, with only mild improvement of his symptoms. The patient’s condition continued to deteriorate, his troponin levels remained elevated, and his family decided to withhold additional treatment. The patient died shortly thereafter.
Discussion
Cardiotoxicity resulting from ICI therapy is far less common than the other potential severe toxicities associated with ICIs. Nevertheless, many cases of ICI-induced cardiac inflammation have been reported, and it has been widely established that patients treated with ICIs are generally at higher risk for acute coronary syndrome.9-11 Acute cardiotoxicity secondary to autoimmune destruction of cardiac tissue includes myocarditis, pericarditis, and vasculitis, which may manifest with symptoms of heart failure and/or arrhythmia. Grading of ICI-induced cardiomyopathy has been defined by both CTCAE and the American Society of Clinical Oncology (ASCO), with grade 4 representing moderate to severe clinical decompensation requiring IV medications in the setting of life-threatening conditions.
Review articles have described the treatment options for severe cases.7,12 As detailed in prior reports, once ICI-induced cardiomyopathy is suspected, urgent admission and immediate evaluation to rule out acute coronary syndrome should be undertaken. Given the potential for deterioration despite the occasional insidious onset, aggressive cardiac monitoring, and close follow-up to measure response to interventions should be undertaken.