Itchy rash in groin
A 45-year-old man sought care from his family physician (FP) for a rash in his groin that he’d had for over a year. The rash was itchy and would not go away, no matter what he tried. The patient’s previous doctor had prescribed both topical and oral antifungal medicines, which hadn’t helped. The patient also bought 1% hydrocortisone cream, which diminished the itching, but didn’t resolve the rash. The patient had a history of controlled hypertension and smoked a pack of cigarettes a day.
What’s your diagnosis?
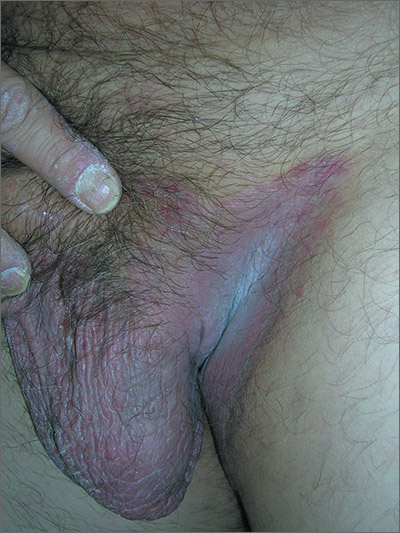
The FP examined the rash closely and considered a diagnosis of inverse psoriasis. He looked at the patient’s nails for further clues and found that the patient had nail pitting and some onycholysis, which are both found in psoriasis. There were also some psoriatic plaques over the dorsum of his fingers. The remainder of the patient’s skin was clear.
Between the nail findings and the fact that the rash didn’t respond to antifungal medicine, the FP realized that this was truly inverse psoriasis and decided not to perform a potassium hydroxide (KOH) preparation.
The partial response to hydrocortisone supported the psoriasis diagnosis as well, but the FP knew that hydrocortisone was rarely potent enough to treat psoriasis, so he prescribed topical triamcinolone cream. While ointments are frequently more potent, the choice of the cream was made to avoid the greasiness that the patient would feel with an ointment in the groin.
Triamcinolone was chosen to avoid issues of atrophy that could occur with a higher potency steroid in an intertriginous area. However, if the triamcinolone was not effective, the FP was prepared to prescribe a stronger potency topical steroid for a short period of time until the psoriasis cleared. Then, the moderate potency triamcinolone could be used to prevent recurrence. The patient was also told he could use the triamcinolone on his fingers.
The physician counseled the patient on quitting smoking because smoking worsens psoriasis and, of course, has many health risks. The patient was not willing to completely stop, but said he would try to cut down. The FP encouraged him to have a long-term goal of complete smoking cessation.
At a follow-up visit one month later, the rash was 90% better, but the psoriasis over the fingers was only 50% better. The FP then prescribed clobetasol ointment for the fingers and told the patient to also use it in the inguinal area for one week. Two months later, the patient had 95% clearance in both areas. The FP told the patient that this is a lifelong disease that can often be controlled, but not cured.
Photos and text for Photo Rounds Friday courtesy of Richard P. Usatine, MD. This case was adapted from: Usatine R, Smith M. Tinea cruris. In: Usatine R, Smith M, Mayeaux EJ, et al, eds. Color Atlas of Family Medicine. 2nd ed. New York, NY: McGraw-Hill; 2013:795-798.
To learn more about the Color Atlas of Family Medicine, see: www.amazon.com/Color-Family-Medicine-Richard-Usatine/dp/0071769641/
You can now get the second edition of the Color Atlas of Family Medicine as an app by clicking on this link: usatinemedia.com




