Discolored lower legs
A 30-year-old woman asked her family physician (FP) to look at the discoloration on both of her lower legs. She did not have diabetes, but she indicated that type 2 diabetes did run in her family. She had visible hyperpigmentation, yellow discoloration, atrophy, and telangiectasias on her legs. The patient’s blood sugar during the visit was 142 mg/dL 1 hour after eating lunch.
What's your diagnosis?
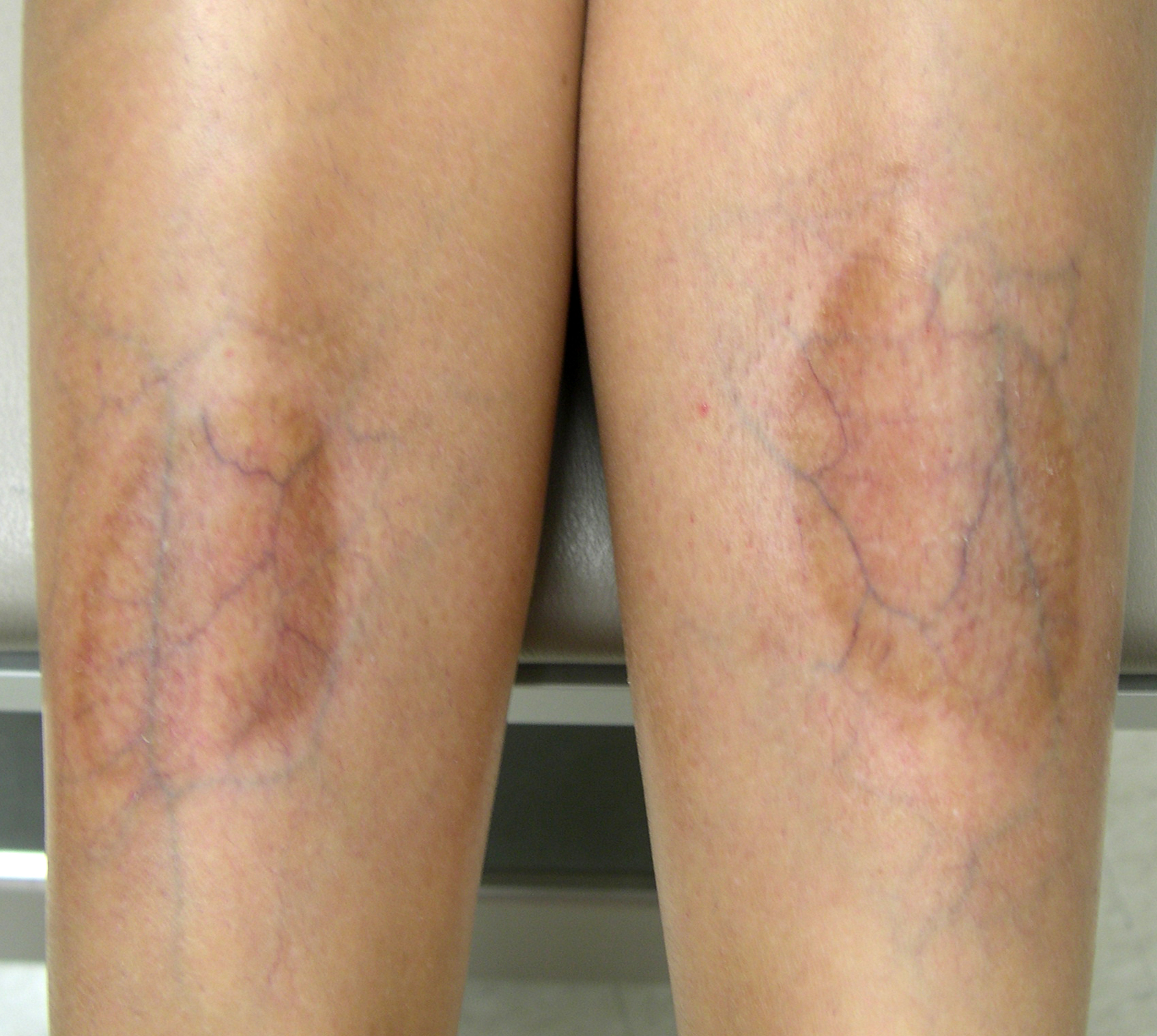
The FP recognized the lesions as necrobiosis lipoidica (NL) and ordered some lab work. The following day, the patient’s fasting blood sugar was 121 mg/dL, with a glycosylated hemoglobin value of 6.1%.
NL was previously called necrobiosis lipoidica diabeticorum because it was thought to be seen almost exclusively in patients with diabetes. A significant minority of patients with NL do not have diabetes, however, so the newer name is NL. The condition is rare, and occurs in 0.3% of patients with diabetes. NL primarily affects women—particularly those with type 1 diabetes—but it can occur with type 2. Average age of onset is 34 years.
The cause of NL remains unknown. The lesions are usually located on the shins. They begin as erythematous papules or plaques in the pretibial area and become larger and darker, with irregular margins and raised erythematous borders. The lesion’s center atrophies and turns yellow in color. There is often a prominent brown color or hyperpigmentation. The lesions may ulcerate and become painful. Telangiectasias and prominent blood vessels may be seen within the lesions. The yellow color may result from lipid deposits or beta-carotene—hence the term “lipoidica.”
Treatment options include topical steroids or intralesional injections (2.5 mg/mL triamcinolone). Treatment risks include increasing the existing atrophy, so patients should be informed of risks and benefits before initiating steroid treatments. Another treatment option (off-label) is pentoxifylline (400 mg, 2-3 times daily). Pentoxifylline improves blood flow and decreases red cell and platelet aggregation; however, it’s use is only supported by case reports.
In this case, the FP recommended diet and exercise for the patient’s borderline diabetes and prescribed a moderate-strength topical corticosteroid.
Photo courtesy of Suraj Reddy, MD. Text for Photo Rounds Friday courtesy of Richard P. Usatine, MD. This case was adapted from: Smith M. Necrobiosis lipoidica. In: Usatine R, Smith M, Mayeaux EJ, et al, eds. The Color Atlas of Family Medicine. New York, NY: McGraw-Hill; 2009:948-950.
To learn more about The Color Atlas of Family Medicine, see:
• https://www.amazon.com/Color-Atlas-Family-Medicine/dp/0071474641
You can now get The Color Atlas of Family Medicine as an app for mobile devices including the iPhone, iPad, and all Android devices by clicking this link




