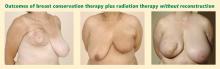
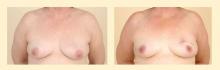
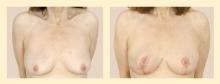
Reconstruction options following breast conservation therapy
ABSTRACT
Women who have had breast conservation therapy for malignancy are candidates for various surgical techniques for immediate or delayed breast reconstruction. These include local tissue rearrangement, therapeutic reduction mammaplasty, and various flap reconstruction procedures. Each technique has advantages and disadvantages, and individual patient factors, particularly breast size and resection defect size, should drive the choice among procedures. Immediate reconstruction (at the time of breast conservation surgery) is preferred over delayed reconstruction, for multiple reasons. Patients tend to be satisfied with the cosmetic outcome of these procedures, but thorough patient counseling and preop-immediate or erative planning is critical to a good result.
Oncoplastic surgery refers to immediate or delayed breast reconstruction following partial mastectomy, also known as breast conservation therapy. The term was coined by Audretsch et al in 19981 and is now often referred to as oncoplasty. It involves four integral components:2
- Oncologically sound techniques of tumor removal
- Partial reconstruction of the breast to correct small defects
- Immediate reconstruction for larger defects using various principles of plastic surgery
- Creation of symmetry with the contralateral breast.
This article provides a brief overview of various procedures used for reconstruction following breast conservation therapy and the factors that guide selection among these procedures for individual patients. It concludes with a discussion of complications of oncoplastic procedures, patient counseling, and other general considerations in patient management.
THE RATIONALE FOR RECONSTRUCTION
Effects of radiation argue for immediate reconstruction
Although radiation therapy is integral to the comprehensive treatment of breast cancer after breast conservation therapy, radiation-induced changes to the breast are one of the greatest obstacles faced when delayed reconstruction is performed. Radiation results in deformation of the parenchyma, leading to retraction, fibrosis, vasculitis, and skin breakdown. The effects of radiation on breast tissue may possibly be a larger problem when reconstruction is delayed, as wound healing is inhibited and vascular supply is impaired. Therefore, immediate reconstruction should be undertaken whenever possible.7 (The timing of reconstruction is discussed in greater detail in the final article in this supplement, although mainly in the context of mastectomy.)
OPTIONS FOR RECONSTRUCTION
Various techniques of partial breast reconstruction can be used to achieve an aesthetically acceptable result. They can be thought of as volume-displacement procedures, such as local tissue rearrangement and reduction mammaplasty, or as volume-replacement procedures using flap reconstruction.8 Additionally, simple wound closure (primary closure) may be performed if small amounts of tissue can be removed without creating a noticeable defect, but simple closure is an option only for large breasts. The decision among techniques depends on a variety of factors, as delineated below.
Local tissue rearrangement
Local tissue rearrangement is defined as the use of local tissue (skin and subcutaneous and/or breast tissue) from either the breast or the axilla. This technique involves the transfer of adjacent breast parenchyma and skin to the area of the defect. It is dependent on a random blood supply and does not involve creating a parenchymal tissue pedicle.4,5 It does rely, however, on a balance between the amount of tissue resected and the available residual breast size and volume. This procedure is not suitable for patients who require large-volume resection with a small breast or limited breast tissue.
When local tissue rearrangement is to be performed, the surgical incision needs to be planned by both the oncologic surgeon and the plastic surgeon to ensure an appropriate cosmetic outcome and prevent displacement or distortion of the nipple-areola complex. If such planning is not done, the cosmetic outcome may be compromised, thereby undermining one of the reasons for breast conservation in the first place. When full-thickness excisions of tissue are removed from a certain area of the breast—termed “no man’s land” by Grisotti and Calabrese7—the nipple-areola complex shifts to an unnatural position. Therefore, resections in this area, located superiomedial to the nipple, should include little or no skin.
Other techniques of tissue transposition include circumareolar incisions for tumors located adjacent to the nipple-areola complex, radially designed resections for lateral tumors, and donut-shaped resections for superior or lateral tumors.8
Reduction mammaplasty
Standard breast reduction techniques are used on the contralateral (uninvolved) breast. This matching procedure can be performed at the same time as the initial cancer operation or as a delayed procedure. The matching procedure is usually performed at a later date for those who need to undergo radiation therapy, allowing time for healing and for final breast volume and shape to be achieved. Reduction of the contralateral breast does not increase its risk for cancer; in fact, reduction may improve body image and make breast self-examinations and follow-up mammography easier.
Therapeutic reduction mammaplasty is highly versatile and gives a better aesthetic result in the immediate setting when compared with flap reconstruction. However, it is usually limited to patients with a brassiere cup size of D or larger.4
An advantage of reduction mammaplasty is that reducing the size of the affected breast facilitates postoperative radiation therapy. Some radiation oncologists are reluctant to administer radiation to a large breast because of increased toxicity to the skin and the likelihood of a poor aesthetic outcome. With reduction mammaplasty, lower radiation doses are required and the delivery of radiation is more uniform.4
Reduction mammaplasty is ideal for women with moderate-sized or large breasts with ptosis (sagging), for whom a reduction in size would be considered a positive outcome.10 Patients with symptomatic macromastia likewise benefit from reduction in breast volume. An additional advantage is that the reduction procedure on the contralateral breast affords the opportunity for tissue sampling from this presumedly uninvolved breast; occult carcinomas in the contralateral breast have been identified in a small percentage of patients.11
At the same time, the exposure of the contralateral breast to surgery also constitutes the main disadvantage of this procedure, as both breasts are placed at risk for wound or nipple complications and the discomfort of surgery.9 Moreover, surgery time is also increased. Lastly, reduction mammaplasty can be offered only to patients who possess enough breast tissue to undergo reduction.12