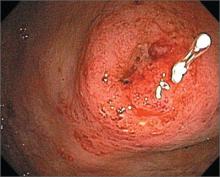
Episodic rectal bleeding
A 30-year-old man sought care from his family physician (FP) for intermittent episodes of bloody diarrhea. This was the third such episode; the last one occurred several weeks earlier. He indicated that cramps accompanied the bouts of diarrhea, but felt fine when the diarrhea wasn’t an issue. The patient hadn’t traveled outside of the United States. He was of Ashkenazi Jewish descent and had a cousin with Crohn’s disease. Colonoscopy showed mucosal friability with superficial ulceration and exudates confined to the rectosigmoid colon.
What's your diagnosis?
The FP made a clinical diagnosis of ulcerative colitis that was confirmed by colonoscopic biopsy.
Inflammatory bowel disease (IBD) includes ulcerative colitis (UC) and Crohn’s disease. The intestinal inflammation in UC is usually confined to the mucosa and affects the rectum with or without parts or the entire colon (pancolitis) in an uninterrupted pattern. In Crohn’s disease, inflammation is often transmural and affects primarily the ileum and colon, often discontinuously. However, Crohn’s disease can affect the entire GI tract from mouth to anus.
There is a predilection for IBD in those of Jewish ancestry (especially Ashkenazi Jews) followed in order by non-Jewish whites and African Americans, Hispanics, and Asians.
UC is classified by severity based on the clinical picture and results of endoscopy; treatment is based on disease classification.
○ Mild: Less than 4 stools per day, with or without blood, no signs of systemic toxicity, and a normal erythrocyte sedimentation rate (ESR).
○ Moderate: More than 4 stools per day but with minimal signs of toxicity.
○ Severe: More than 6 bloody stools per day, and evidence of toxicity is demonstrated by fever, tachycardia, anemia, and elevated ESR.
○ Fulminant: Patient may have more than 10 bowel movements daily, continuous bleeding, toxicity, abdominal tenderness and distention, a blood transfusion requirement, and colonic dilation on abdominal plain films.
Treatment for mild to moderate distal disease includes: oral aminosalicylates (ASAs), topical mesalamine, or topical steroids. An oral 5-ASA agent can be a prodrug (eg, sulfasalazine, 2 - 6 g/day), a drug with a pH-dependent coating (eg, Asacol, 2.4 - 4.8 g/day), or a slow-release agent (Pentasa, 2 - 4 g/day). Mesalamine suppositories (1 g/day) are the best way to induce remission in patients with proctitis. Rectal suppositories or enemas should also be used to improve medication delivery when treating active distal colitis, and a combination of oral and rectal mesalamine is better than monotherapy to stop rectal bleeding.
Up to 75% of patients will show clinical improvement with 2 g/day of 5-ASA and a similar percentage will maintain remission with doses of 1.5 to 4 g/day.
In this case, the patient’s physician started him on sulfasalazine and referred him to a gastroenterologist.
Photo courtesy of Marvin Derezin, MD. Text for Photo Rounds Friday courtesy of Richard P. Usatine, MD. This case was adapted from: Smith M. Inflammatory bowel disease. In: Usatine R, Smith M, Mayeaux EJ, et al, eds. Color Atlas of Family Medicine. 2nd ed. New York, NY: McGraw-Hill; 2013:405-413.
To learn more about the Color Atlas of Family Medicine, see: https://www.amazon.com/Color-Family-Medicine-Richard-Usatine/dp/0071769641/
You can now get the second edition of the Color Atlas of Family Medicine as an app by clicking this link: https://usatinemedia.com/