When and how to evaluate mildly elevated liver enzymes in apparently healthy patients
ABSTRACTBecause 1% to 9% of people without symptoms have elevated liver enzymes, extensive evaluation of all abnormal test results would expose many patients to undue risks and expenses. On the other hand, failure to evaluate minor liver enzyme elevations could mean missing the early diagnosis of potentially treatable disorders. This review discusses likely causes of elevated aminotransferase, alkaline phosphatase, and gamma-glutamyl transferase levels and provides algorithms for evaluating high liver enzyme values in apparently healthy patients in the primary care setting.
KEY POINTS
- Nonalcoholic fatty liver disease is the most common cause of asymptomatic elevated aminotransferase levels.
- Suspect alcoholic liver disease when the aminotransferases are elevated and the aspartate aminotransferase level is two to three times higher than the alanine aminotransferase level, especially when gamma-glutamyl transferase levels are elevated.
- If medications or alcohol is a suspected cause of elevated aminotransferase levels, remeasure the levels after 6 to 8 weeks of abstinence.
Studies of mild aminotransferase elevations
Only a few studies have documented the results of a thorough evaluation of patients with mildly elevated aminotransferase levels:
Hultcrantz et al1 performed a full evaluation, including liver biopsy, in 149 consecutive patients with chronic, asymptomatic, mild elevations of AST or ALT. Of these patients, 63% had “fatty liver,” 20% had “chronic hepatitis,” and 17% had miscellaneous diagnoses. Whether patients in the “chronic hepatitis” group had hepatitis C was not determined because serologic testing was not available at the time.
Friedman et al16 studied 100 healthy blood donors with elevated ALT levels and found that in 33% of patients the elevation occurred once, in 36% it was intermittent, and in 28% it was persistent. In this series, 45% of patients had no diagnosis, 22% were obese (presumed to have nonalcoholic steatohepatitis), 5% had alcoholic liver disease, 3% had “resolving hepatitis,” 1% had hemochromatosis, and 1% had “cytomegalovirus hepatitis.”16 Although the patients underwent a complete history, physical examination, and serologic testing, liver biopsy was not done to confirm the clinical diagnosis.
Hay et al17 described 47 patients with chronically elevated aminotransferases (three to eight times higher than normal levels) who underwent full evaluation and liver biopsy and who had no clinical symptoms of alcoholic, viral, or drug-induced liver disease. A diagnosis of steatohepatitis was given in 10 patients, another 34 were diagnosed with “chronic hepatitis,” and 3 had miscellaneous diagnoses. Of patients with chronic hepatitis, 16 had evidence of cirrhosis on biopsy, and 18 tested positive for at least one autoimmune marker (antinuclear antibody or smooth muscle antibody).
Daniel et al18 performed biopsy in 81 of 1,124 asymptomatic and symptomatic patients with chronically elevated aminotransferases in whom a cause was not identified via noninvasive studies. Liver biopsy showed that 67 (83%) of the 81 patients had steatosis or steatohepatitis, while 8 (10%) had normal histologic findings. Of note, 6 patients had underlying fibrosis or cirrhosis and some degree of fatty infiltration.
Together, these studies suggest that fatty liver, resulting either from alcohol use or from nonalcoholic fatty liver disease, is the major cause of mildly elevated aminotransferases. Two major drawbacks of the earlier studies include the lack of data on the hepatitis C serologic status of patients with the diagnosis of “chronic hepatitis” and the lack of a uniform approach to the pathologic diagnosis of nonalcoholic steatohepatitis. With serologic testing for hepatitis C virus infection now widely available, it is possible that a substantial portion of patients with “chronic hepatitis“ can further be classified as having chronic hepatitis C infection.
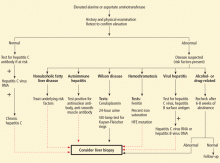
Workup of aminotransferase elevations
- Viral hepatitis (intravenous drug use, intranasal cocaine use, native of an endemic area of the world, unsafe sexual activity, blood product transfusions)
- Nonalcoholic fatty liver disease (components of the metabolic syndrome, including visceral obesity)
- Alcoholic liver disease (smaller amounts are needed to cause liver disease in women)
- Medication exposure (prescription, overthe-counter, and herbal medications)
- Genetic liver disorders (family history of liver disease)
- Possible coexisting disease (diabetes and obesity in nonalcoholic steatohepatitis, neurologic disorders in Wilson disease, emphysema in alpha-1-antitrypsin deficiency, thyroid disease in autoimmune hepatitis and primary biliary cirrhosis, and diabetes and impotence in genetic hemochromatosis).
Although the physical signs of chronic liver disease (eg, spider angiomata, palmar erythema, caput medusae, and gynecomastia) are nonspecific and are usually observed in advanced liver disease, some physical findings suggest potential causes (eg, Kayser-Fleischer rings on slit-lamp examination for Wilson disease, hypertrophy of the second and third metacarpophalangeal joints for hemochromatosis). Iron studies for middleaged men, autoimmune markers for women, and screening for Wilson disease in young patients are helpful when the clinical information points to one of these entities as a potential diagnosis.
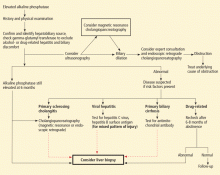
If medication or alcohol is a suspected cause, aminotransferase levels should be repeated after 6 to 8 weeks of abstinence. If nonalcoholic steatohepatitis is suspected, testing should be repeated after treating the potential risk factor (eg, obesity, diabetes, hyperlipidemia), but the levels may remain elevated for a period of time. An imaging study (ultrasonography, computed tomography, or magnetic resonance imaging) may be helpful; eg, abdominal ultrasonography may show increased hepatic echogenicity, suggesting increased fatty infiltration, in addition to excluding most hepatic tumors.
If the history and physical do not suggest a specific condition, serologic testing for hepatitis C should be done. If negative, other testing can be helpful (iron studies in men, autoimmune markers in women, ceruloplasmin and slit-lamp examination in young patients). If the preliminary workup remains negative and the aminotransferase levels remain elevated for 6 months (ie, chronic elevation), liver biopsy may establish the diagnosis. Features in the biopsy specimens may further confirm the diagnosis: eg, globules positive on periodic acid-Schiff testing in alpha-1-antitrypsin deficiency; hepatic iron index for hemochromatosis; hepatic copper content for Wilson disease.