Annular rash
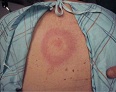
On a summer afternoon, a 32-year-old woman went to see her family physician (FP) because she’d had a low-grade fever for 5 days. She also had a rash. Her FP noted a large, erythematous, annular patch with central clearing on her back. The patient indicated that the rash had gotten progressively larger during the previous 3 days and that her joints had been bothering her. She didn’t recall being bitten by an insect, but had been on a recent camping trip in eastern Massachusetts.
What's your diagnosis?
| 
|
| FIGURE 1 | FIGURE 2 |
The FP recognized the annular pattern of erythema migrans (EM) (FIGURE 1) and diagnosed the patient with Lyme disease.
In 1977, clusters of patients in Old Lyme, Connecticut, began reporting symptoms originally thought to be juvenile rheumatoid arthritis. In 1981, American entomologist, Dr. Willy Burgdorfer, isolated the infectious pathogen responsible for Lyme disease from the midgut of Ixodes scapularis (aka, black-legged deer ticks) (FIGURE 2), which serve as the primary transmission vector in the United States.
Localized Lyme disease has a duration of days to weeks. The pathognomonic finding of erythema migrans occurs in roughly 68% of Lyme disease cases. Described as a “bull’s eye” eruption, this nonpruritic, maculopapular lesion typically occurs near the site of infection. The erythematous perimeter migrates outward over several days while the central area clears. Multiple lesions in different sites can develop in some individuals. Erythema migrans can persist for 2 to 3 weeks if left untreated. Roughly 67% of patients will develop flu-like symptoms that can include fever, myalgias, and lymphadenopathy. Symptoms usually subside within 7 to 10 days.
Diagnosing Lyme disease is generally based on pertinent history findings and/or the presence of an EM lesion, especially in patients living in endemic areas. In cases where an EM lesion is absent, serological testing (enzyme-linked immunosorbent assay, Western blot [IgM and IgG for Borrelia burgdorferi]) may be warranted.
Empiric antibiotic therapy should be considered when there is an EM rash and flu-like symptoms after a known tick bite, a case of Bell’s palsy in an endemic area (especially between June and September), or a tick bite that occurs during pregnancy.
In this case, the patient met the criteria for empiric therapy and responded quickly to antibiotics (doxycycline 100 mg twice daily for 14 days).
Photos courtesy of Thomas Corson, MD and McGraw-Hill. The text for Photo Rounds Friday is courtesy of Richard P. Usatine, MD. This case was adapted from: Corson T, Usatine, R. Lyme disease. In: Usatine R, Smith M, Mayeaux EJ, et al, eds. The Color Atlas of Family Medicine. New York, NY: McGraw-Hill; 2009:933-939.
To learn more about The Color Atlas of Family Medicine, see:
• https://www.amazon.com/Color-Atlas-Family-Medicine/dp/0071474641
You can now get The Color Atlas of Family Medicine as an app for mobile devices including the iPhone and iPad by clicking this link:




