Managing osteoporosis: Challenges and strategies
ABSTRACTMany patients at high risk of fracture are not being identified and treated, and many of those who start treatment do not take it correctly or long enough to lower their risk. This paper is a review of unmet needs in the management of osteoporosis and strategies to improve clinical outcomes.
KEY POINTS
- Osteoporosis is underdiagnosed. Patients discharged from the hospital after hip fractures are commonly not diagnosed with or treated for osteoporosis although the risk of future fractures is very high.
- The Fracture Risk Assessment Tool (FRAX) estimates the 10-year probability of fracture on the basis of clinical risk factors for fracture and the bone mineral density of the femoral neck. The combination of bone mineral density and clinical risk factors predicts fracture risk better than either alone.
- A drug holiday, for 1 year or perhaps longer, may be considered for patients on alendronate (Fosamax) who are no longer at high risk of fracture. On the other hand, given the evidence of increased risk of clinical vertebral fracture and hip fracture after bisphosphonates are discontinued, a drug holiday is probably not a reasonable choice in patients at high risk of fracture.
- Patient education and regular contact with a health care provider may improve compliance and persistence with therapy.
Economic assumptions behind the guidelines
The National Osteoporosis Foundation based its recommendations on cost-effectiveness modeling39 and the US version of FRAX.40 The fracture risk algorithm was calibrated to US fracture and death rates, with economic assumptions that included the following: 5 years of drug therapy with 100% compliance and persistent use of a drug that costs $600 per year and results in a 35% reduction in fracture risk, followed by discontinuation of the drug associated with a linear offset of effect over the next 5 years, with a societal willingness to pay up to $60,000 per quality-adjusted life-year gained.39
FRAX is used to decide on treatment only in those with osteopenia
FRAX is used for making treatment decisions only in patients with osteopenia. Those with a densitometric diagnosis of osteoporosis according to a T-score value of −2.5 or less or a clinical diagnosis of osteoporosis by virtue of having had a fracture of the hip or spine should be treated regardless of FRAX, and those with normal T-scores are not recommended for treatment regardless of FRAX. By providing a quantitative estimation of fracture probability, FRAX allows clinicians to distinguish patients with osteopenia who are at high fracture risk from those who are not, and thereby to treat those most likely to benefit.
Since approximately one-half of patients who have fragility fractures do not have T-scores in the osteoporosis range,41,42 there is great clinical utility in identifying the subset of osteopenic patients who are candidates for treatment. It is likely that the use of FRAX will result in fewer early postmenopausal women and more older women with osteopenia being treated with drugs, since age is an important risk factor for fracture that is independent of bone mineral density.
Which drugs to use?
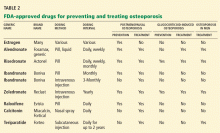
The drugs currently approved in the United States for preventing and treating osteoporosis are:
- Alendronate (Fosamax)
- Risedronate (Actonel)
- Ibandronate (Boniva)
- Zoledronate (Reclast)
- Salmon calcitonin (Miacalcin, Fortical)
- Raloxifene (Evista)
- Teriparatide (Forteo) (Table 2).
It is not known with certainty whether any of these drugs is more effective than any other, because no head-to-head clinical trials have been done using fracture as the primary end point.
Selecting a drug requires assessing its benefits and risks for each patient. The National Osteoporosis Foundation’s intervention thresholds do not consider nonskeletal benefits and risks, such as reduction in the risk of invasive breast cancer and increase in the risk of thromboembolic events with raloxifene.
For patients on glucocorticoids
Chronic glucocorticoid therapy is a special category of fracture risk. Rapid bone loss can occur at the start of therapy43 and the adverse effects on bone strength are at least partially independent of bone mineral density.44 US Food and Drug Administration indications for drugs for prevention and treatment of glucocorticoid-induced osteoporosis are distinct from those for postmenopausal osteoporosis and osteoporosis in men (Table 2). Since FRAX may underestimate the fracture risk in some patients on glucocorticoid therapy, the National Osteoporosis Foundation recommendations may leave out some patients who could benefit from therapy.
The American College of Rheumatology recommends prescribing a bisphosphonate (with caution in premenopausal women) for patients beginning therapy with prednisone 5 mg per day or higher (or its equivalent) if the corticosteroid therapy is planned to continue for 3 months or longer, and for patients who have been receiving this dose long-term who have low bone mineral density (T-score < −1.0).45
STRATEGIES FOR IMPROVING TREATMENT
Look for causes of secondary osteoporosis
All patients with osteoporosis should undergo an evaluation for factors other than postmenopausal status or aging that may adversely affect skeletal health or the choice of treatment. Causes of secondary osteoporosis are common,46 occurring in about two-thirds of men and about one-fifth of postmenopausal women,47 and unless they are recognized and treated, they may block or attenuate the response to therapy.
Particular attention must be paid to the adequacy of calcium and vitamin D intake and absorption. While there is no standard laboratory evaluation, one study suggests that cost-effective testing in a referral practice includes measurement of serum calcium, serum 25-hydroxyvitamin D, serum parathyroid hormone, 24-hour urinary calcium, and thyroidstimulating hormone if on thyroid replacement in all women with osteoporosis.48,49
Other helpful tests are a complete blood count, alkaline phosphatase, serum creatinine, serum phosphorus, serum protein electrophoresis in elderly patients, and serum testosterone in men; additional evaluation may be indicated, depending on clinical circumstances.
Think about special indications for or contraindications to specific drugs
If you have determined that drug therapy is indicated to reduce fracture risk, then a particular drug must be selected that is likely to be effective, safe, and affordable for the individual patient. Consideration must be given to what is known about the skeletal and non-skeletal benefits and risks, as well as patient factors such as other medical conditions, past drug experiences, and beliefs. For example:
- An oral bisphosphonate should not be given to a patient with a history of esophageal stricture, but an intravenous bisphosphonate may be very helpful.
- Raloxifene may be attractive for a patient at high risk of invasive breast cancer but not if there is a history of thromboembolic disease.
- Generic alendronate may be the first choice for a patient whose primary concern is keeping cost to a minimum, but risedronate or ibandronate may be best for a patient who prefers the convenience of monthly oral dosing.