Whom should you test for secondary causes of hypertension?
IT'S RECOMMENDED that all children and adolescents with a new diagnosis of hypertension undergo renal ultrasound and laboratory evaluation for renal pathology (strength of recommendation [SOR]: C, consensus-based guidelines).
Specific diagnostic tests are recommended for newly diagnosed patients who have suspicious clinical findings suggestive of a secondary cause of hypertension based on the initial history (excess daytime sleepiness, palpitations, tremor, sweating); physical examination (abdominal bruit, thyromegaly, malar rash); or laboratory analysis (elevated serum creatinine, low thyroid-stimulating hormone) (SOR: C, consensus-based guidelines).
Patients with undifferentiated resistant hypertension should receive further directed evaluation for secondary causes (SOR: C, consensus-based guidelines).
EVIDENCE SUMMARY
The evidence for selecting which patients should undergo additional testing for potentially correctable secondary causes of hypertension is based on the prevalence of these causes in different age groups, case series of reversal of hypertension with effective treatment of the underlying cause, and clinical suspicion of a secondary cause that may be reversible. We found no prospective cohort studies or randomized trials evaluating diagnostic approaches or outcomes associated with particular selection criteria for conducting additional diagnostic evaluations in search of secondary causes. Therefore, our recommendations are based primarily on expert guidelines, which we summarize here.
When caring for children and adolescents with newly diagnosed hypertension...
Secondary hypertension is more prevalent in younger children and in children and adolescents with stage 2 hypertension (blood pressure [BP] >99th percentile for age and height plus 5 mm Hg).1 Renoparenchymal and renovascular disease account for most cases of secondary hypertension in these children.2
The National High Blood Pressure Education Program Working Group on High Blood Pressure in Children and Adolescents recommends that all children and adolescents with hypertension have an additional diagnostic work-up. This is based on the observation that 70% to 85% of children <12 years and 10% to 15% of adolescents 12 to 18 years with hypertension have an underlying cause, most commonly renoparenchymal and renovascular disease.3
According to the National Institutes of Health (NIH), “the possibility that some underlying disorder may be the cause of the hypertension should be considered in every child or adolescent” with elevated BP, but the evaluation itself should be individualized.3
The NIH recommends more extensive evaluation for very young children, children with stage 2 hypertension, and children or adolescents who show clinical signs suggesting hypertension-linked systemic conditions. Such evaluation should include a renal ultrasound and laboratory testing (creatinine, urinalysis, and urine culture) to look for structural or functional anomalies.3
What about newly diagnosed adults with suspected secondary causes?
Secondary hypertension reportedly occurs in 5% to 10% of hypertensive patients.4,5 The only prospective study completed in a primary care setting evaluated 1020 patients at a general outpatient clinic in Yokohama, Japan. The investigators reported that 9.1% of the patients had an endocrinologic or renovascular cause contributing to their hypertension.6 The 5 most common causes were primary aldosteronism (6%), Cushing syndrome (1%), preclinical Cushing syndrome (1%), pheochromocytoma (0.6%), and renovascular disease (0.5 %).6
According to the Institute for Clinical Systems Improvement (ICSI), patients at highest risk for secondary hypertension have no family history of hypertension; abrupt onset, symptomatic, or crisis hypertension; stage 2 hypertension; sudden loss of hypertensive control; and drug-resistant hypertension.7
The Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure recommends that patients with the following characteristics undergo further directed evaluation for a secondary cause:8
• younger than 30 years with no family history of hypertension
• older than 55 years with new hypertension
• abdominal bruit with diastolic component
• sudden worsening of BP control
• recurrent flash pulmonary edema
• renal failure with abnormal urinary sediment or proteinuria
• acute renal failure after administration of an ACE inhibitor or ARB.
These patients should receive particular scrutiny
Patients with resistant hypertension (BP>140/90 mm Hg despite taking optimal doses of 3 antihypertensive medications, one of which is a diuretic) should receive particular scrutiny for an identifiable secondary cause, according to the ICSI.7
In a retrospective analysis of 141 patients with resistant hypertension referred to a university hypertension center in Chicago in 2005, 5% of patients had an identifiable secondary cause.9 A chart review of 436 patients presenting to a tertiary hypertension clinic in Japan identified 91 with resistant hypertension. A secondary cause was identified in 9.1%.10
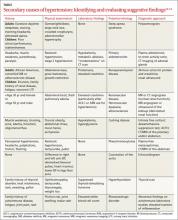
Careful history and examination should identify patients suffering from uncontrolled hypertension because of noncompliance, suboptimal antihypertensive regimen, inaccurate BP readings, antagonizing substances, and white coat hypertension.11 The TABLE summarizes common presentations of, and workup for, secondary causes of hypertension.12-14