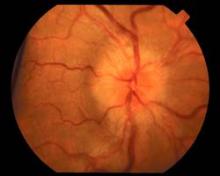
Chronic headaches
A 29-year-old obese woman sought care for chronic headaches that were worse in the morning or while lying down. She denied nausea or other neurologic symptoms. She had no other medical problems and took no medications. On examination, she had a visual acuity of 20/20 in both eyes, no spontaneous venous pulsations, and no other neurologic signs.
What's your diagnosis?
The family physician (FP) recognized the papilledema on funduscopic exam and ordered a lumbar puncture, which led to a diagnosis of idiopathic intracranial hypertension. (A brain MRI was also ordered, but it showed no mass or hydrocephalus.)
The term papilledema refers specifically to optic disc swelling related to increased intracranial pressure. When no localizing neurologic signs or space-occupying lesion is present, idiopathic intracranial hypertension (IIH) is likely the cause in patients younger than age 45 years—especially obese women. Patients with IIH usually present with daily pulsatile headaches with nausea, and often have transient visual disturbances and/or pulsatile tinnitus. Patients often report hearing a “whooshing” sound. Bilateral papilledema and visual field defects on a perimetry test are found in almost all patients. Elevated opening pressure on lumbar puncture is required for the diagnosis.
In many cases, IIH is self-limiting, presents without visual symptoms, and will resolve over several years without loss of vision. However, when patients present with persistent or worsening visual disturbances, treatment is required to lower the intracranial pressure to prevent optic nerve damage and irreversible loss of vision. Management of the headache is a key factor when choosing a therapeutic plan. Management includes the following:
Nonpharmacologic options
- careful observation—often by an ophthalmologist—with documentation of any visual changes (formal visual field testing is indicated).
- weight loss of 15% of body weight is beneficial, but will not decrease intracranial pressure quickly enough if visual compromise is present.
Medications
- acetazolamide 1000 to 2000 mg/day; early studies indicate that topiramate may also be effective; other diuretics such as furosemide are less effective.
- high-dose corticosteroids for short periods for rare cases of rapidly advancing vision loss.
In this case, the patient was started on acetazolamide and joined a weight-loss program. Her symptoms resolved over the course of 18 months.
Text for Photo Rounds Friday courtesy of Richard P. Usatine, MD. Photo courtesy of Paul D. Comeau. This case was adapted from: Chumley H. Papilledema. In: Usatine R, Smith M, Mayeaux EJ, et al, eds. Color Atlas of Family Medicine. 2nd ed. New York, NY: McGraw-Hill; 2013:151-154.
To learn more about the Color Atlas of Family Medicine, see:
• https://www.amazon.com/Color-Family-Medicine-Richard-Usatine/dp/0071769641/ref=dp_ob_title_bk
You can get the second edition of the Color Atlas of Family Medicine as an app for mobile devices by clicking this link: