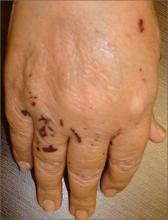
Purpuric lesions on extremities
A 68-year-old woman sought care for pruritic purpuric skin lesions on her trunk and extremities that she’d had for 5 days. She also had a few nonblanching, erythematous macules on her extremities. The patient, who was given a diagnosis of asthma 3 years earlier, had recently lost weight without trying. She also complained of malaise.
What's your diagnosis?
This patient was given a diagnosis of Churg-Strauss syndrome. A CSS diagnosis can be made if 4 of the following 6 criteria are met: (1) asthma, (2) eosinophilia >10% on a differential white blood cell count (WBC), (3) paranasal sinus abnormalities, (4) a transient pulmonary infiltrate detected on chest x-ray, (5) mono- or polyneuropathy, and (6) a biopsy specimen showing extravascular accumulation of eosinophils.
This patient met 4 of the 6 criteria. She had asthma and a punch biopsy showed leukocytoclastic vasculitis with prominent tissue eosinophilia. Lab studies showed an elevated WBC of 12,300/mcL and eosinophilia of 40%. A serologic test for perinuclear pattern antineutrophil cytoplasmic antibodies (p-ANCA) was positive. Radiography of the chest showed transient pulmonary infiltrates.
CSS—also known as allergic granulomatosis and angiitis—is a rare multisystemic vasculitis of small- to medium-sized vessels characterized by asthma, chronic rhinosinusitis, and prominent peripheral blood eosinophilia. The mean diagnosis age is 50 years and any organ system can be affected, although the lungs and skin are most commonly involved.
Three distinct phases of CSS have been described. The first is the prodromal or allergic phase, which is characterized by the onset of asthma later in life in patients with no family history of atopy. The eosinophilic phase is characterized by peripheral blood eosinophilia and eosinophilic infiltration of multiple organs. The vasculitis phase is characterized by life-threatening systemic vasculitis of the small and medium vessels that is often associated with vascular and extravascular granulomatosis. One-half to two-thirds of patients with CSS have cutaneous manifestations that typically present in the vasculitis phase.
Systemic corticosteroids (prednisone, 1 mg/kg/day) are the primary treatment for patients with CSS; most patients improve dramatically with therapy. Adjunctive therapy with immunosuppressive agents such as cyclophosphamide, methotrexate (10-15 mg per week), chlorambucil, or azathioprine may be needed if a patient does not respond adequately to steroids alone.
In this case, the patient was prescribed prednisone 1 mg/kg/d. Her skin lesions resolved and subsequent laboratory tests normalized, including her eosinophil counts. Prednisone therapy was gradually tapered over several months to attain the lowest dose required for control of symptoms—in this case, 5 mg/d.
Adapted from: Abadi R, Dakik H, Abbas O. Purpuric lesions in an elderly woman. J Fam Pract. 2014;63:159-161.