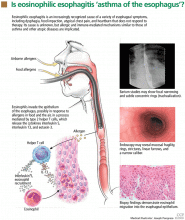
Eosinophilic esophagitis: An increasingly recognized cause of dysphagia, food impaction, and refractory heartburn
ABSTRACTEosinophilic esophagitis is an increasingly recognized cause of a variety of esophageal symptoms, including dysphagia, food impaction, atypical chest pain, and heartburn that does not respond to medical therapy. Its cause is unknown, but allergic and immunemediated mechanisms similar to those of asthma and other atopic diseases are implicated.
KEY POINTS
- The diagnosis is made with upper endoscopy and esophageal biopsies that show diffuse infiltration of eosinophils.
- Current treatment in adults is limited and consists of either swallowed fluticasone (Flonase) or a proton pump inhibitor.
- Because many patients with eosinophilic esophagitis have atopic disease, a complete evaluation for dietary allergens and aeroallergens is recommended, as avoidance of these allergens may be helpful in some adults.
- Cautious endoscopic dilation is a treatment option in patients with evidence of esophageal stenosis. Systemic corticosteroids and novel biologic therapy have been used in refractory cases.
Abundant eosinophils in the esophagus were first described in 1977 in a 51-year-old man with dysphagia, chest pain, and a personal history of severe asthma and marked peripheral eosinophilia.1 In 1983, a similar case was reported in an adolescent with dysphagia.2 In both patients, large numbers of eosinophils were also noted in the duodenum, suggesting that these findings were part of a systemic hypereosinophilic syndrome.
Increased numbers of eosinophils in the gastrointestinal tract have been described in a number of diseases, including Crohn disease, connective tissue disorders, malignancy, various infections, and drug hypersensitivity reactions. However, not until 1993 was eosinophilic esophagitis described as a distinct clinical entity, consisting of isolated esophageal eosinophilia (typically more than 15 eosinophils per high-power field) in patients with dysphagia.3
Now, epidemiologic studies suggest that eosinophilic esophagitis may be as common as inflammatory bowel disease. In a study of children in Cincinnati, OH,4 the incidence was estimated at 10 per 100,000 children per year and the prevalence was estimated at 43 per 100,000. Of interest, 97% of cases were diagnosed after the year 2000.
RISING INCIDENCE, OR INCREASED RECOGNITION?
Over the last several years, the number of reported cases has increased substantially as interest in this disease has grown. The increase has been attributed in part to heightened awareness of this condition among clinicians and, hence, more esophageal biopsies being performed. Similarly, pathologists may have previously attributed esophageal eosinophilia to gastroesophageal reflux disease (GERD). However, the prevalence of eosinophilic esophagitis increased 10-fold between 1989 and 2003 in a fixed and stable adult population in Olten, Switzerland, suggesting that more than just increased awareness is responsible for this dramatic rise.5
PATHOGENESIS: SIMILAR TO OTHER ALLERGIC DISEASES?
The growing incidence of eosinophilic esophagitis parallels that of asthma, eczema, allergic rhinitis, and other atopic diseases, raising the possibility that these disorders share common environmental exposures and similar inflammatory pathways.6 The pathologic mechanisms of eosinophilic esophagitis are unknown, but emerging evidence suggests that, like other allergic diseases, it is an immune response mediated by type 2 T helper cells.
Several animal studies support this hypothesis. Mice sensitized and then exposed to aeroallergens developed both allergic airway inflammation and eosinophilic esophagitis. Interleukin 5, a cytokine involved in asthma, also helps recruit eosinophils into the esophagus, as transgenic mice deficient in interleukin 5 do not develop esophageal eosinophilia upon allergen exposure.7
Recently, eotaxin-3, a potent attractant for eosinophils, was shown to be markedly overexpressed in children with eosinophilic esophagitis compared with controls.8
Acid reflux does not appear to be a causative factor in most patients. However, reflux may play a secondary role, as some patients have experienced symptomatic, endoscopic, and histologic resolution of eosinophilic esophagitis after treatment with a proton pump inhibitor.9
GERD AND EOSINOPHILIC ESOPHAGITIS: WHAT IS THE RELATIONSHIP?
Given the high prevalence of GERD in the general population, much time and effort have been spent on comparing eosinophilic esophagitis with GERD. In fact, some endoscopic features typically seen in eosinophilic esophagitis were previously attributed to acid reflux.10
Both diseases share varying degrees of esophageal eosinophilia, and some have speculated on the relationship of eosinophilic esophagitis and GERD. Spechler et al11 recently suggested that the mucosal injury caused by acid reflux may allow swallowed allergens to penetrate an esophageal layer that is otherwise impermeable to most proteins, thereby causing mild eosinophilia. Conversely, the intense degranulation of activated eosinophils seen in eosinophilic esophagitis can trigger changes in the lower esophageal sphincter that could predispose to acid reflux.
Although their clinical and pathologic features may overlap, GERD and eosinophilic esophagitis appear to have different genetic profiles. In a recent pediatric study, Blanchard et al8 found that genes up-regulated in eosinophilic esophagitis were markedly different than those in chronic esophagitis. This suggests that while the two diseases share a constellation of symptoms, they have a different pathogenesis. Nevertheless, because of this possible overlap, the diagnosis of eosinophilic esophagitis should be made after acid reflux has been either treated or excluded with pH testing (see below).