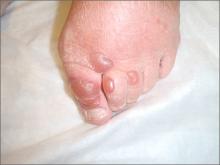
Blisters on toes
A 69-year-old woman with a history of hypertension, hyperlipidemia, diabetes, osteoarthritis, and depression presented to the emergency department (ED) with a 2-day history of clear, fluid-filled blisters on the dorsal aspect of her toes on both feet. The patient had no fever, chills, pain, or itching. There were no recent changes to any medications and she’d had no prolonged exposure to the sun. The patient was initially hospitalized out of concern for cellulitis, but discharged the next day with no change in status or treatment. She returned to the ED several days later with the bullae still intact.
What's your diagnosis?
A biopsy was performed and direct immunofluorescence came back negative. This, along with the patient’s history of diabetes, led us to diagnose bullosis diabeticorum.
This condition, also known as bullous disease of diabetes, is characterized by abrupt development of noninflammatory bullae on acral areas in patients with diabetes. The skin appears normal except for the bullae. Bullosis diabeticorum occurs in just .5% of patients with diabetes and is twice as common in men as it is in women.
The etiology of bullosis diabeticorum is unknown. The acral location suggests that trauma may be a contributing factor. Although electron microscopy has suggested an abnormality in anchoring fibrils, this cellular change does not fully explain the development of multiple blisters at varying sites. Glycemic control is not thought to play a role.
The distribution of lesions and the presence—or absence—of systemic symptoms goes a long way toward narrowing the differential of blistering diseases. The presence of generalized blistering and systemic symptoms would suggest conditions related to medication exposure, such as Stevens-Johnson syndrome or toxic epidermal necrolysis; infectious etiologies (eg, staphylococcal scalded skin syndrome); autoimmune causes; or underlying malignancy. Generalized blistering in the absence of systemic symptoms would support diagnoses such as bullous impetigo and pemphigoid.
Lesion distribution provides important clues, too. Sun exposure-related causes typically leave lesions on the hands and forearms, not just the toes. A dermatomal distribution would suggest herpes zoster. A linear distribution of blisters argues for contact dermatitis.
A diagnosis of bullosis diabeticorum can be made when biopsy with immunofluorescence excludes other histologically similar entities such as epidermolysis bullosa, noninflammatory bullous pemphigoid, and porphyria cutanea tarda. And while immunofluorescence findings are typically negative, elevated levels of immunoglobulin M and C3 have, on occasion, been reported. Cultures are warranted only if a secondary infection is suspected.
The bullae of this condition spontaneously resolve over several weeks without treatment, but tend to recur. The lesions typically heal without significant scarring, although they may have a darker pigmentation after the first occurrence. Treatment may be warranted if a patient develops a secondary infection.
In our patient’s case, the bullae resolved within 2 weeks without treatment, although mild hyperpigmentation remained.
Adapted from: Mims L, Savage A, Chessman A. Blisters on an elderly woman's toes. J Fam Pract. 2014;63:273-274.