Brown recluse spider bite? Consider this uniquely conservative treatment
An antihistamine and observation work as well—and often better—than more intensive therapies.
- Be concerned about brown recluse envenomation when a patient reports intensifying localized pain disproportionate to physical findings after a “bite” (C).
- Prescribe an oral antihistamine alone to control symptoms, even with a necrotic wound, and mark the patient’s progress over 24 hours (C).
- If the patient improves dramatically, continue the antihistamine; with little or no improvement, consider giving an antibiotic with the antihistamine (C).
Strength of recommendation (SOR)
- Good-quality patient-oriented evidence
- Inconsistent or limited-quality patient-oriented evidence
- Consensus, usual practice, opinion, disease-oriented evidence, case series
What is the best way to treat the bite of a brown recluse spider? Having treated more than 185 bite wounds on 150 patients over the past 30 years, I have found that an oral antihistamine works best and makes surgery unnecessary.
I did not arrive at this treatment protocol immediately but, rather, developed it in 4 phases, which I describe in this article. Not only does this conservative approach consistently heal confirmed brown recluse bite wounds, but should a bite be mistakenly attributed to the brown recluse (or one of its relatives in the Loxosceles genus of spider), there is no harm to the patient, nor any big expense.
Is a brown recluse to blame?
Due to limited experience among the wider medical community in identifying spider envenomation,1-4 bite recognition and selection of appropriate therapy can be difficult.
Early findings can be confusing. Brown recluse bites typically feel like a pin prick. A vasoconstrictive halo may surround the bite, but this sign is inconsistent. Usually there is nothing to see immediately and pain from the bite goes away, so most patients dismiss the incident.5 Soon, however, pain from the envenomation begins and, importantly, becomes disproportionate to physical findings—the patient shows you where it hurts, but there is nothing visible to support a diagnosis or suggest a course of action.
Progression of the wound usually tells more than a captured specimen. If you are fortunate enough to examine an intact spider caught by the patient, a “fiddle” mark on the spider’s back confirms it is a brown recluse (FIGURE 1). However, most specimens brought in for examination are so misshapen from the patient’s retribution as to make identification futile. I focus instead on the resultant wound.
Spider’s venom causes the wound. Spiders lack a mechanical digestive system; their so-called venom actually is a set of enzymes that liquefy a prey’s tissues.6 In the 48 hours after a bite, these digestive enzymes cause a progressive necrosis of fat under the skin. Eventually the overlying skin also turns necrotic. The venom does not penetrate underlying fascia planes, as many infectious processes do.
Necrosis can, rarely, cause disseminated intravascular coagulation and death. A more likely scenario, though still relatively uncommon, is that the necrotic sequence leads to an indolent wound that heals only with difficulty. Most patients recover without medical care and do not even seek it.7-9
Wounds can be categorized, as outlined by Auer et al,10 into groups 1 through 4, from least severe to most severe. However, this classification scheme has made no difference in my management decisions.
FIGURE 1
The distinctive “fiddle” mark
How my treatment protocol evolved
My protocol for treating necrotic bite wounds of the brown recluse, and similar wounds from other insects, progressed over 30 years through 4 phases of treatment concepts.
Phase 1: Surgical excision
From 1979 to 1980, I treated necrotic wounds with surgical excision and secondary closure or skin grafting.1 Many patients complained of severe itching around these wounds, which I treated empirically with the antihistamine Benadryl. All patients experienced symptom relief and had a reasonable cosmetic result (FIGURE 2).
In writing up the case results for a presentation to the Society of Air Force Clinical Surgeons, I conducted background research and found a postulate suggesting that antigen recognition was an important factor in wound progression and that it took approximately 7 days to achieve. That postulate drove the second phase of discovery.1
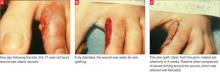
FIGURE 2
Bite wound treatment: Debridement and closure or skin grafting
From 1980 to 1981, I focused on the postulate, which also suggested that the antigen–antibody reaction following envenomation could make reactions to subsequent (“second set”) bites less severe.1 This made sense, though good clinical data were lacking.