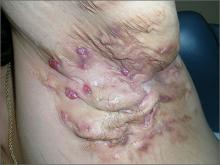
Painful lesions in axillae
A 43-year-old woman sought care for painful lesions in both axillae that she’d had for the past 10 years. Her previous physicians had given her oral antibiotics that provided little relief, and when she went to the emergency department or an urgent care center, the doctors often cut her skin to let the pus out. She said that this hurt and didn’t improve things.
What's your diagnosis?
The family physician (FP) diagnosed hidradenitis suppurativa, a disorder of the terminal follicular epithelium in the apocrine gland-bearing skin. Hidradenitis suppurativa causes chronic relapsing inflammation with mucopurulent discharge. As seen in this case, it can also lead to sinus tracts, draining fistulas, and progressive scarring, as well as disabling pain and social isolation.
Hidradenitis suppurativa is also called acne inversa because it involves intertriginous areas and not the regions affected by acne (face and back). Patients typically complain of painful, tender, firm, nodular lesions in the axillae. Both obesity and smoking make the condition worse.
The patient was desperate for relief from this condition. The FP explained exacerbating factors and treatment options. The patient acknowledged that she needed to quit smoking and lose weight, but found it painful to move her arms because of the lesions in both axillae. She set a smoking quit date for 2 weeks in the future and planned to quit without any pharmacologic intervention. The physician suggested that she start exercising by walking, especially since she did not have any of the hidradenitis in the inguinal or buttocks region. Diet control was also briefly discussed.
The patient chose to have intralesional steroid injections for the 3 most painful nodules. The FP injected the nodules with triamcinolone 10 mg/mL and started the patient on doxycycline 100 mg bid for one month. Injections are less painful than incision and drainage and usually work better (unless there is a huge abscess).
The FP also explained that the Food and Drug Administration had approved the first drug specifically for hidradenitis, called adalimumab (Humira), which has been used for years for psoriasis and various other inflammatory conditions, including rheumatoid arthritis. While he was not comfortable prescribing this injectable biologic medication, he offered the patient a referral to Dermatology. The patient gladly accepted this and was happy to know that there was some hope for her condition.
Unfortunately, adalimumab does not cure hidradenitis and will not reverse the damage that’s been done. It can, however, provide symptomatic relief and minimize the number of future flare-ups. Surgery is another option, but it is major surgery that involves a long, painful healing time that brings with it the risk of complications. Surgery is also not curative, as the hidradenitis may reappear in the skin that was not resected.
Photos and text for Photo Rounds Friday courtesy of Richard P. Usatine, MD. This case was adapted from: Usatine R. Hidradenitis suppurativa. In: Usatine R, Smith M, Mayeaux EJ, et al, eds. Color Atlas of Family Medicine. 2nd ed. New York, NY: McGraw-Hill; 2013:671-675.
To learn more about the Color Atlas of Family Medicine, see: www.amazon.com/Color-Family-Medicine-Richard-Usatine/dp/0071769641/
You can now get the second edition of the Color Atlas of Family Medicine as an app by clicking on this link: usatinemedia.com