How to remove those things children put up their nose
Beans, buttons, batteries… Kids put all sorts of objects in their nostrils. Here’s how best to retrieve them.
When a parent brings in a young child who has inexplicably used his or her nostril as the repository for an object like a marble or a button, are you prepared to get it out—or do you send them to the ED? If you send patients to the local hospital (or otolaryngologist), you’re not alone. Lack of appropriate equipment prevents many family physicians from handling this all-too-common dilemma. Yet you can usually retrieve a nasal foreign body yourself, if you have several simple instruments (FIGURE 1) and a topical decongestant and anesthetic on hand.
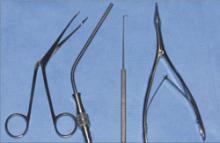
FIGURE 1
Pediatric nasal retrieval tools you’ll need
The equipment you’ll need to remove an object from a child’s nostril includes (left to right): Hartmann forceps, Frazier suction tube, blunt-tipped right-angle ear hook, and pediatric nasal speculum.
What did he put up there? Parental history often yields the specific time of insertion and the item involved. When such information is not available, purulent unilateral nasal discharge strongly suggests the presence of a foreign body. A plain radiograph can help identify a metallic or radiopaque object such as a button-like hearing aid battery. Batteries leak caustic alkali and require rapid removal. (Of course, all objects should be extracted as promptly as possible.)
Start with a topical decongestant
How to proceed? Apply a topical decongestant with 0.05% oxymetazoline, either in the form of a spray or nasal drops, to reduce edema and bleeding and facilitate removal. (I recommend applying the nasal decongestant to both nostrils; the child may have inserted more than 1 foreign object, so you should always examine both sides.)
The decongestant may be supplemented with a 4% lidocaine topical anesthetic, to reduce the discomfort associated with object retrieval—and, possibly, make the procedure less stressful for patient, family, and physician. If you’re using an oxymetazoline spray bottle, remove the top, add an equal amount of the lidocaine, and replace the top before applying it. You can use the same 50-50 formula to mix lidocaine and nasal drops.
Use a “papoose.” For further ease and safety, restrain the patient by wrapping him or her in a bed sheet made into a “papoose.” While there is a trend away from restraining children, my experience suggests that doing so reduces the risk of intranasal injury caused by uncontrolled patient motion while instruments are in the nose. Good lighting is also essential (a headlight is best), along with suction and safety eyewear for the staff.
Have the right equipment on hand
The pediatric nasal speculum, with its shorter blades, is best for small nostrils (FIGURE 1). The blunt-tipped right-angle ear hook is probably the most useful instrument for retrieving nasal foreign bodies because it can reach behind objects such as beads, buttons, or batteries, and hook textile or other fabric-like foreign bodies. The Hartmann forceps are more effective than the smaller jaw “alligator” forceps (FIGURE 2); their longer jaws with their less obtuse angle make it easier to avoid pushing the object posteriorly. Availability of these few instruments will allow you to remove most foreign bodies, reducing the need to refer to another physician.
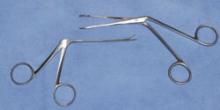
FIGURE 2
Which forceps are best?
Avoid using the alligator forceps (left) for retrieving a nasal foreign body; the longer jaws of the Hartmann forceps (right) are less likely to push the object farther into the nostril.
No luck? If your efforts fail, referral will of course be necessary. It’s usually better to send the patient to an otolaryngologist than to the ED, for 2 reasons: (1) The otolaryngologist is more likely to have rigid nasal endoscopes on hand, and (2) a visit to the otolaryngologist will typically cost less than a trip to the ED. In addition, an otolaryngic evaluation will help determine whether a particular case warrants an extraction in the operating room under general anesthesia.